Histology — MCQs

On this page
Hassall's corpuscles are found in?
Elastic fibers of tunica media are secreted by
Lining epithelium of vagina is
The nasopharynx is primarily lined by which type of epithelium?
T cells in lymph node are present in:
What is the approximate ratio of connective tissue to smooth muscle in the cervix?
Which type of collagen is primarily responsible for forming the basement membrane sheets?
What is the approximate number of cones in the human retina?
Type of collagen found in space of Disse in liver is -
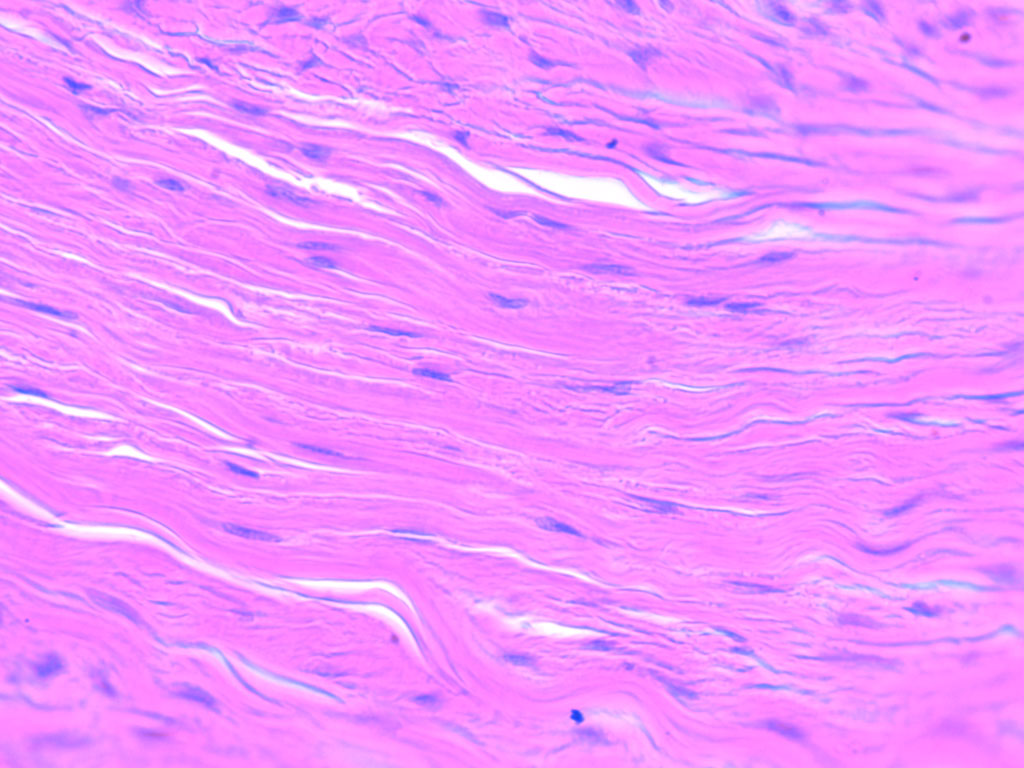
Identify the type of connective tissue present in the image.
Practice by Chapter
Basic Tissue Types
Practice Questions
Cell Biology and Organelles
Practice Questions
Epithelial Tissue
Practice Questions
Connective Tissue
Practice Questions
Muscular Tissue
Practice Questions
Nervous Tissue
Practice Questions
Cardiovascular System Histology
Practice Questions
Lymphoid Organs and Immune System
Practice Questions
Endocrine System Histology
Practice Questions
Respiratory System Histology
Practice Questions
Digestive System Histology
Practice Questions
Urinary and Reproductive System Histology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
