Embryology and Development — MCQs

On this page
What is the embryological basis for the uterine anomaly shown in the images?
What stage of embryonic development is shown in the following image?
What is the most common type of ventricular septal defect?
Which of the following structures develop from the 6th pharyngeal arch artery on the left side?
The condition seen in the image results from failure of fusion of:
A patient presents cyst on the neck with anterior to the sternocleidomastoid at the junction of the upper and middle third of the muscle. This cyst is due to the persistence of which of the following embryological clefts?
The image shows a congenital cardiac defect. Abnormal development of which branch of aortic arch leads to this defect?
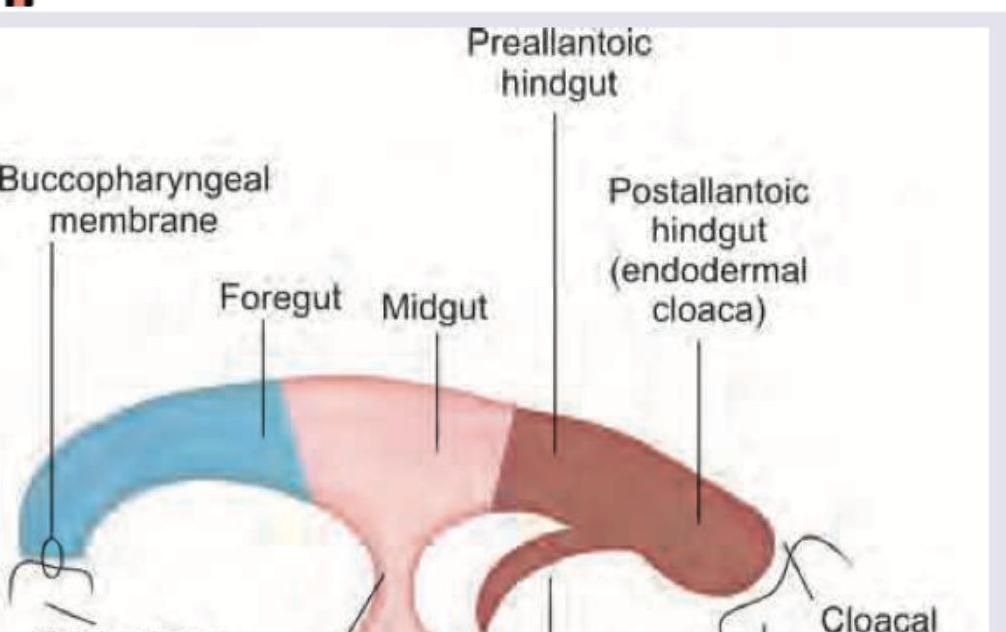
Which is correct sequence about the blood supply of the primitive gut?
Which is wrong about the image given below?
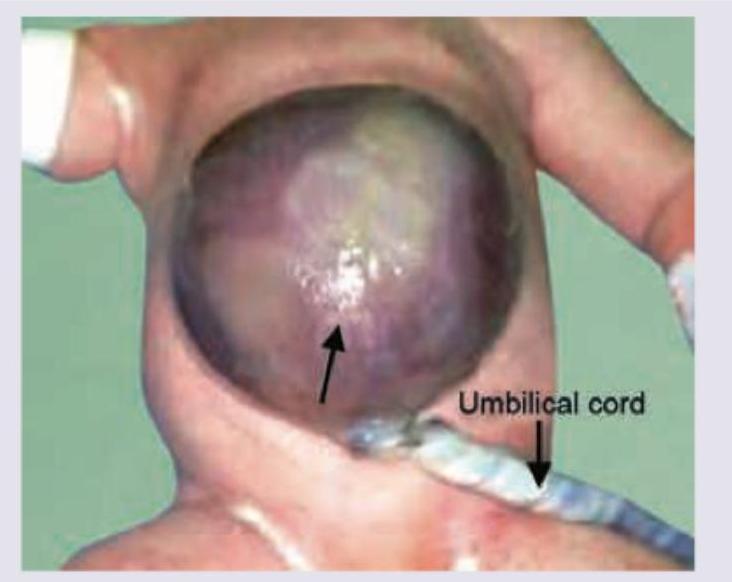
The condition shown below is due to ?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
