Embryology and Development — MCQs

On this page
What is the female homologue of the scrotum?
The mandible is embryologically derived from which structure?
Lumbar hemivertebra results due to the abnormal development of:
Embryologically, the forehead develops from which of the following structures?
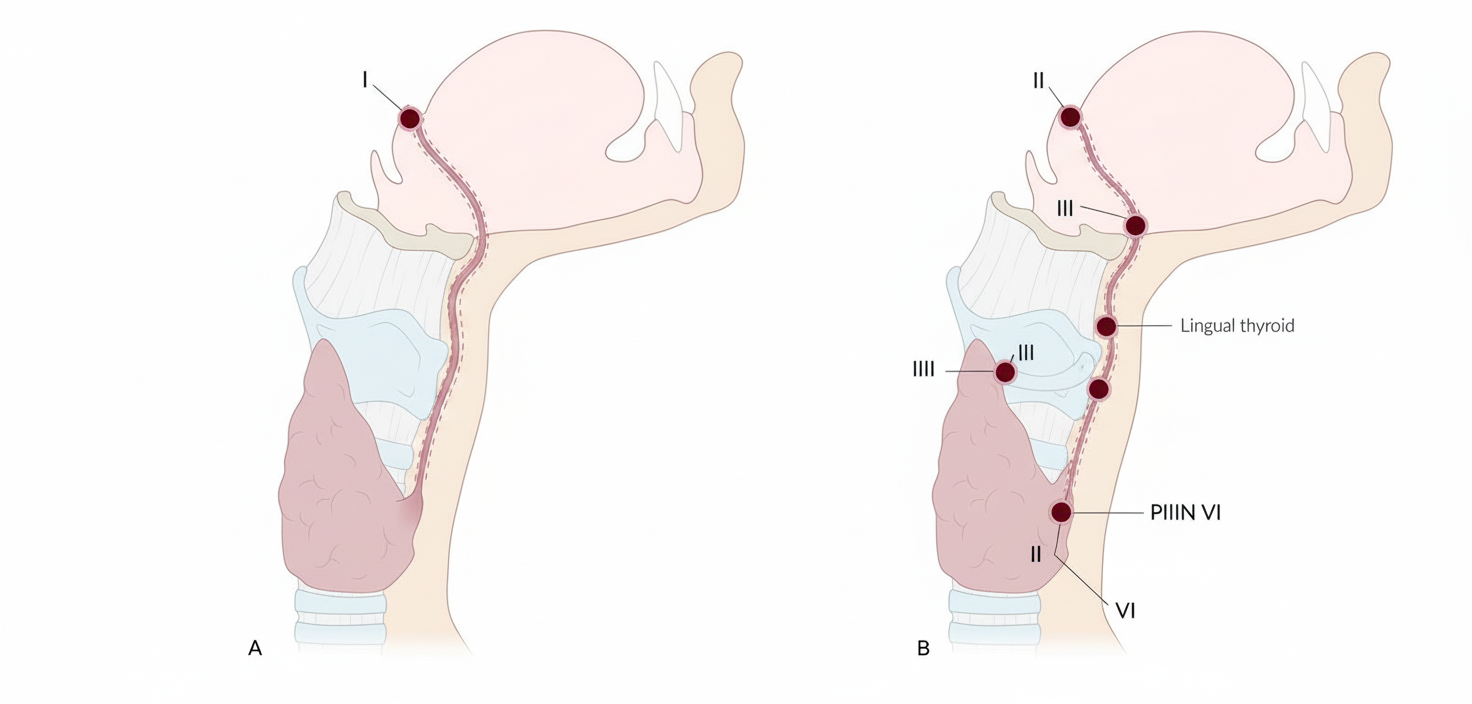
The diagram represents the path traversed in the neck by the developing thyroid gland embryo. Which point along this path is the commonest site of a thyroglossal cyst?
What is the derivative of the 3rd pharyngeal arch?
At which age of intrauterine life is the heart fully developed?
Trisomy 13 is also known as which syndrome?
During intrauterine life, which of the following organs is not dependent upon the placenta?
Which muscle is derived from the third pharyngeal arch?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
