Embryology and Development — MCQs

On this page
The internal carotid artery is a derivative of which pharyngeal arch?
Cochlear function in the fetus develops between which gestational weeks?
Which of the following is NOT one of the phases of implantation of the embryo?
A double aortic arch is due to persistent?
The dorsal panus of the ventral mesogastrium forms which of the following structures?
A 5-day-old male infant is diagnosed with Hirschsprung disease. CT scan examination reveals an abnormally dilated colon. Which of the following is the most likely embryologic mechanism responsible for Hirschsprung disease?
A patient at 22 weeks gestation is diagnosed with intra-uterine fetal demise (IUFD) that occurred at 17 weeks. The patient is at increased risk of which of the following complications?
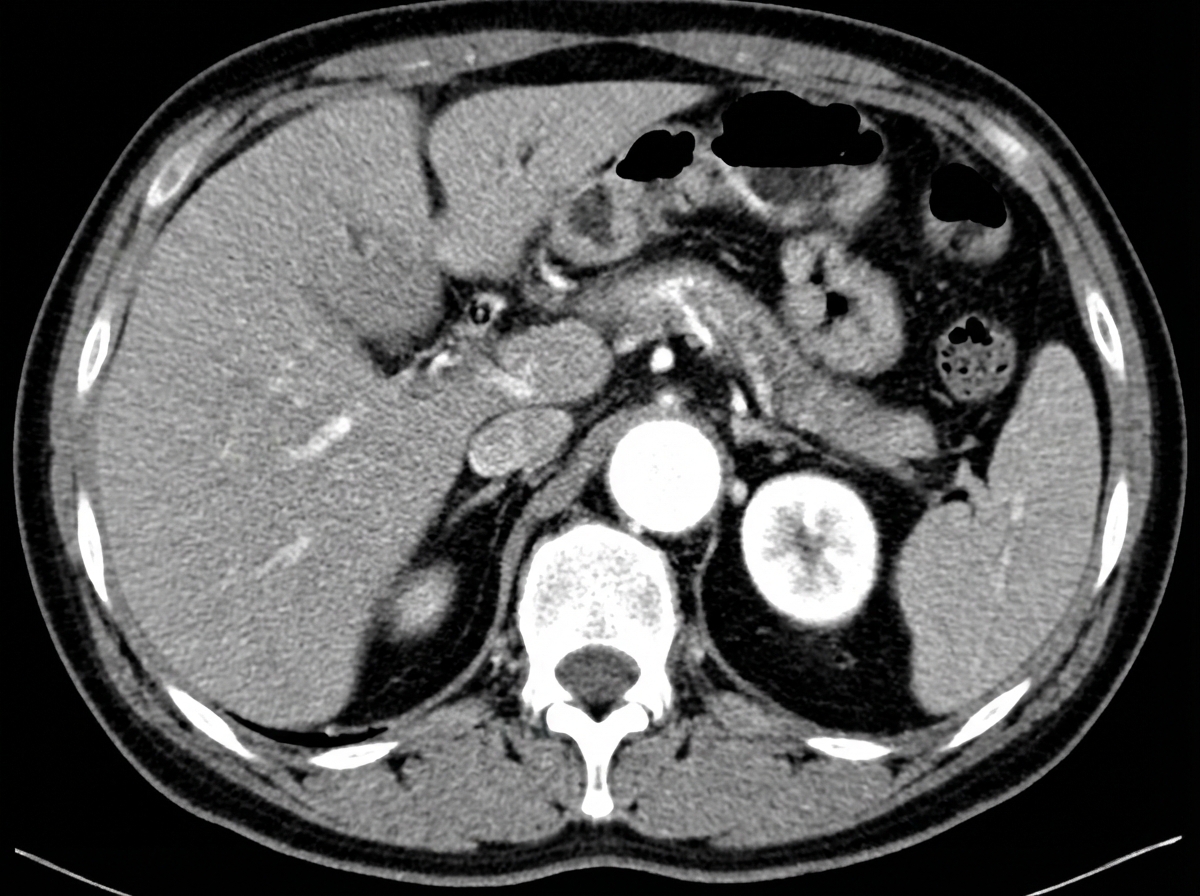
Complete regression of which of the following veins causes this anomaly in the development of the Inferior Vena Cava?
Which cranial nerve supplies the musculature of the first pharyngeal arch?
Merkel cells of the epidermis are derived from which embryonic structure?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
