Embryology and Development — MCQs

On this page
Which of the following is NOT a true statement regarding the derivatives of the aortic arches?
Which of the following statements is NOT true regarding paramedian pits?
The Glossopharyngeal nerve supplies the posterior 1/3 of the tongue because it develops from which embryological structure?
The diaphragm is formed of all the following except?
Ossification of long bones begins at what age?
What is the name of the congenital anomaly this child is suffering from?
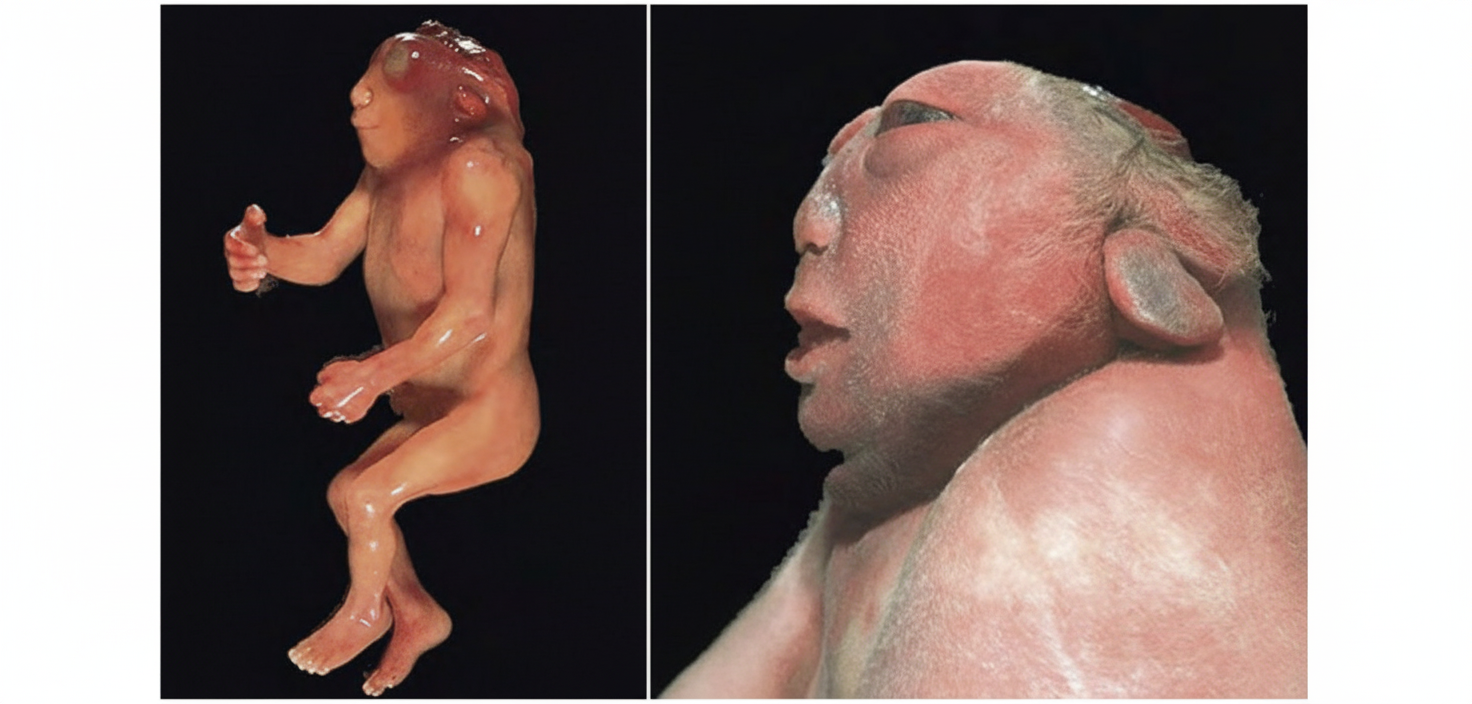
The visceral efferent column of the neural tube arises from which embryonic structure?
During the first 3-4 months of gestation, erythrocytes are formed by which structure?
During development, the parts of the ear develop at different intervals. All of the following structures are of adult size at birth, EXCEPT?
Oogonia reach their maximum number at which of the following stages of human development?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
