Embryology and Development — MCQs

On this page
Anatomical closure of the Ductus Arteriosus takes place at what time after birth?
Pierre Robin syndrome is a:
Parafollicular cells develop from which embryological structure?
By which week of gestation does the gender of a fetus become clearly distinguishable from external genitalia?
Differentiation of the genital ridge takes place at which gestational age?
Which embryonic structure gives rise to the facial skeleton?
The sinus occupying the coronary sulcus is derived from which of the following?
The second maturation division of the human ovum occurs at the time of?
Which of the following structures is derived from the surface ectoderm?
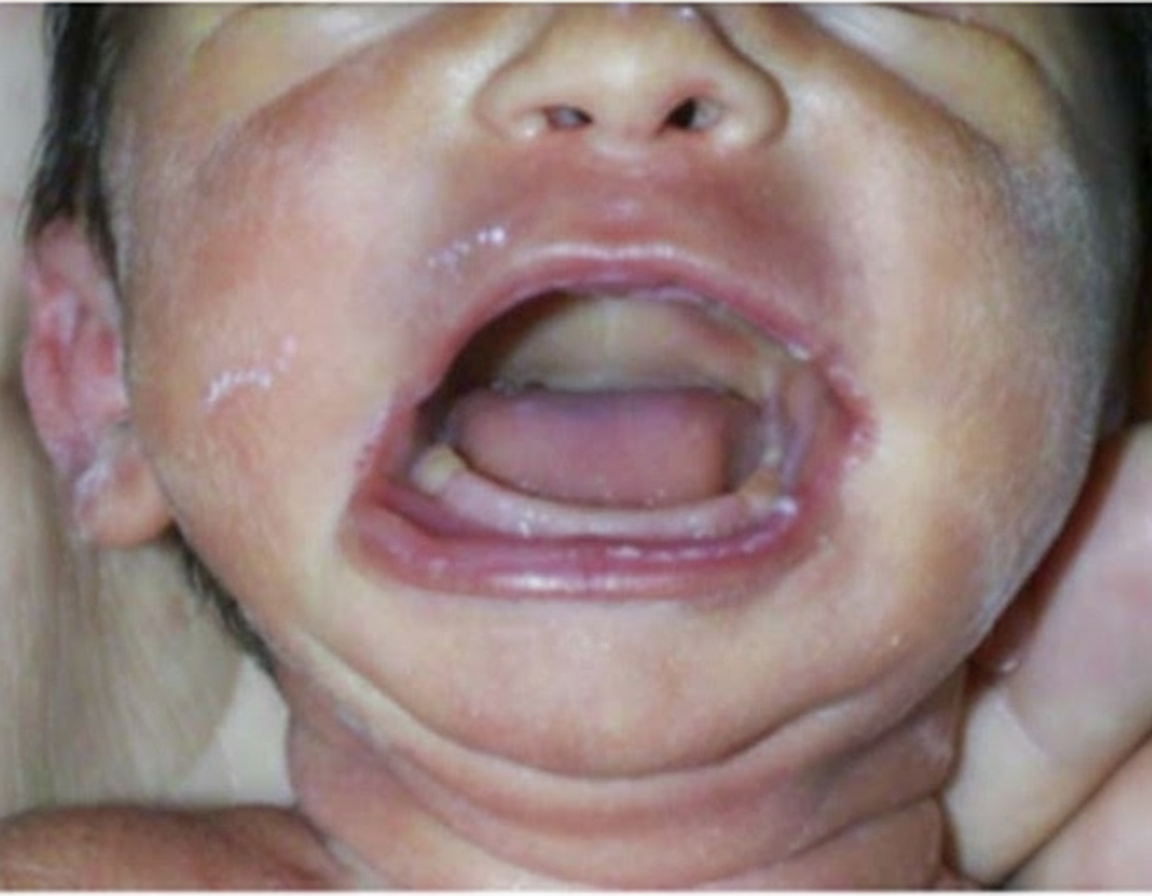
The given deformity is due to which of the following developmental anomalies?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
