Pelvis and Perineum — MCQs

On this page
The blood supply of uterus is from: 1. Uterine artery 2. Ovarian artery 3. Pudendal artery 4. Superior vesical artery Select the correct answer using the code given below:
The following are the contents of broad ligament EXCEPT:
Which one of the following is NOT a support of uterus, preventing its descent?
What is the volume of the prostate in normal adult males?
What can cause the absence of fructose in seminal fluid?
Identify the pelvic diaphragm in the picture given below:
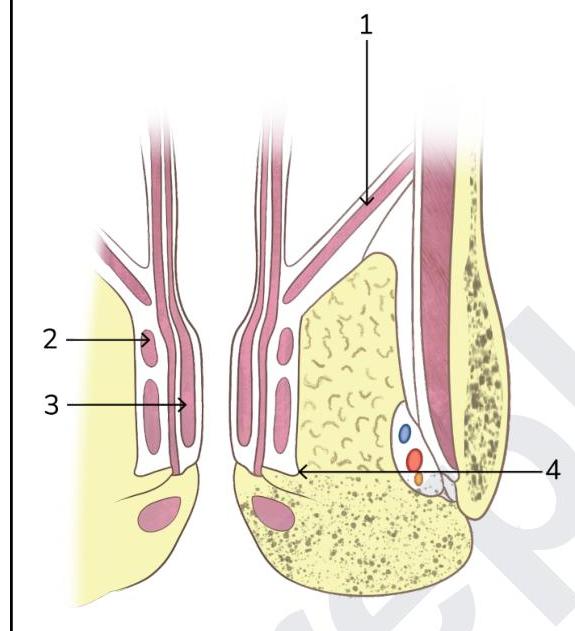
Bleeding vessel in hemorrhoids is
Among the following the plane of least pelvic dimension is:
Injury to which of the following muscles that forms the deep support of the perineal body causes cystocele, enterocele and urethral descent?
Vaginal sphincter is formed by all except
Practice by Chapter
Pelvic Walls and Floor
Practice Questions
Pelvic Viscera
Practice Questions
Urogenital Organs
Practice Questions
Pelvic Vasculature
Practice Questions
Pelvic Innervation
Practice Questions
Male Perineum
Practice Questions
Female Perineum
Practice Questions
Pelvic Lymphatics
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Gender Differences in Pelvic Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
