Histology — MCQs

On this page
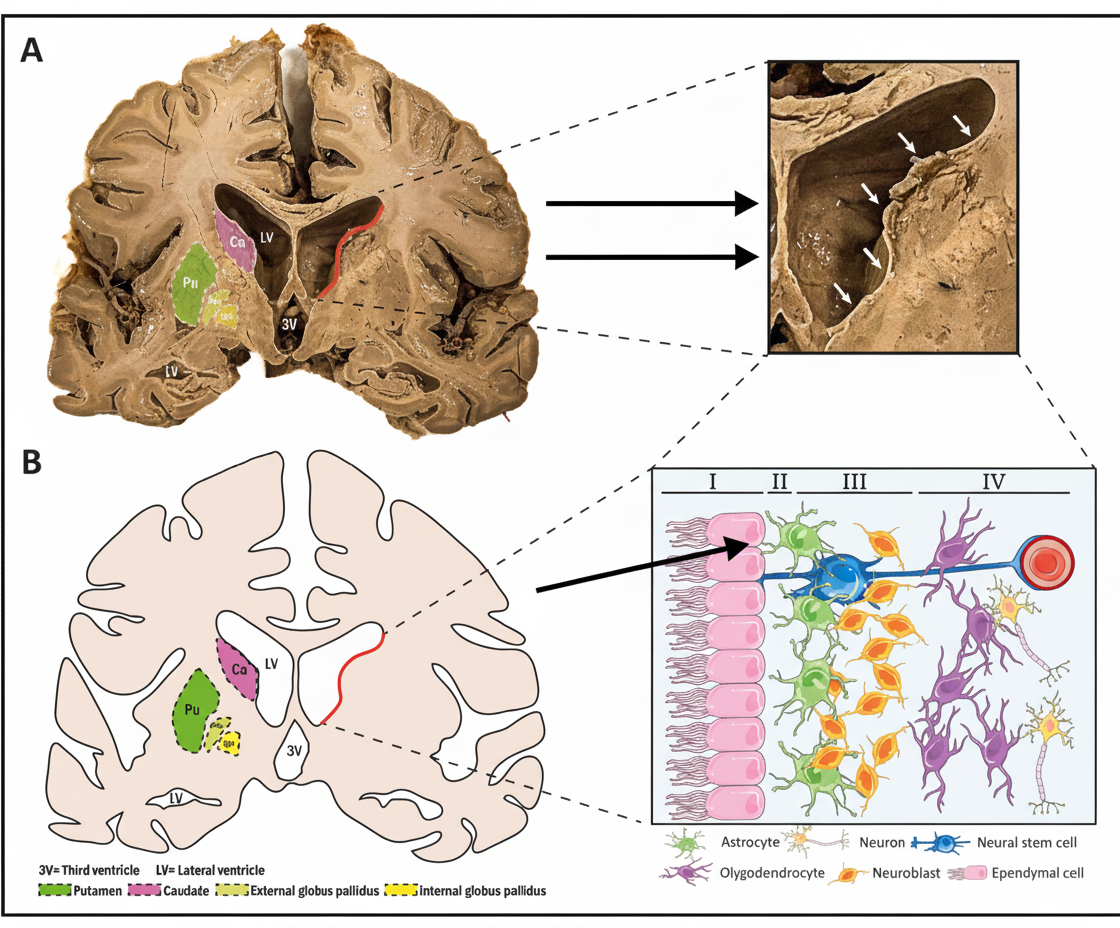
What is the type of epithelium lining the structures indicated by arrows in the provided diagram of the brain?
Ureteric colic due to a stone is primarily caused by:
Which of the following does not form the ground substance?
On the basis of anatomical knowledge of the pelvis, a rupture of the urethra above the deep perineal pouch will lead to extravasation of urine in which of the following locations?
What is the specific name for tissue macrophages?
What is the most suitable test to assess iron stores?
Which is the only fixed cell of connective tissue?
Which of the following is NOT a feature of neuroglia cells?
Kupffer cells are a type of:
Mucin is not secreted by which of the following cells/structures?
Practice by Chapter
Basic Tissue Types
Practice Questions
Cell Biology and Organelles
Practice Questions
Epithelial Tissue
Practice Questions
Connective Tissue
Practice Questions
Muscular Tissue
Practice Questions
Nervous Tissue
Practice Questions
Cardiovascular System Histology
Practice Questions
Lymphoid Organs and Immune System
Practice Questions
Endocrine System Histology
Practice Questions
Respiratory System Histology
Practice Questions
Digestive System Histology
Practice Questions
Urinary and Reproductive System Histology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
