Embryology and Development — MCQs

On this page
The heart assumes its normal four-chambered shape by the end of which week of gestation?
Which of the following is not an embryologic structure that contributes to the formation of the face?
A male newborn infant is brought to the clinic by his mother and diagnosed with a congenital malformation. MRI studies reveal that the cerebellum and medulla oblongata are protruding inferiorly through the foramen magnum into the vertebral canal. What is this clinical condition called?
The conus arteriosus is derived from which of the following?
Intermediate mesoderm is the precursor of which of the following structures?
The thymus develops from which pharyngeal arch?
Remnant of vitello intestinal duct causes which of the following?
Oxygenated blood to the fetus is carried by?
What is the most likely condition depicted below?
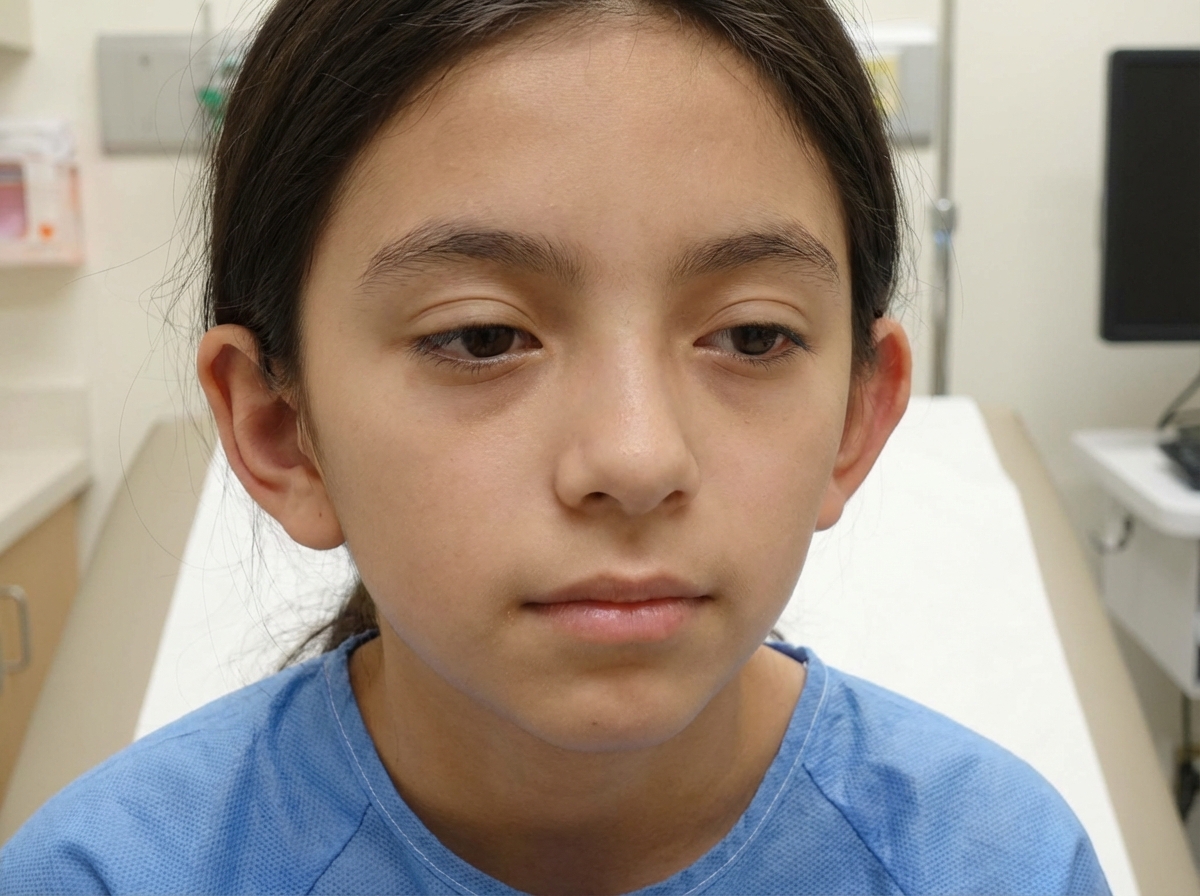
Rohr's stria are found in?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
