Developmental Abnormalities — MCQs

Double bubble sign is seen in -
Tetralogy of Fallot (TOF) includes all of the following components except:
Seal like limbs i.e. phocomelia is a specific side effect of -
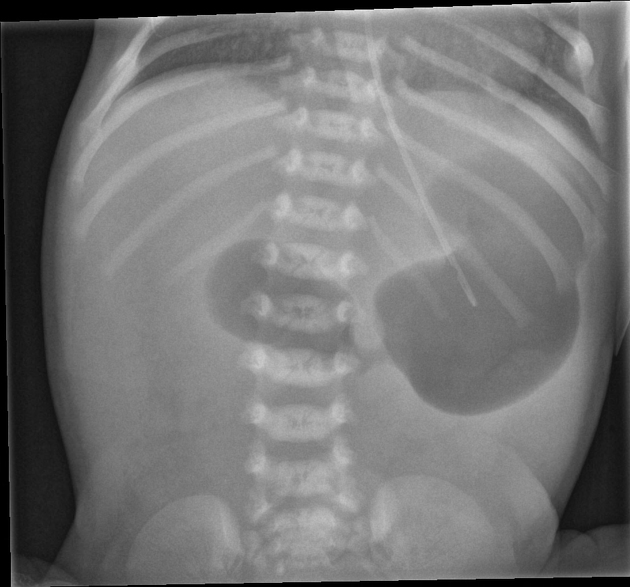
A 6-week-old baby is brought in by the mother with complaints of vomiting. An X-ray shows a single bubble appearance. What is the most likely diagnosis?
Which of the following is the MOST accurate test for detecting neural tube defects?
Which of the following is a characteristic feature of Down syndrome?
What is the time period for the embryonic period?
The labia majora develop from which embryological structure?
All of the following are neural tube defects except:
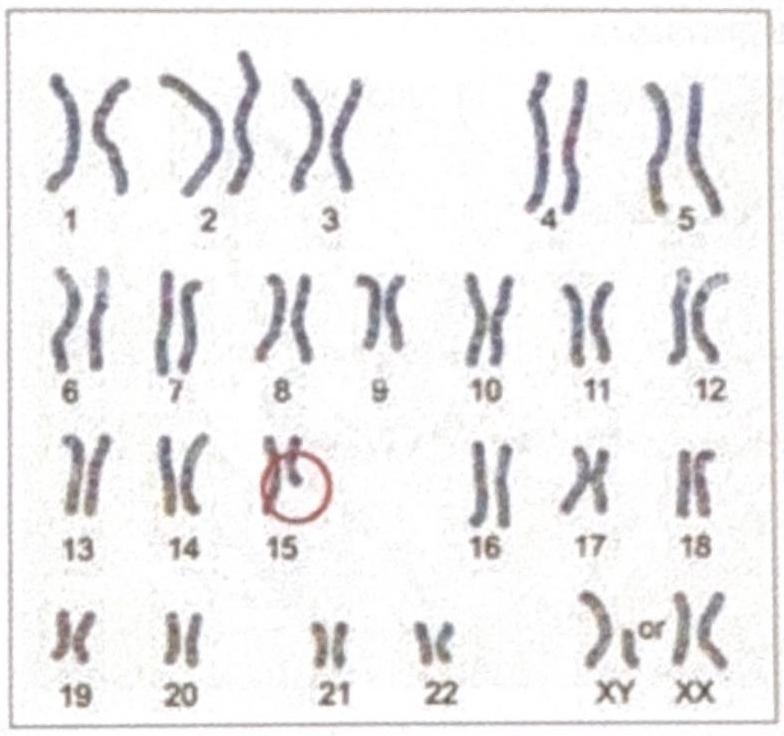
The diagrammatic representation of the karyotype of an individual indicates a specific genetic abnormality. What is the diagnosis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
