Embryology and Development — MCQs

On this page
Which of the following structures is derived from the second pharyngeal arch?
Embryologically, the dorsal aorta forms which of the following structures?
Which of the following structures is NOT derived from the second pharyngeal arch?
The corneal stroma is derived from which embryonic tissue?
Which umbilical vessel disappears by the 4th month of gestation?
All of the following statements regarding the development of the thyroid gland are true, EXCEPT:
Which of the following events occurs during the third week of human embryo development?
Formation of the primary palate is from which of the following structures?
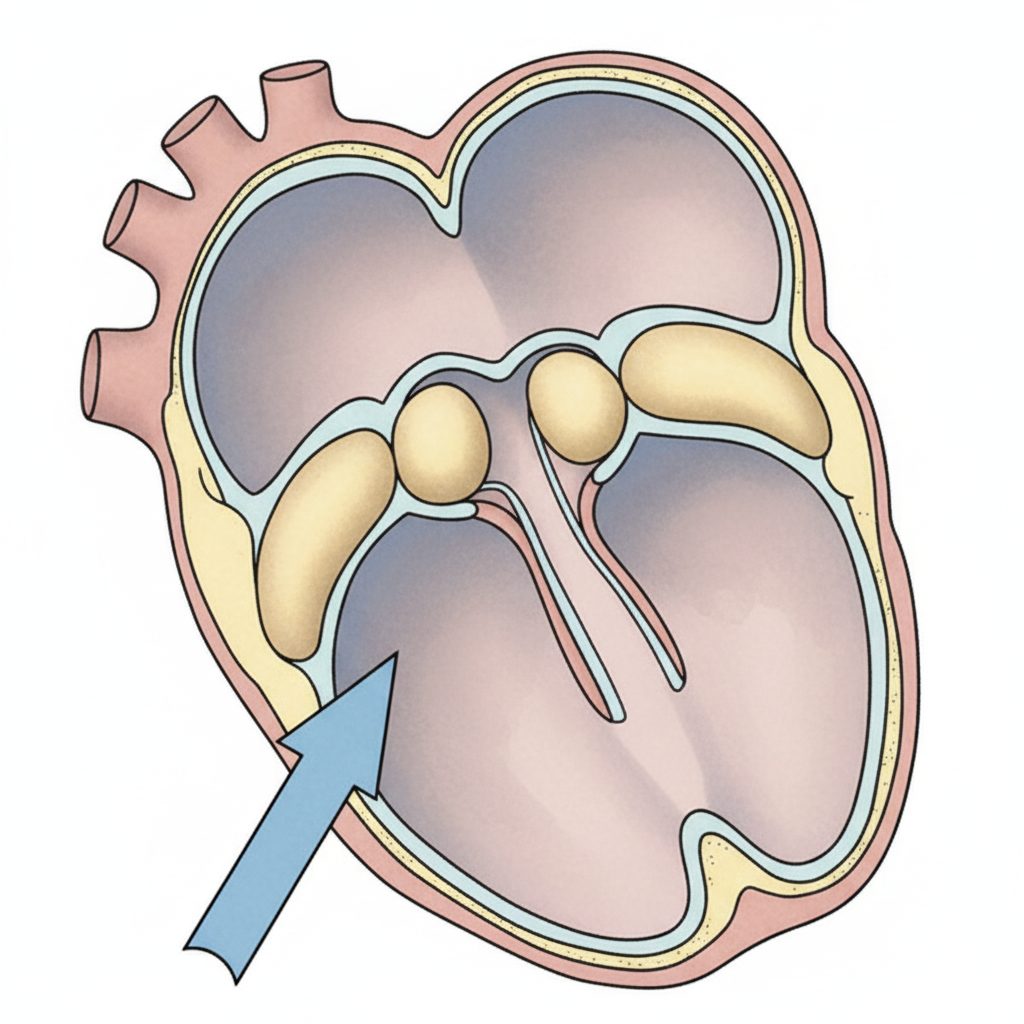
The structure marked by the blue arrow develops from which of the following structures?
The embryonic period is defined as the time from fertilization until which week of development?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
