Pelvis and Perineum — MCQs

On this page
How can a female pelvis be differentiated from a male pelvis?
In a study, it is observed that the right ovary ovulates more frequently than the left. Which of the following is NOT a possible explanation for this observation?
All of the following statements regarding the vas deferens are true, EXCEPT?
Which of the following statements about the ovary is correct?
The opening in the prostatic sinus is related to which structure?
Before puberty, what is the ratio between the cervical length and uterine body length?
A 49-year-old woman has a large mass on the pelvic brim. Which of the following structures is most likely compressed by this mass when crossing the pelvic brim?
Which of the following is NOT true about the lobes of the prostate?
Which structure secretes fluid containing fructose, which allows for forensic determination of rape?
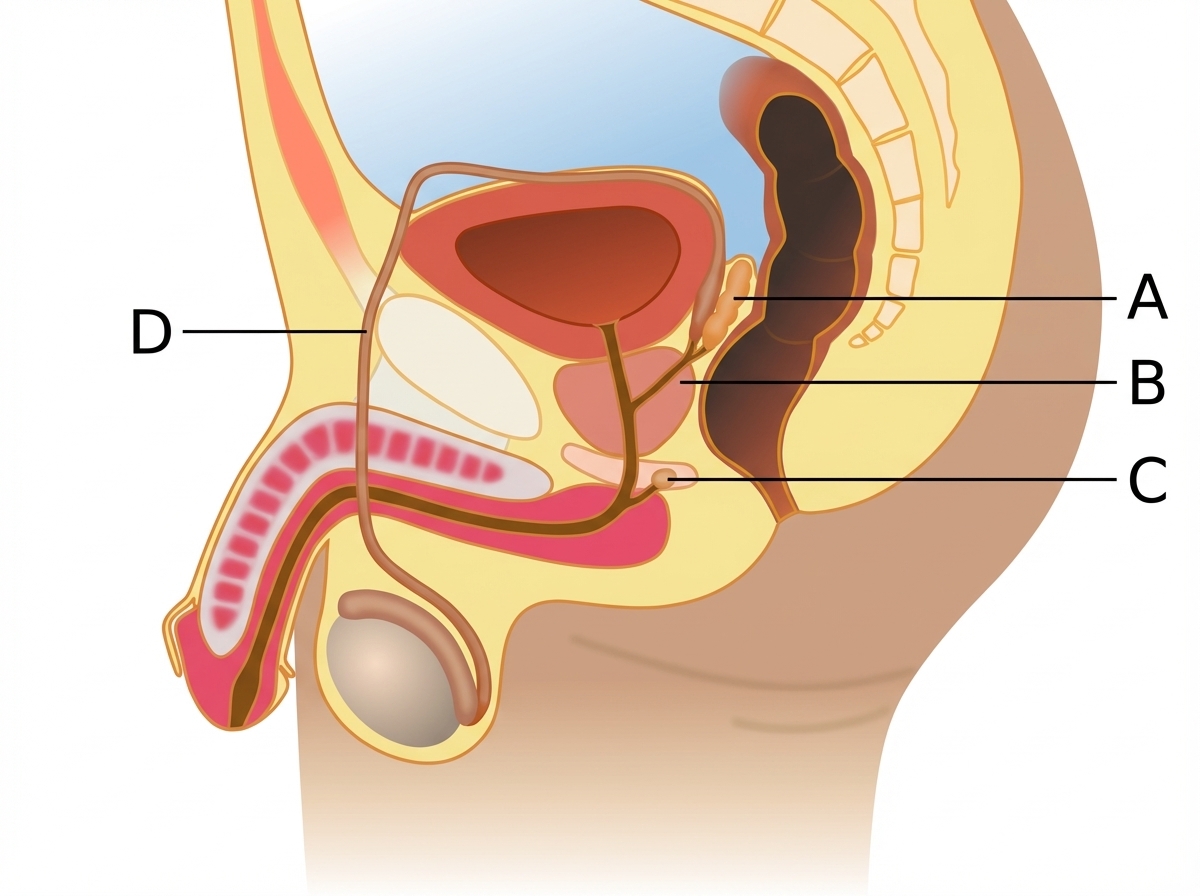
Which muscle does not constitute the pelvic diaphragm?
Practice by Chapter
Pelvic Walls and Floor
Practice Questions
Pelvic Viscera
Practice Questions
Urogenital Organs
Practice Questions
Pelvic Vasculature
Practice Questions
Pelvic Innervation
Practice Questions
Male Perineum
Practice Questions
Female Perineum
Practice Questions
Pelvic Lymphatics
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Gender Differences in Pelvic Anatomy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
