Back — MCQs

On this page
Q1Easy
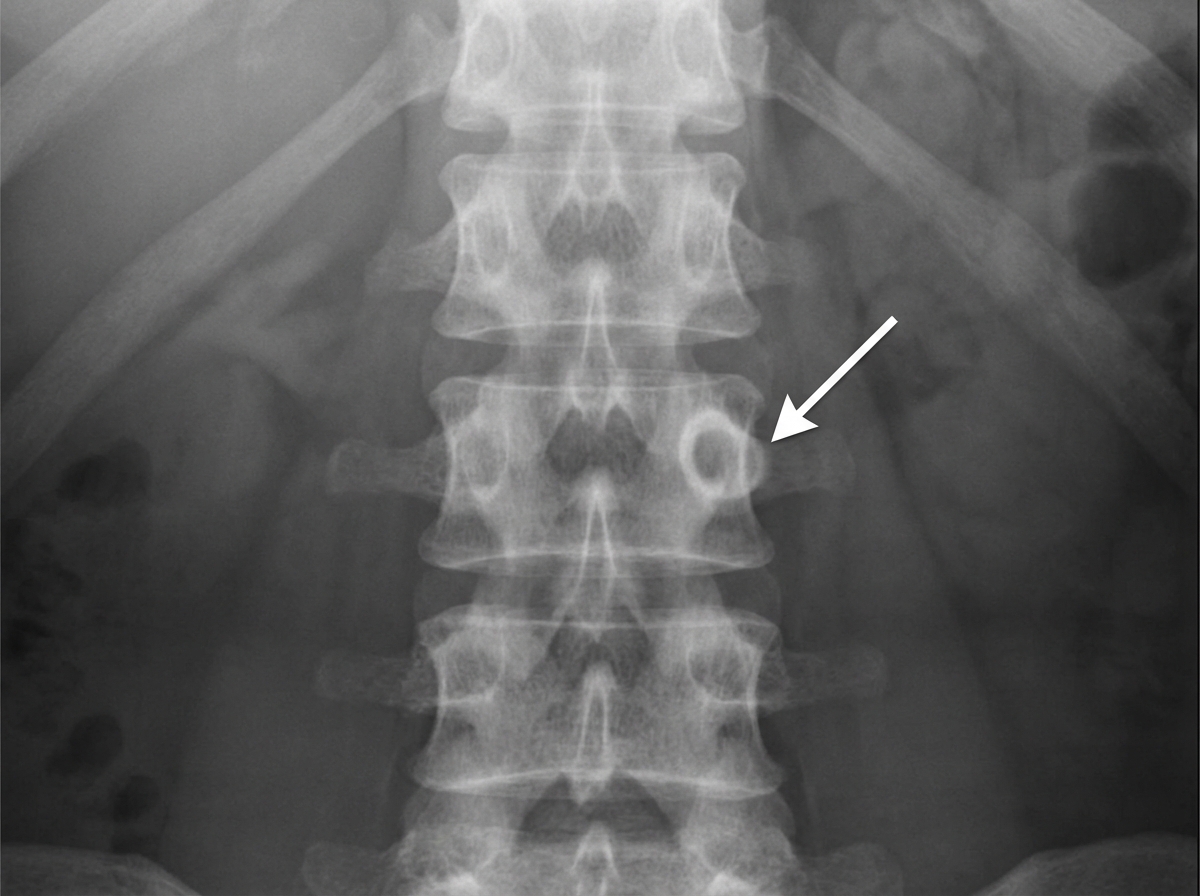
In the provided X-ray, what anatomical structure is indicated by the marked region?
Practice by Chapter
1
Vertebral Column
Practice Questions
2
Spinal Cord and Meninges
Practice Questions
3
Back Muscles and Fasciae
Practice Questions
4
Vertebral Joints and Ligaments
Practice Questions
5
Vasculature of the Back
Practice Questions
6
Innervation of the Back
Practice Questions
7
Clinical Aspects of Back Disorders
Practice Questions
8
Applied Anatomy of the Back
Practice Questions
9
Surface Anatomy of the Back
Practice Questions
10
Development of the Vertebral Column
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
