Neck — MCQs

On this page
The spinal part of the accessory nerve supplies which of the following muscles?
The common carotid artery divides at the level of which anatomical landmark?
A 31-year-old man sustained a shrapnel wound in the neck. On examination, it was noticed that when he blew his nose or sneezed, the skin above the right clavicle bulged upward. Which of the following best explains this phenomenon?
What is the narrowest part of the pediatric airway?
Which of the following group of lymph nodes are known as 'delphic nodes'?
The submental triangle is bounded laterally on both sides by which muscle?
The recurrent laryngeal nerve has a close anatomical relationship with which of the following structures?
The danger space in front of the prevertebral fascia extends till which anatomical landmark?
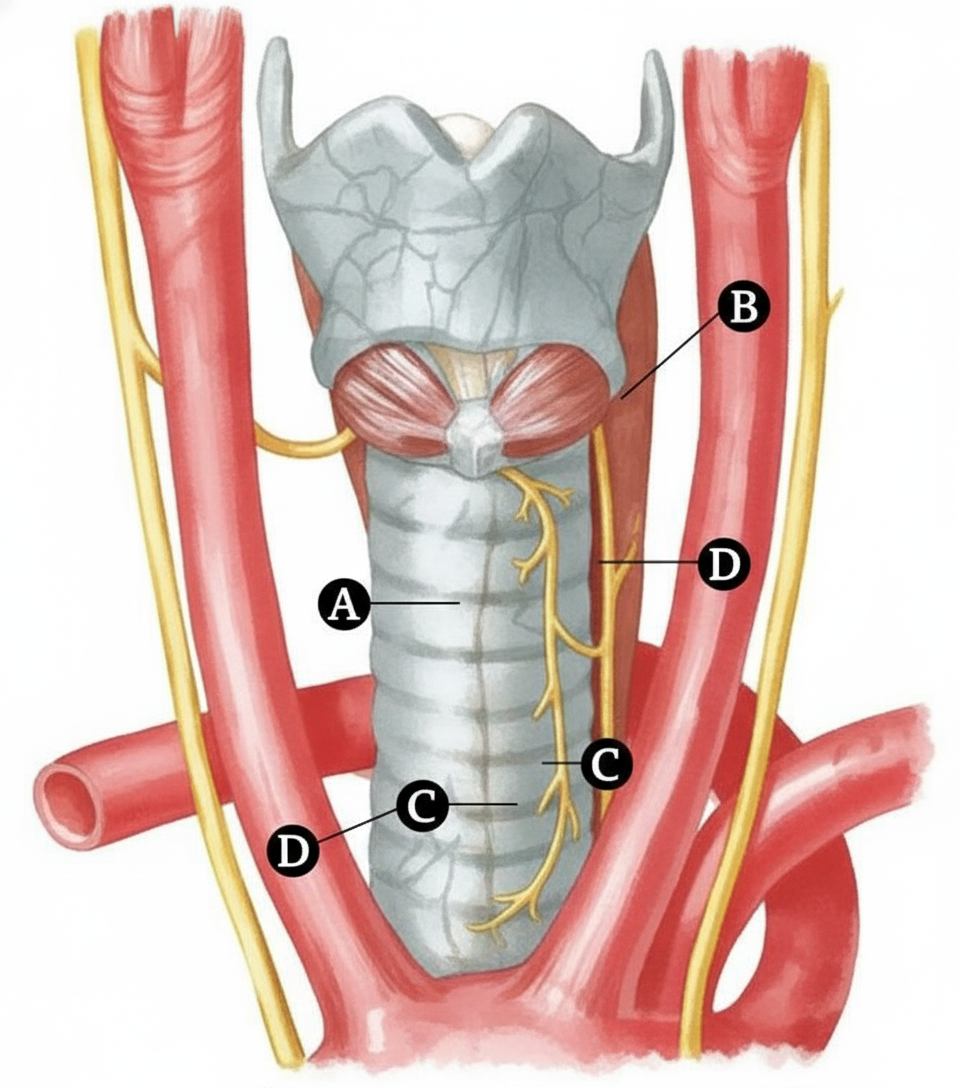
Different nerves are marked in the given diagram. Which of the following nerves supplies the posterior cricoarytenoid muscle?
Which muscle of the neck has a dual nerve supply?
Practice by Chapter
Cervical Fascia
Practice Questions
Triangles of the Neck
Practice Questions
Deep Structures of the Neck
Practice Questions
Thyroid and Parathyroid Glands
Practice Questions
Vasculature of the Neck
Practice Questions
Lymphatic Drainage
Practice Questions
Cervical Plexus
Practice Questions
Root of the Neck
Practice Questions
Applied Anatomy and Clinical Correlations
Practice Questions
Surface Anatomy of the Neck
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
