Surface and Radiological Anatomy — MCQs

On this page
What is true regarding the surface anatomy of the internal jugular vein?
What is the approximate distance of the gastroesophageal junction from the upper incisors?
Which of the following represents the surface marking of the aortic valve?
Which of the following does not contribute to the hilar shadow?
Which anatomical landmark represents the surface projection of the internal jugular vein?
What is the approximate size of the optic disc in millimeters?
Which spinal segment supplies the umbilicus?
Which organ does not move with respiration?
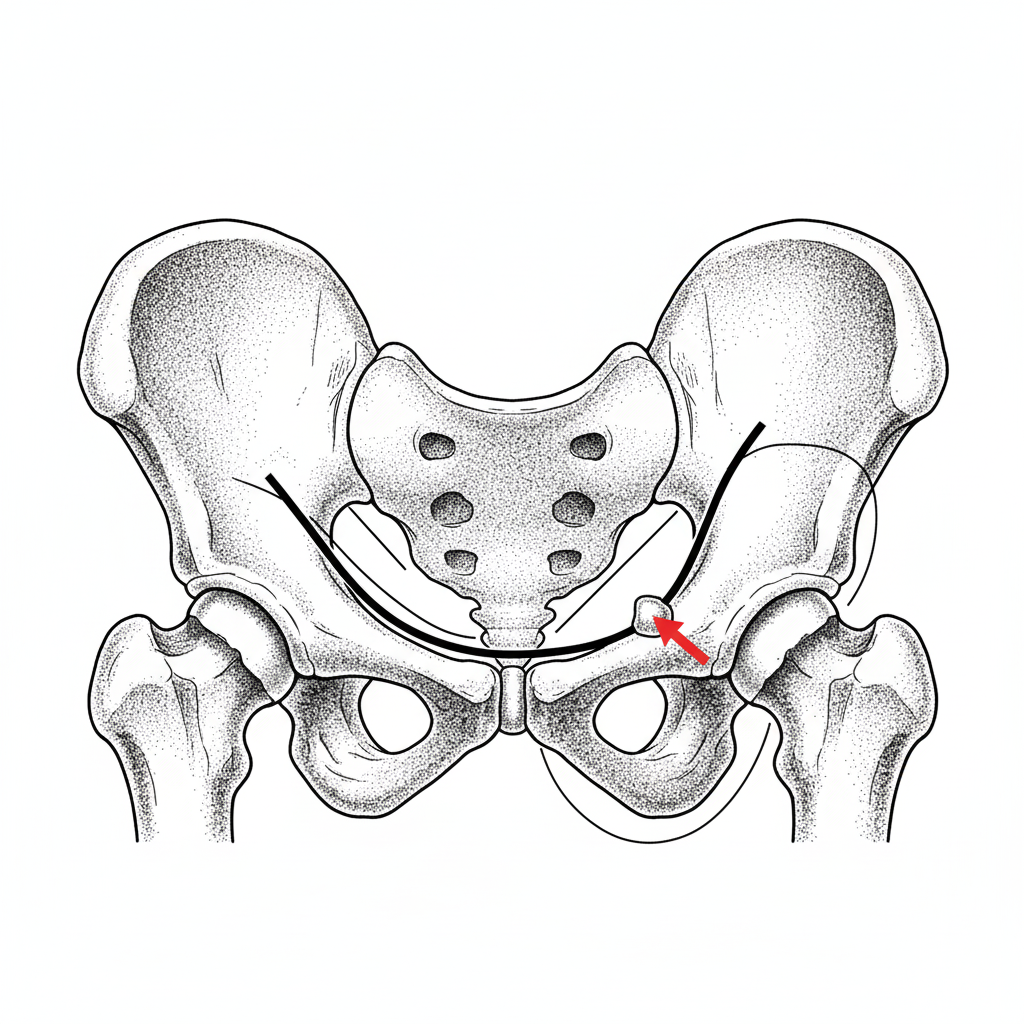
Shenton's line is:
The bony landmark shown in the diagram is used to differentiate between inguinal and femoral hernias. What is this landmark?
Practice by Chapter
Surface Landmarks of the Head and Neck
Practice Questions
Surface Landmarks of the Thorax
Practice Questions
Surface Landmarks of the Abdomen
Practice Questions
Surface Landmarks of the Limbs
Practice Questions
Radiographic Anatomy
Practice Questions
CT Anatomy
Practice Questions
MRI Anatomy
Practice Questions
Ultrasonographic Anatomy
Practice Questions
Angiographic Anatomy
Practice Questions
Sectional and Cross-sectional Anatomy
Practice Questions
Anatomical Correlations in Common Imaging
Practice Questions
Interventional Radiological Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
