Histology — MCQs

On this page
Which of the following is not typically seen in a chronic case of sickle cell anemia?
Tuberculosis of the testis first affects which of the following structures?
Which cells of the mononuclear phagocyte system are present in the liver?
What is true about Intercalated Discs?
Dust cells can be found in which organ?
Which is the first carpal bone to ossify?
A patient presents with bleeding due to platelet function defects. Which of the following features is typically observed?
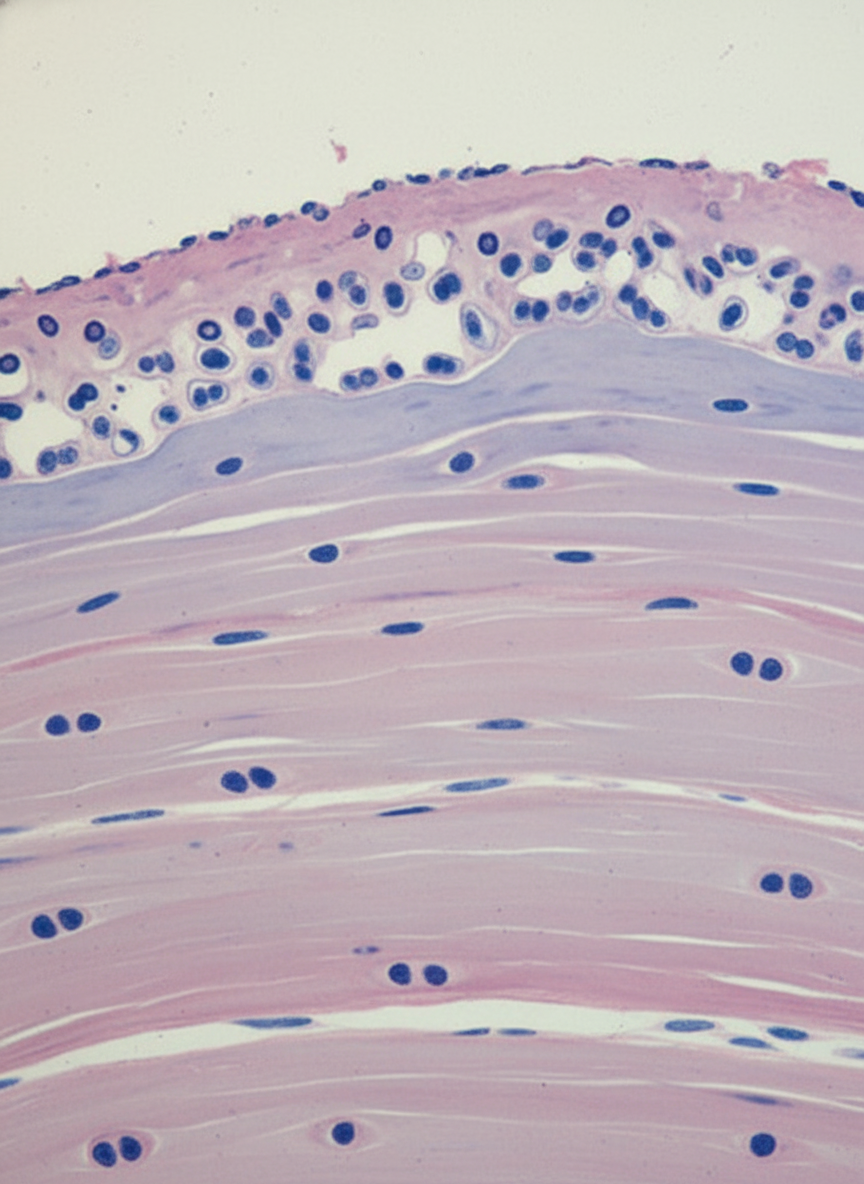
Microscopic examination of the articular surface of a synovial joint demonstrates the following histology representing:
What is the primary storage form of iron in the body?
A 55-year-old smoker presents with a history of 5 episodes of macroscopic hematuria, each lasting for about 4-5 days in the past 5 years. Which of the following investigations should be performed to evaluate the suspected cause?
Practice by Chapter
Basic Tissue Types
Practice Questions
Cell Biology and Organelles
Practice Questions
Epithelial Tissue
Practice Questions
Connective Tissue
Practice Questions
Muscular Tissue
Practice Questions
Nervous Tissue
Practice Questions
Cardiovascular System Histology
Practice Questions
Lymphoid Organs and Immune System
Practice Questions
Endocrine System Histology
Practice Questions
Respiratory System Histology
Practice Questions
Digestive System Histology
Practice Questions
Urinary and Reproductive System Histology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
