Histology — MCQs

On this page
Identify the type of cartilage shown in the figure:
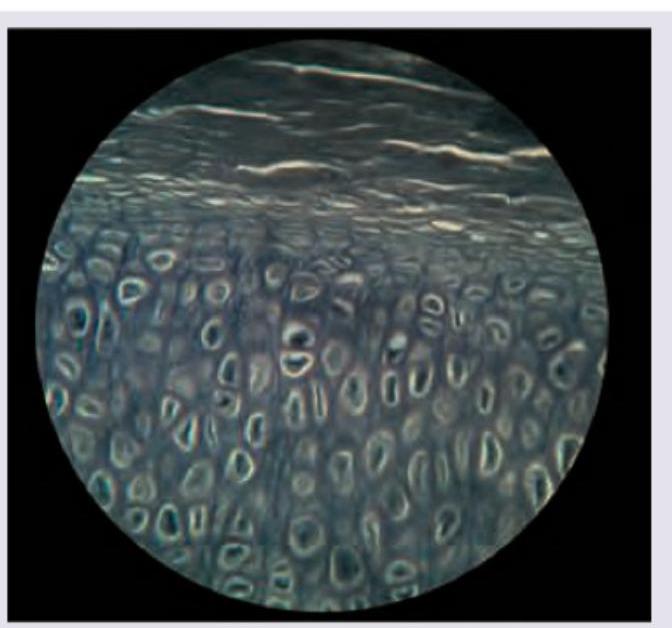
All are true about the cartilage shown in the figure except: (Recent NEET Pattern 2016-17)
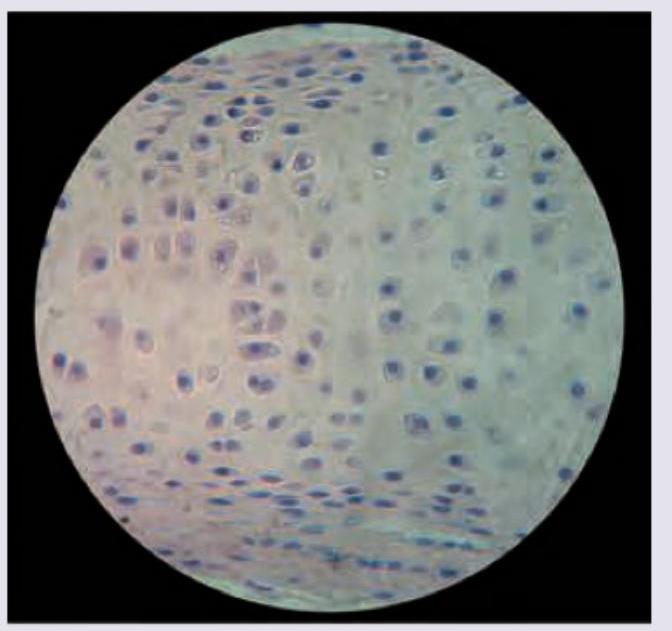
Identify the type of cartilage shown in the figure:
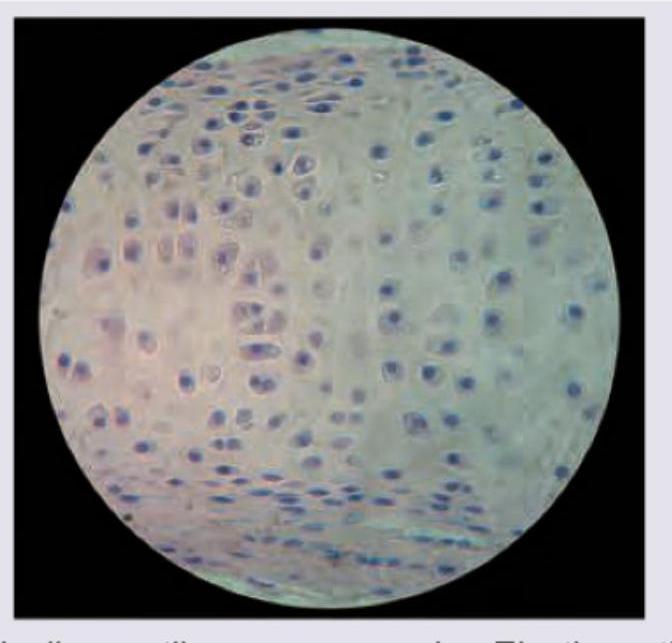
Which of the following has holocrine secretion?
Identify the type of connective tissue present in the area marked with the arrow.
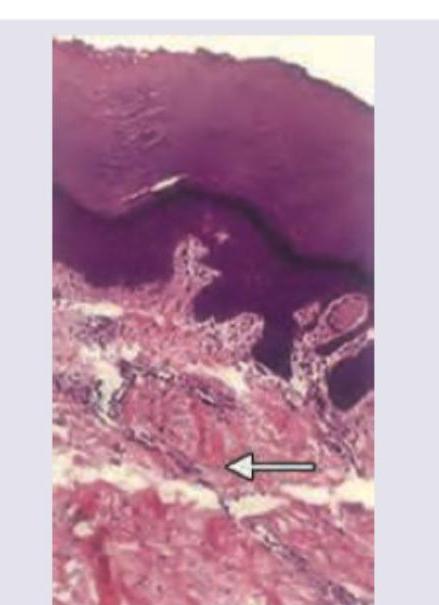
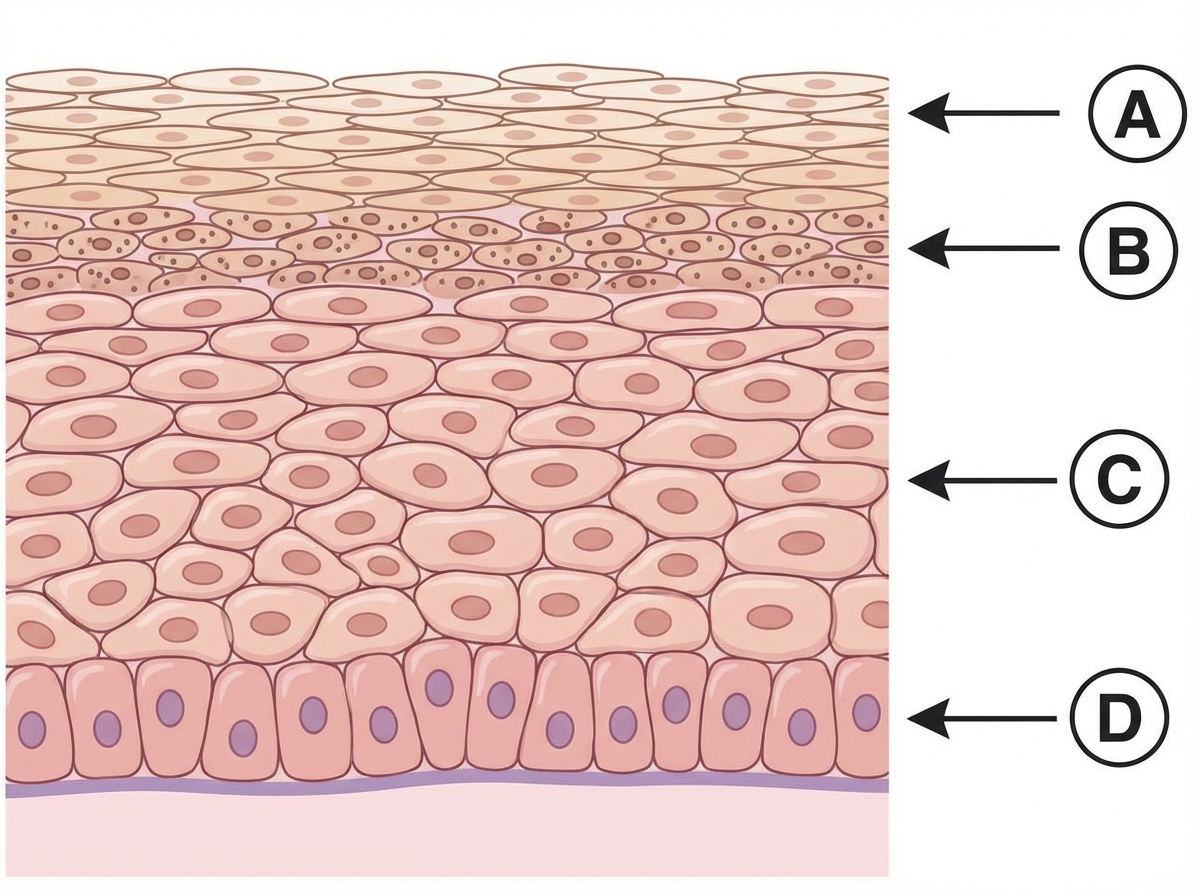
Identify the marked layer in the given histological section.
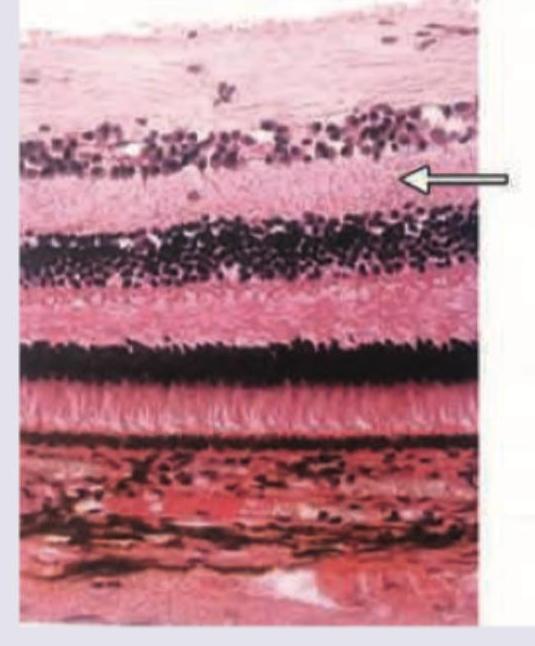
The cells marked as $X$ are called:
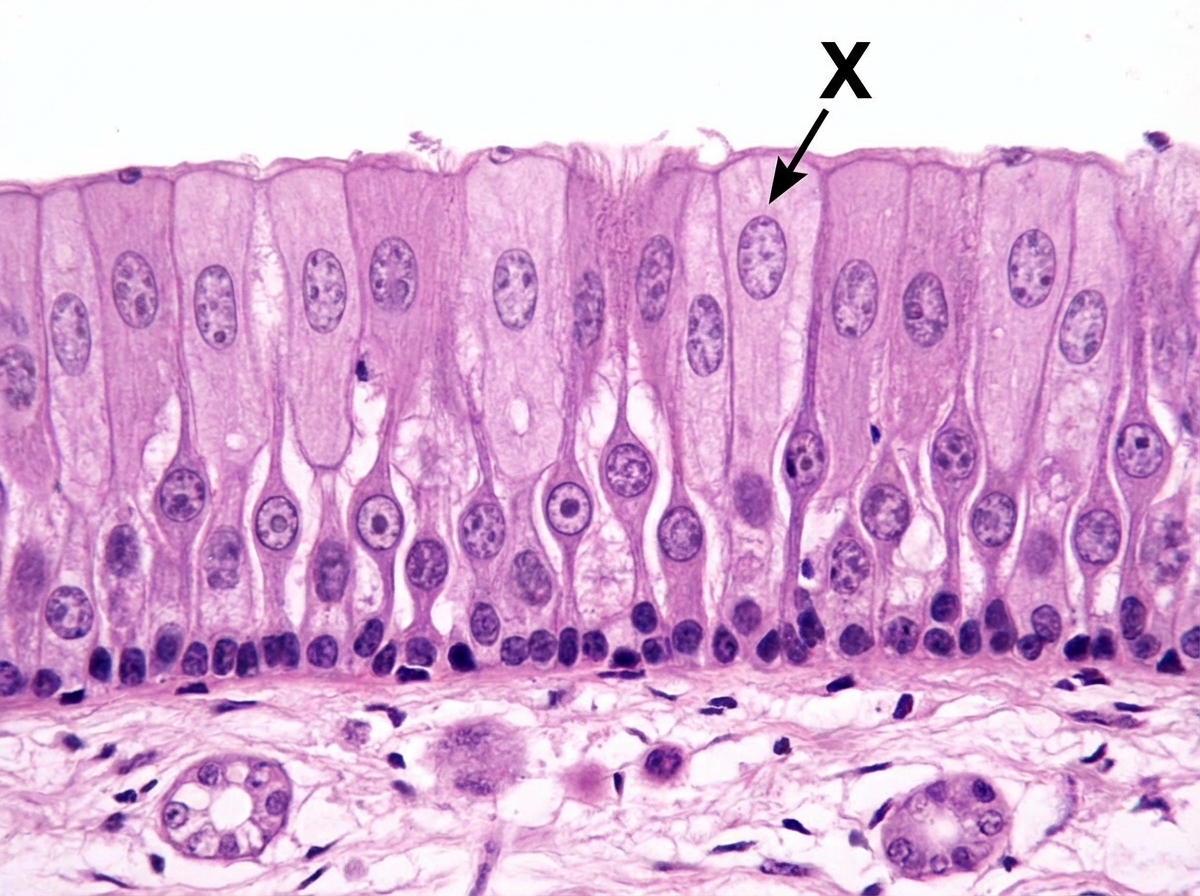
The area marked as $X$ is called:
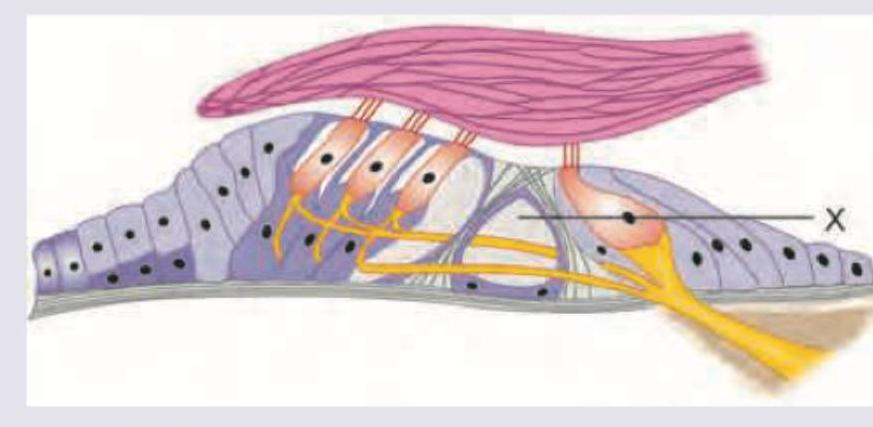
Which of the following layers has abundance of desmosomes? (AIIMS Nov 2017)
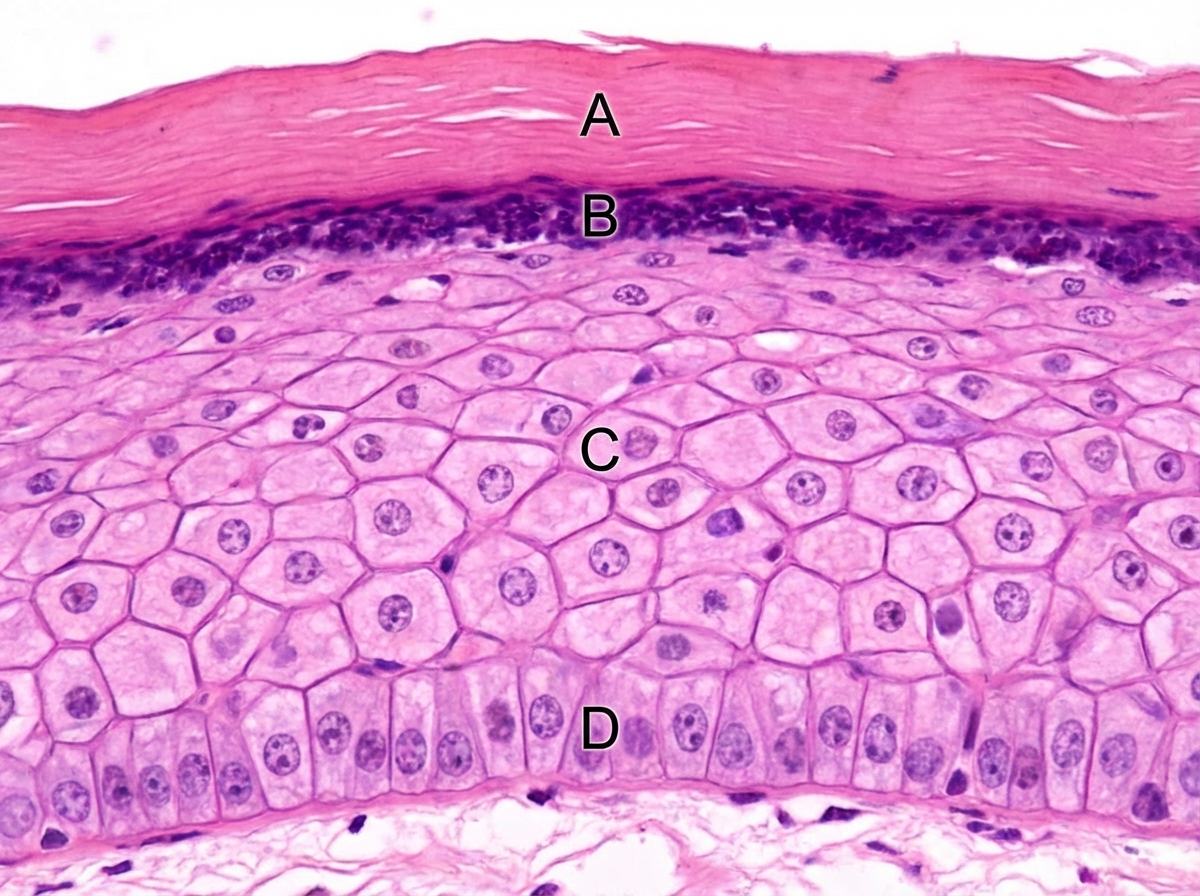
Which of the following layers contains Odland bodies?
Practice by Chapter
Basic Tissue Types
Practice Questions
Cell Biology and Organelles
Practice Questions
Epithelial Tissue
Practice Questions
Connective Tissue
Practice Questions
Muscular Tissue
Practice Questions
Nervous Tissue
Practice Questions
Cardiovascular System Histology
Practice Questions
Lymphoid Organs and Immune System
Practice Questions
Endocrine System Histology
Practice Questions
Respiratory System Histology
Practice Questions
Digestive System Histology
Practice Questions
Urinary and Reproductive System Histology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
