Embryology and Development — MCQs

On this page
All of the following statements about the embryology of Meckel's diverticulum are true except:
Hirschsprung's disease is due to?
The third ventricle is derived from which embryonic structure?
Independent assortment of chromosomes occurs at which stage of meiosis?
Trophoblast differentiates at which post-fertilization day?
A 3-month-old child presents with a typical mewing cry and congenital heart disease. Which chromosome abnormality is associated with these findings?
What is the term for a dome-shaped skull?
What is the term for a primary defect in structure?
In the adult heart, the floor of the fossa ovalis represents:
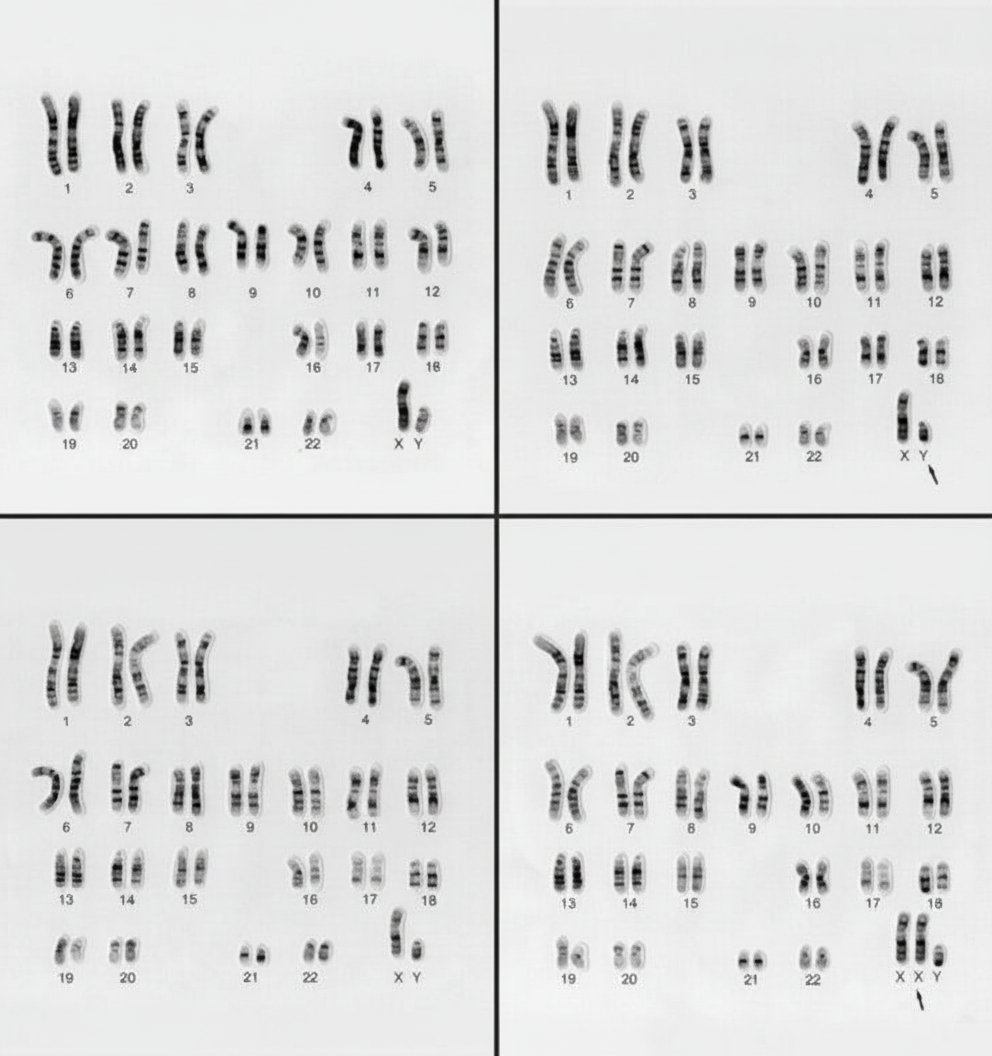
What is the abnormality seen in the following karyotype?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
