Histology — MCQs

On this page
A midline protrusion in the maxillary region is mostly due to which of the following?
The term Stratum Malpighi refers to which of the following layers of the epidermis?
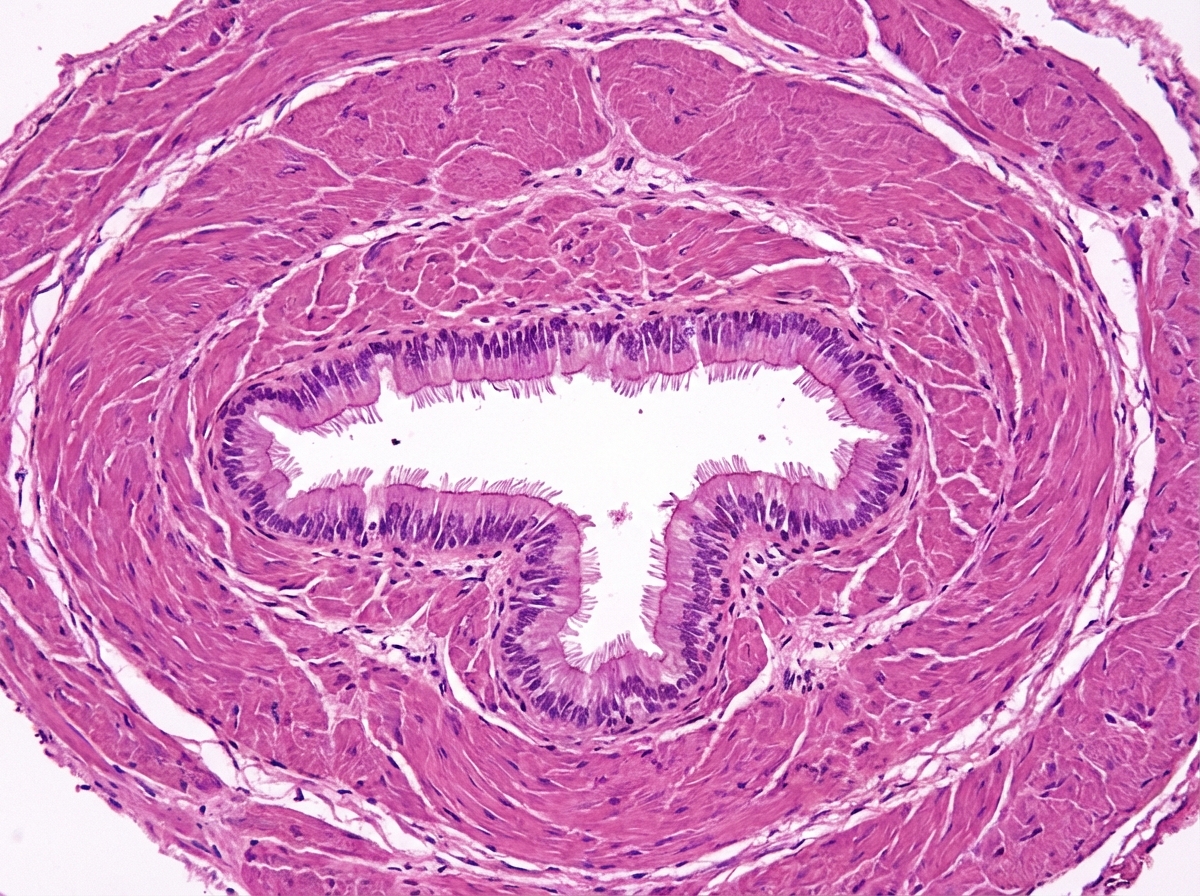
The following histological sample belongs to which of the following tissues?
Mean corpuscular hemoglobin concentration (MCHC) is increased in which of the following conditions?
Which type of collagen is present in the basement membrane?
Which stain is used for fat cells?
Small intestine and colon are lined by which type of epithelium?
What type of collagen is predominantly found in the ovary?
Circumcision is included in the management of Ca penis at which site?
Paneth cells are known to contain which of the following trace elements?
Practice by Chapter
Basic Tissue Types
Practice Questions
Cell Biology and Organelles
Practice Questions
Epithelial Tissue
Practice Questions
Connective Tissue
Practice Questions
Muscular Tissue
Practice Questions
Nervous Tissue
Practice Questions
Cardiovascular System Histology
Practice Questions
Lymphoid Organs and Immune System
Practice Questions
Endocrine System Histology
Practice Questions
Respiratory System Histology
Practice Questions
Digestive System Histology
Practice Questions
Urinary and Reproductive System Histology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
