Embryology and Development — MCQs

On this page
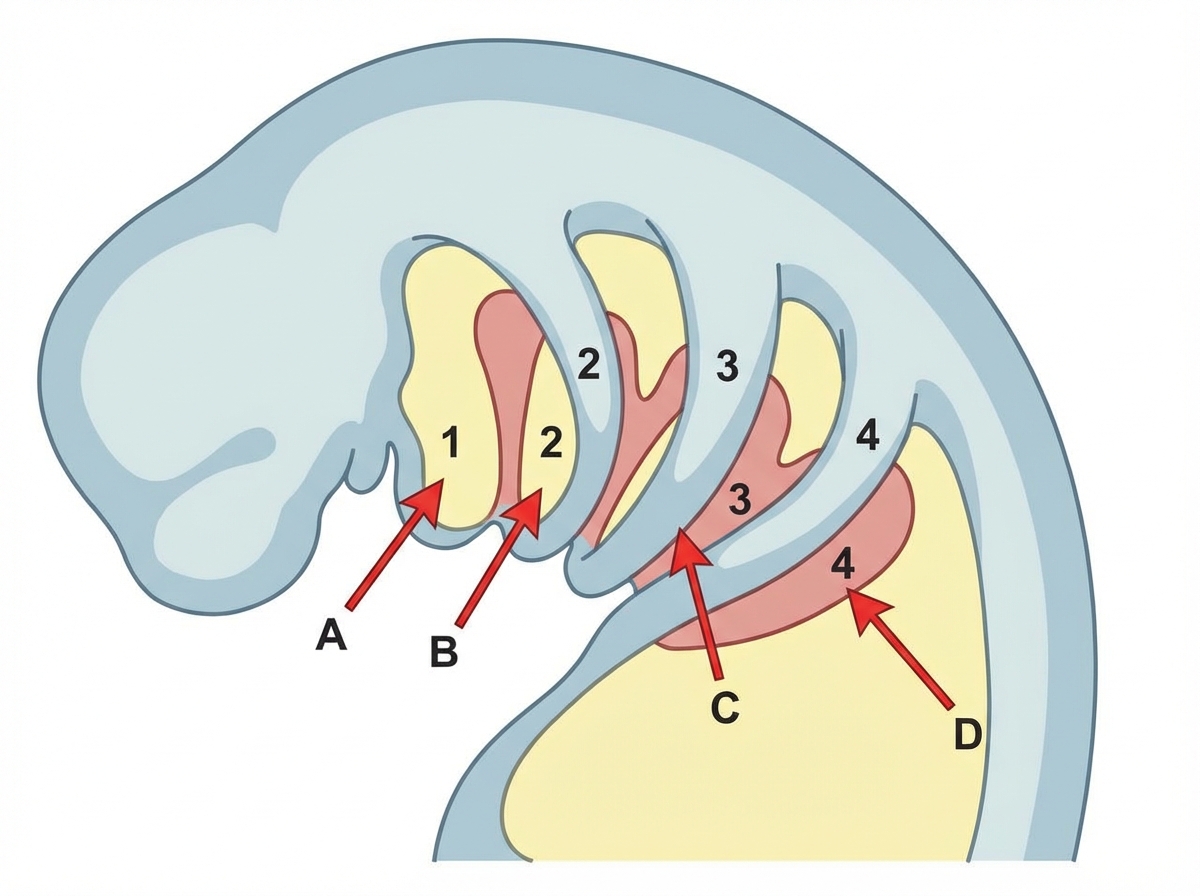
A young patient with absent thymus presents with tetany and hypoparathyroidism. Which of the following is a marked area in the picture defective in this condition?
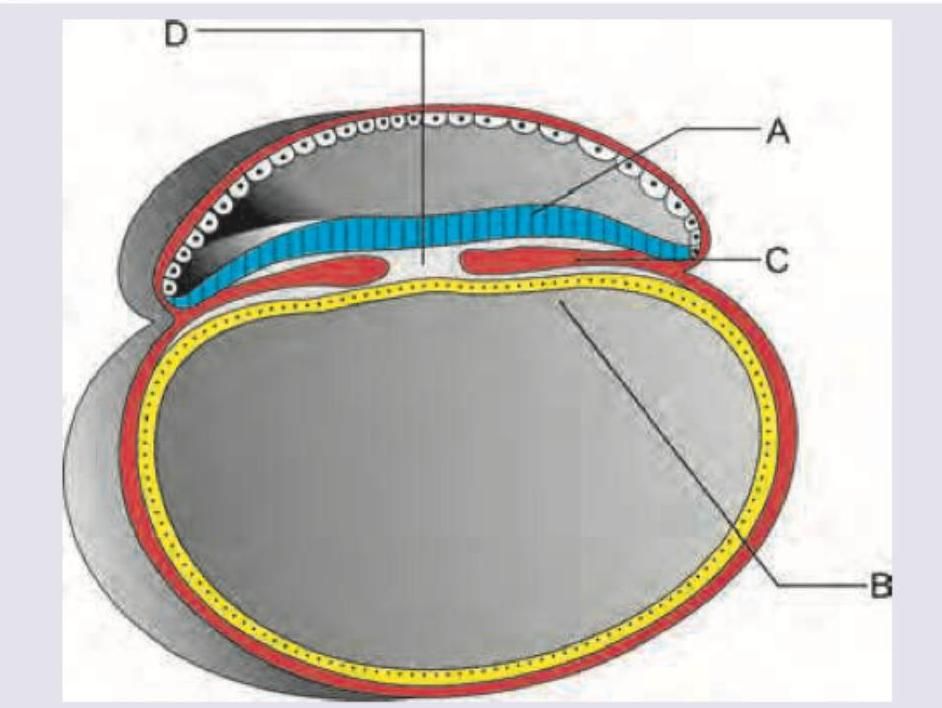
Nucleus pulposus develops from: (AIIMS May 2018)
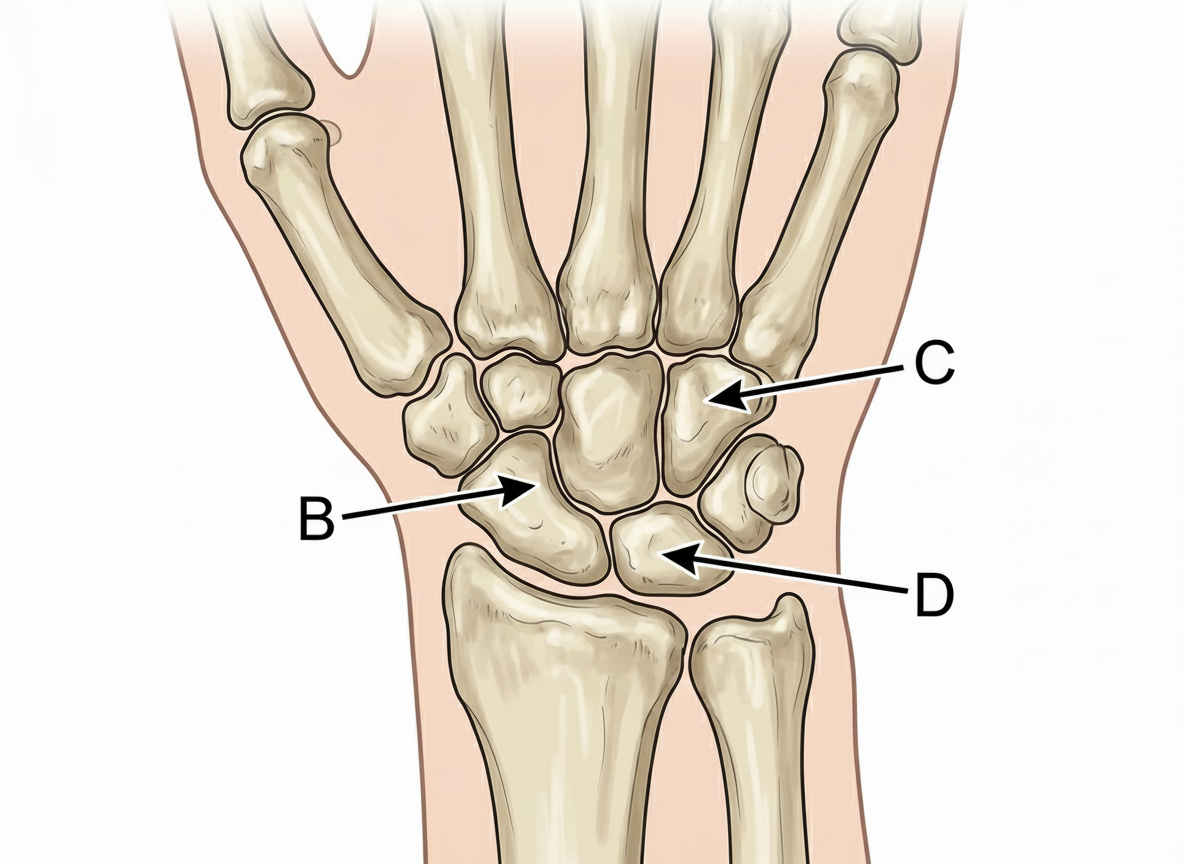
Which of the following bones is the first one to ossify?
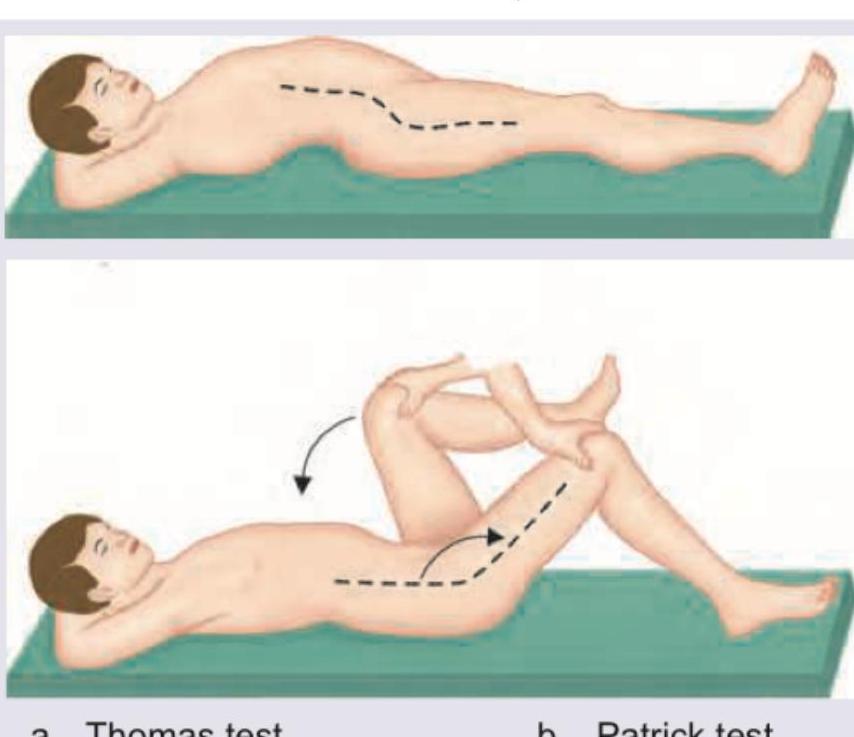
Identify the clinical examination test being performed in the given image.
The following USG scan should prompt you to screen for which of the following disorders?
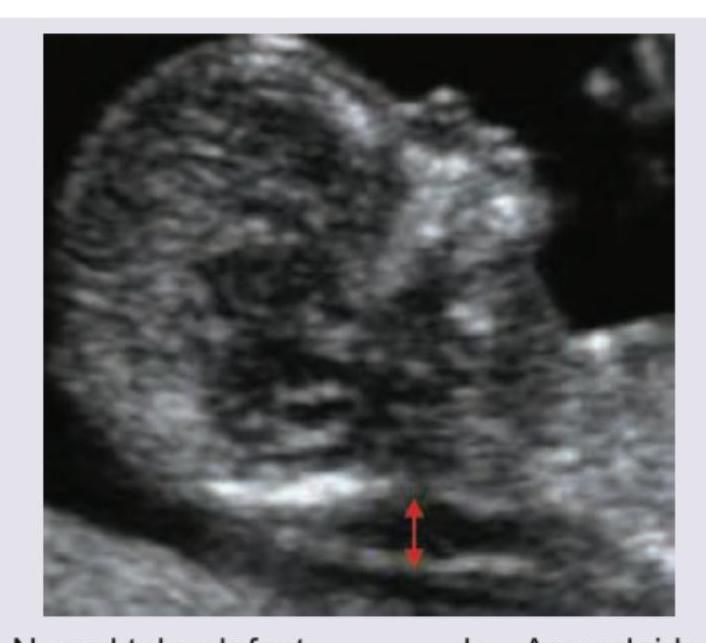
The image shows:
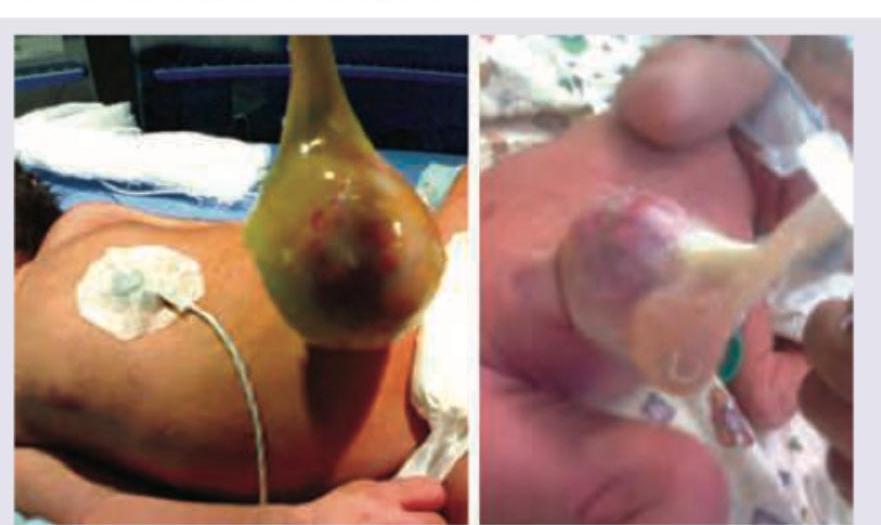
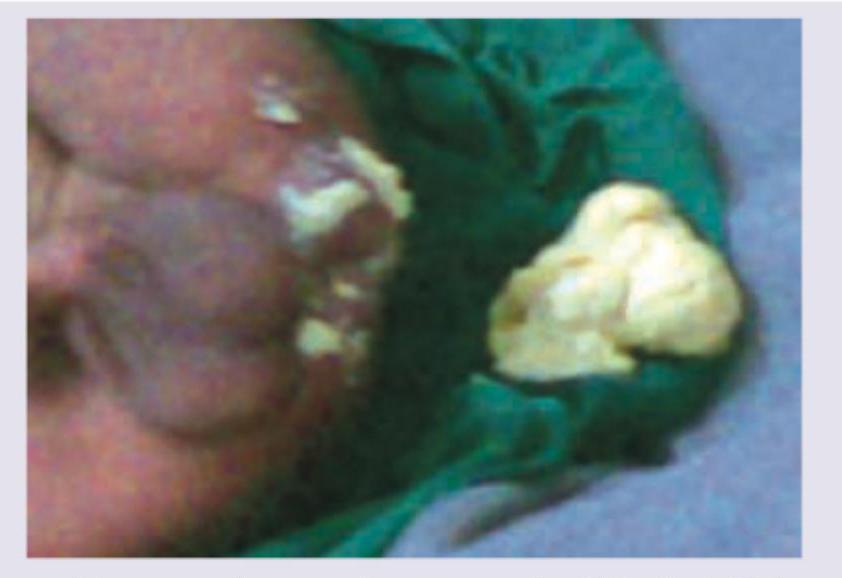
A 2-week-old neonate presents with feeding problems and otitis media. Based on the clinical image, what is the most likely diagnosis?
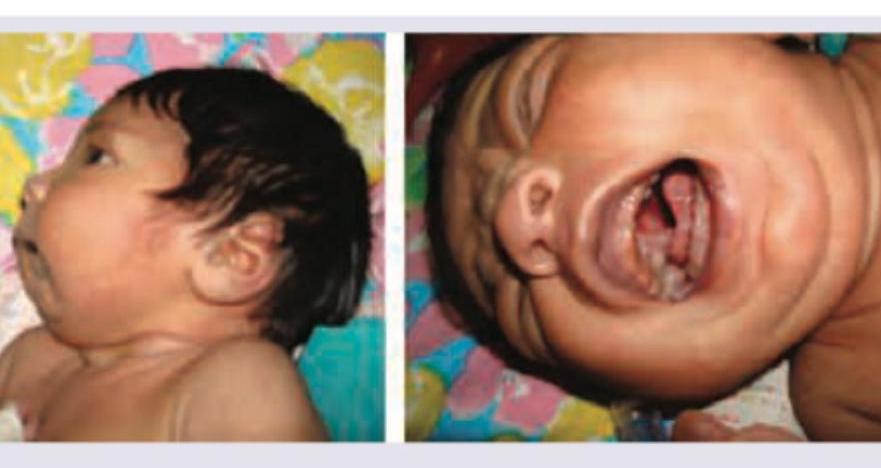
A 2-day-old neonate under phototherapy unit. For exchange transfusion serum bilirubin-albumin ratio should be: (Recent NEET Pattern 2016-17)
A 2-day-old neonate has passed stool of the color shown in the image. Which of the following best describes the clinical possibility?
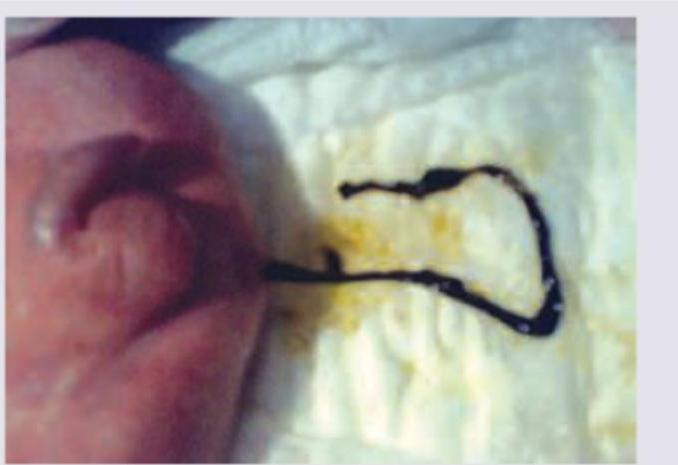
Mother of a 6-hour-old neonate has pointed to passage of stool of the following color. Which of the following best describes the clinical possibility?
Practice by Chapter
Gametogenesis and Fertilization
Practice Questions
Early Embryonic Development
Practice Questions
Placentation
Practice Questions
Development of Nervous System
Practice Questions
Development of Cardiovascular System
Practice Questions
Development of Gastrointestinal System
Practice Questions
Development of Urogenital System
Practice Questions
Development of Musculoskeletal System
Practice Questions
Development of Head and Neck
Practice Questions
Congenital Anomalies
Practice Questions
Teratology
Practice Questions
Molecular Mechanisms in Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
