Histology — MCQs

On this page
All of the following are true about type-II pneumocytes, EXCEPT:
Fat is present in relation to which anatomical structure?
Elastic cartilage is found in which of the following locations?
What is the primary treatment modality for extragonadal germ cell tumors?
Myelin is stained by which of the following techniques?
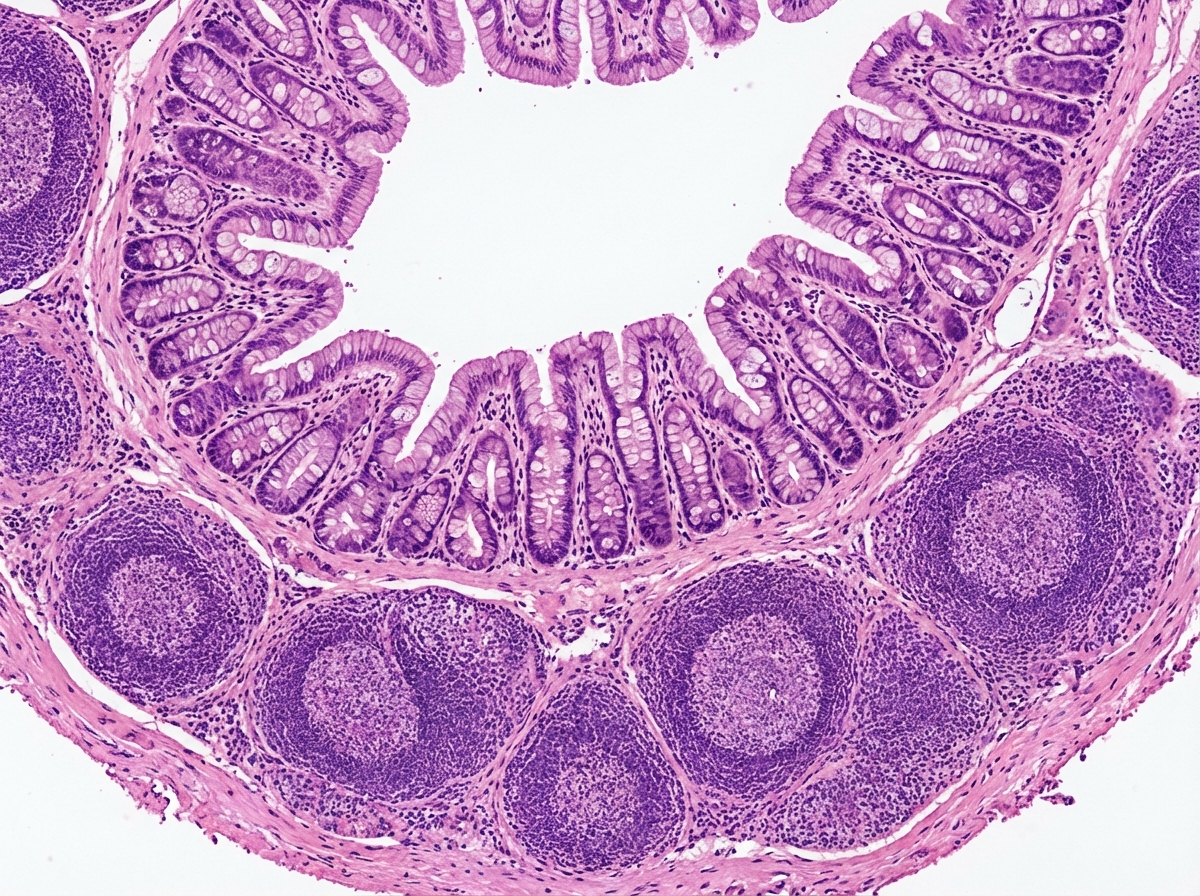
The given histological specimen is:
A peripheral smear demonstrates leukemia composed of small mature lymphocytes without blast forms. What is the most likely age of this patient?
Which of the following types of dendritic cells are characteristically found in the thymus?
Articular cartilage is primarily composed of which type of collagen?
Which cells of the liver play a role in the absorption of Vitamin A and Vitamin D?
Practice by Chapter
Basic Tissue Types
Practice Questions
Cell Biology and Organelles
Practice Questions
Epithelial Tissue
Practice Questions
Connective Tissue
Practice Questions
Muscular Tissue
Practice Questions
Nervous Tissue
Practice Questions
Cardiovascular System Histology
Practice Questions
Lymphoid Organs and Immune System
Practice Questions
Endocrine System Histology
Practice Questions
Respiratory System Histology
Practice Questions
Digestive System Histology
Practice Questions
Urinary and Reproductive System Histology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
