Embryology and Development — MCQs

On this page
All of the following develop from the Wolffian duct except:
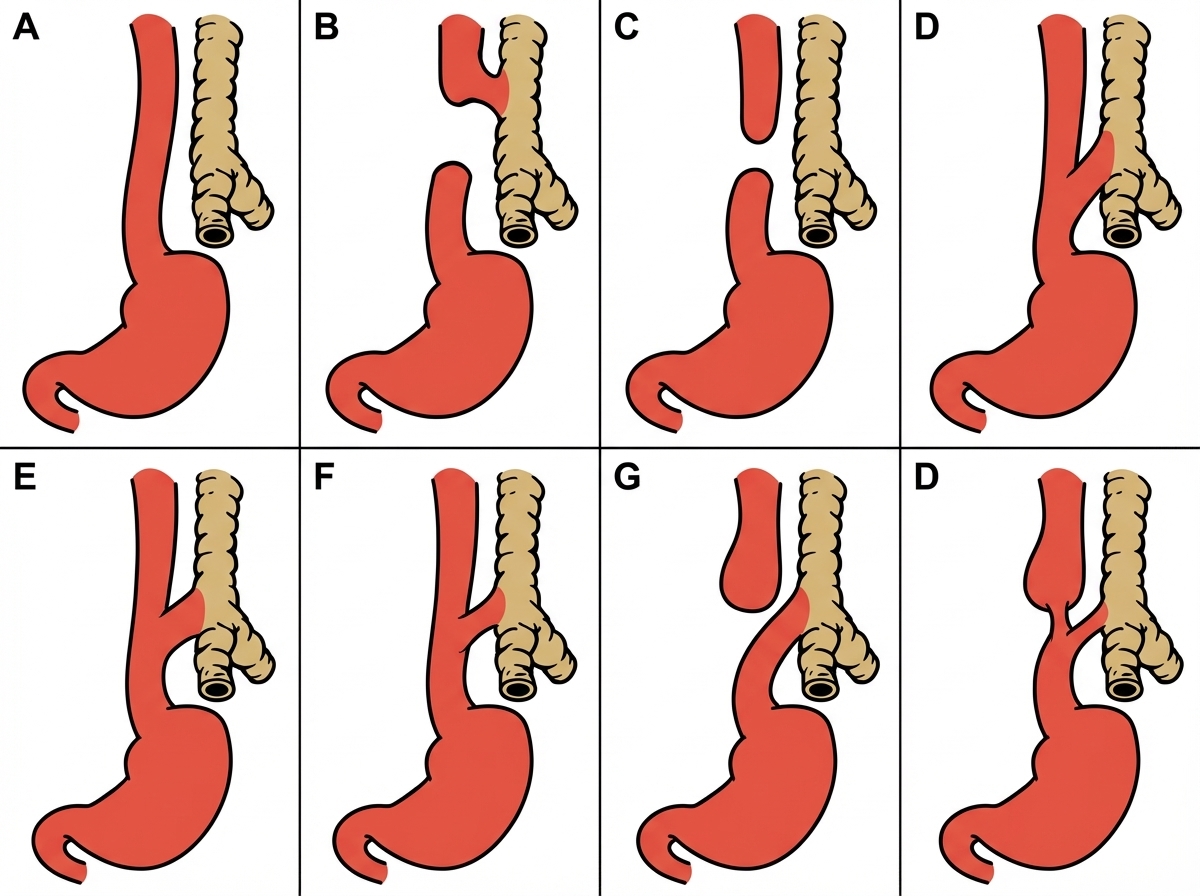
Shortly after birth, an infant develops abdominal distention and begins to drool. When she is given her first feeding, it runs out the side of her mouth, and she coughs and chokes. Physical examination reveals tachypnea, intercostal retractions, and bilateral pulmonary rales. Which esophageal anomaly most commonly causes these signs and symptoms?
All of the following are ectodermal derivatives EXCEPT?
At what gestational age do spontaneous fetal movements typically begin?
Which of the following statements is NOT true regarding the zona pellucida?
At what gestational age are breathing movements and swallowing movements typically observed in a fetus?
Extramedullary hematopoiesis is very common in the human fetus. At 8 months' gestation, the most important site of hematopoiesis is the:
The external auditory meatus develops from which embryonic structure?
A 3-month-old female infant is diagnosed with anal stenosis after several periods of stool infrequency, two of which lasted 10 days without a bowel movement. Which of the following is the most likely cause of this condition?
All of the following organs develop in the mesentery of the stomach except:
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
