Biochemistry
1 questionsOf the following amino acids required by the human body, which one falls under the category of 'essential' amino acid?
UPSC-CMS 2022 - Biochemistry UPSC-CMS Practice Questions and MCQs
Question 111: Of the following amino acids required by the human body, which one falls under the category of 'essential' amino acid?
- A. Arginine
- B. Threonine (Correct Answer)
- C. Proline
- D. Serine
Explanation: ***Threonine*** - **Threonine** is one of the nine **essential amino acids** that the human body cannot synthesize on its own. - It must be obtained through the **diet** to support protein synthesis and other vital bodily functions. *Arginine* - **Arginine** is generally considered a **conditionally essential** or **semi-essential amino acid**. - While the body can synthesize it, requirements may increase during periods of rapid growth, illness, or stress, making dietary intake important in those situations. *Proline* - **Proline** is a **non-essential amino acid**, meaning the human body can synthesize it from other precursors. - It plays a crucial role in the structure of **collagen** and connective tissue. *Serine* - **Serine** is also a **non-essential amino acid** that can be synthesized by the human body. - It is involved in the metabolism of fats, fatty acids, and the synthesis of various other biomolecules.
Community Medicine
6 questionsRegarding maternal health programs in Community Medicine, which of the following statements about public-private partnership schemes is CORRECT?
Consider the following measures for making unlined katcha wells sanitary: 1. Deepening the bottom 2. Filling the well with clay up to the water level and with coarse sand above that level 3. Installing a hand pump with screen 4. Constructing a platform and drainage once the material used for filling is completely consolidated Which of the above measures are effective in making unlined katcha wells sanitary?
In which way is 'membrane filtration technique' better than 'multiple tube method' for determining the presence of coliform organisms in water?
Consider the following statements with reference to the National Framework for Malaria Elimination in India, 2016–2030. Which of the following statements is correct? 1. The goal is to eliminate indigenous cases throughout the country by 2030. 2. By 2022, transmission of malaria is to be interrupted and indigenous cases brought to zero in all 26 States/UTs that were under Categories 1 and 2 in 2014. 3. By 2026, incidence of malaria is to be reduced to less than 1 case per 1000 population in all States and UTs, and their districts. 4. By 2030, indigenous transmission of malaria is to be interrupted in all States and UTs of India.
With reference to determinants of 'neonatal mortality', consider the following statements: 1. Neonatal mortality is directly related to the birth weight of the newborn. 2. Neonatal mortality is directly related to the gestational age at which the birth takes place. 3. Neonatal mortality is closely related to the educational status of the mother. 4. Neonatal mortality is low if the mother's age is between 15–16 years.
The following table shows the 'Total Fertility Rate (TFR)' by the Wealth Index, as per the National Family Health Survey, (NFHS–4) findings. Which among the following is/are correct about the information?
UPSC-CMS 2022 - Community Medicine UPSC-CMS Practice Questions and MCQs
Question 111: Regarding maternal health programs in Community Medicine, which of the following statements about public-private partnership schemes is CORRECT?
- A. It is a voluntary scheme wherein any obstetrician, maternity home, nursing home, MBBS doctor can provide safe motherhood services (Correct Answer)
- B. The enrolled doctors must provide iron and folic acid tablets out of their pocket free to the beneficiaries
- C. The TT injections are provided by the District Medical Officers to the enrolled doctors for free administration to the beneficiaries
- D. To join the Vandemataram Scheme, the facility must have resources for caesarean section
Explanation: ***Correct: Statement 1 - It is a voluntary scheme wherein any obstetrician, maternity home, nursing home, MBBS doctor can provide safe motherhood services.*** - **Public-private partnership (PPP) schemes** in maternal health, such as those under **Janani Suraksha Yojana (JSY)** and related initiatives, are designed with **voluntary participation** as a cornerstone. - This allows qualified private providers including **obstetricians, maternity homes, nursing homes, and MBBS doctors** to participate, thereby expanding access to safe motherhood services. - The voluntary nature encourages broader engagement of the private sector in public health objectives. *Incorrect: Statement 2 - The enrolled doctors must provide iron and folic acid tablets out of their pocket free to the beneficiaries.* - This is **incorrect**. In PPP maternal health programs, the government typically **supplies essential supplements** like **iron and folic acid (IFA)** tablets or provides reimbursement. - Requiring private providers to bear these costs out-of-pocket would be a significant **disincentive to participation** and contradict the partnership model. - The scheme aims to expand access while sharing resources between government and private sectors. *Incorrect: Statement 3 - The TT injections are provided by the District Medical Officers to the enrolled doctors for free administration to the beneficiaries.* - This statement is **partially correct in principle but not universally applicable** to all PPP maternal health schemes. - While government supply of **tetanus toxoid (TT)** vaccines to private facilities occurs in some programs, the specific mechanism of supply through District Medical Officers to enrolled private doctors is **not a standard feature** across all PPP schemes. - Many private providers source their own vaccines, with reimbursement mechanisms varying by scheme. *Incorrect: Statement 4 - To join the Vandemataram Scheme, the facility must have resources for caesarean section.* - This is **incorrect**. The **Vande Mataram Scheme** (integrated into broader maternal health initiatives) does **not mandate** that all participating facilities have **cesarean section capabilities**. - Smaller private clinics and individual practitioners can participate by providing **basic antenatal, natal, and postnatal care** services. - High-risk cases requiring C-sections are referred to facilities equipped for surgical interventions, following a **tiered care model**.
Question 112: Consider the following measures for making unlined katcha wells sanitary: 1. Deepening the bottom 2. Filling the well with clay up to the water level and with coarse sand above that level 3. Installing a hand pump with screen 4. Constructing a platform and drainage once the material used for filling is completely consolidated Which of the above measures are effective in making unlined katcha wells sanitary?
- A. 1, 2, 3 and 4 (Correct Answer)
- B. 2 and 3 only
- C. 1 and 2 only
- D. 1, 3 and 4 only
Explanation: ***1, 2, 3 and 4*** - All four measures are crucial for improving the **sanitary conditions** of unlined 'katcha' wells and preventing contamination. - These steps collectively address issues like surface water intrusion, subsurface filtration, and safe water extraction. *2 and 3 only* - This option is incomplete as it misses other vital steps like **deepening the bottom** to access cleaner water strata and **constructing a proper platform and drainage** to prevent surface contamination. - Focusing solely on filling and pump installation is insufficient for comprehensive well sanitation. *1 and 2 only* - This option overlooks the importance of installing a **hand pump with a screen** for hygienic water extraction and constructing a **platform with drainage** to prevent surface water runoff into the well. - Simply deepening and filling does not guarantee safe water delivery or protect against surface pollutants. *1, 3 and 4 only* - This option omits the critical step of **filling the well with clay and coarse sand**, which acts as a natural filter to remove impurities from the water as it seeps into the well. - Without proper filtration, deepening and surface protection alone may not ensure safe water quality.
Question 113: In which way is 'membrane filtration technique' better than 'multiple tube method' for determining the presence of coliform organisms in water?
- A. Membrane filtration technique is more universally available, and hence, easily doable.
- B. Membrane filtration technique is much quicker and results can be obtained within 20 hours, while multiple tube method is much longer. (Correct Answer)
- C. Membrane filtration technique can only be carried out by trained hands.
- D. Membrane filtration technique is far cheaper than multiple tube method.
Explanation: ***Membrane filtration technique is much quicker and results can be obtained within 20 hours, while multiple tube method is much longer.*** - The **membrane filtration technique** offers a significant advantage in terms of **turnaround time**, allowing for results within a single day. - This rapid result is crucial for **public health surveillance** and prompt intervention in case of contamination. *Membrane filtration technique is more universally available, and hence, easily doable.* - While widely used, the **availability** of specialized membrane filters and appropriate laboratory equipment can be a limiting factor in some settings. - Its perceived ease of implementation can be misleading, as proper sterile technique and sample handling are essential for accurate results. *Membrane filtration technique can only be carried out by trained hands.* - This statement is generally true for both methods; **trained personnel** are required to perform either technique accurately and reliably. - However, the expertise needed for interpreting growth patterns and confirming coliforms in the **multiple tube method** can be more involved. *Membrane filtration technique is far cheaper than multiple tube method.* - The **initial setup cost** for membrane filtration equipment can be higher than for the multiple tube method, although the cost per test might be lower in high-volume labs. - Cost comparisons often depend on the volume of samples processed and the ongoing expense of media and supplies for each method.
Question 114: Consider the following statements with reference to the National Framework for Malaria Elimination in India, 2016–2030. Which of the following statements is correct? 1. The goal is to eliminate indigenous cases throughout the country by 2030. 2. By 2022, transmission of malaria is to be interrupted and indigenous cases brought to zero in all 26 States/UTs that were under Categories 1 and 2 in 2014. 3. By 2026, incidence of malaria is to be reduced to less than 1 case per 1000 population in all States and UTs, and their districts. 4. By 2030, indigenous transmission of malaria is to be interrupted in all States and UTs of India.
- A. By 2026, incidence of malaria is to be reduced to less than 1 case per 1000 population in all States and UTs, and their districts.
- B. By 2022, transmission of malaria is to be interrupted and indigenous cases brought to zero in all 26 States/UTs that were under Categories 1 and 2 in 2014.
- C. The goal is to eliminate indigenous cases throughout the country by 2030. (Correct Answer)
- D. By 2030, indigenous transmission of malaria is to be interrupted in all States and UTs of India.
Explanation: ***The goal is to eliminate indigenous cases throughout the country by 2030.*** - This statement accurately reflects the primary overarching goal of the National Framework for Malaria Elimination in India, 2016–2030, which aims for the complete cessation of indigenous malaria cases nationwide by this target year. - The framework sets out a phased approach, with this ultimate goal guiding all intermediate targets and strategies. *By 2026, incidence of malaria is to be reduced to less than 1 case per 1000 population in all States and UTs, and their districts.* - The target of reducing **Annual Parasite Incidence (API)** to **less than 1 case per 1000 population** is actually set for **2024**, not 2026. - This specific target is an important **intermediate milestone** towards elimination, but the timeline provided is incorrect. *By 2022, transmission of malaria is to be interrupted and indigenous cases brought to zero in all 26 States/UTs that were under Categories 1 and 2 in 2014.* - The target for **Category 1 and 2 states/UTs** (those with low or no indigenous malaria cases in 2014) to achieve zero indigenous cases was set for **2020**, not 2022. - This phase focused on areas where elimination was considered more readily achievable due to lower disease burden. *By 2030, indigenous transmission of malaria is to be interrupted in all States and UTs of India.* - While the ultimate goal is elimination by 2030, the specific phrasing "indigenous transmission of malaria is to be interrupted" in all states and UTs is a step towards, but not the entirety of, the 2030 goal. - The **2030 goal is the elimination of indigenous cases**, implying sustained interruption of transmission in all areas.
Question 115: With reference to determinants of 'neonatal mortality', consider the following statements: 1. Neonatal mortality is directly related to the birth weight of the newborn. 2. Neonatal mortality is directly related to the gestational age at which the birth takes place. 3. Neonatal mortality is closely related to the educational status of the mother. 4. Neonatal mortality is low if the mother's age is between 15–16 years.
- A. 2. Neonatal mortality is directly related to the gestational age at which the birth takes place.
- B. 1. Neonatal mortality is directly related to the birth weight of the newborn.
- C. 4. Neonatal mortality is low if the mother's age is between 15–16 years.
- D. 3. Neonatal mortality is closely related to the educational status of the mother. (Correct Answer)
Explanation: ***Statement 3: Neonatal mortality is closely related to the educational status of the mother.*** - This statement is **CORRECT**. - Higher **maternal education** is consistently associated with better health-seeking behaviors, improved nutrition, and greater access to healthcare, leading to significantly lower neonatal mortality rates. - Educated mothers are more likely to understand and practice good hygiene, recognize danger signs in newborns, and adhere to recommended medical interventions, all of which contribute to reduced neonatal deaths. *Statement 1: Neonatal mortality is directly related to the birth weight of the newborn.* - This statement is **INCORRECT**. - Neonatal mortality is **inversely related** to birth weight, not directly related. - **Lower birth weight** is associated with a **higher risk of neonatal mortality**. - Low birth weight often signifies prematurity or intrauterine growth restriction, both of which are major risk factors for neonatal death due to complications like respiratory distress syndrome, infections, and hypothermia. *Statement 2: Neonatal mortality is directly related to the gestational age at which the birth takes place.* - This statement is **INCORRECT**. - Neonatal mortality is **inversely related** to gestational age, not directly related. - The **lower the gestational age (preterm birth)**, the **higher the neonatal mortality rate**. - Infants born extremely preterm face significant challenges due to underdeveloped organs and systems, increasing their risk of mortality. *Statement 4: Neonatal mortality is low if the mother's age is between 15–16 years.* - This statement is **INCORRECT**. - Neonatal mortality is generally **higher** in infants born to mothers in this **young age group** (15-16 years) compared to optimal maternal age groups (e.g., 20s or early 30s). - Adolescent mothers are more likely to experience **complications during pregnancy and childbirth**, have less access to adequate prenatal care, and possess fewer resources for infant care, all of which contribute to elevated neonatal mortality rates.
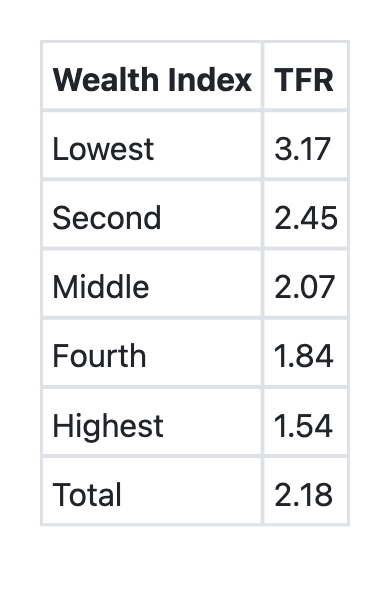
Question 116: The following table shows the 'Total Fertility Rate (TFR)' by the Wealth Index, as per the National Family Health Survey, (NFHS–4) findings. Which among the following is/are correct about the information?
- A. 2. The information given in the table can be presented as a pie chart.
- B. 4. Each of the higher divisions of the Wealth Index had lower TFR than the previous (or lower) division. (Correct Answer)
- C. 1. The divisions of Wealth Index in the NFHS–4 can be called 'quartiles'.
- D. 3. The Wealth Index was calculated in NFHS–4 by asking about the per capita income.
Explanation: ***Each of the higher divisions of the Wealth Index had lower TFR than the previous (or lower) division.*** - Examining the table data: Lowest (3.17), Second (2.45), Middle (2.07), Fourth (1.84), Highest (1.54) - The **Total Fertility Rate consistently decreases** as the wealth index category increases from lowest to highest - This demonstrates an **inverse relationship between wealth and fertility**, a well-established demographic pattern - Each successive higher wealth category shows a lower TFR than the previous category without exception *The divisions of Wealth Index in the NFHS–4 can be called 'quartiles'.* - The table divides the population into **five wealth index categories**: Lowest, Second, Middle, Fourth, and Highest - When a population is divided into five equal groups, these are called **quintiles**, not quartiles - **Quartiles** would divide the population into four groups (25th, 50th, 75th, 100th percentiles) - **Quintiles** divide the population into five groups (20th, 40th, 60th, 80th, 100th percentiles) *The information given in the table can be presented as a pie chart.* - A **pie chart** is used to show parts of a whole, representing proportions or percentages that sum to 100% - The data shows **Total Fertility Rate (TFR)** values for different wealth categories, which are rates (average births per woman), not proportions - TFR values don't sum to a meaningful total and don't represent parts of a whole - This data is better presented as a **bar chart or line graph** to show the trend across wealth categories *The Wealth Index was calculated in NFHS–4 by asking about the per capita income.* - The **Wealth Index** in NFHS surveys is calculated using **principal component analysis** of household assets and characteristics - It includes: consumer durables (TV, refrigerator, vehicles), housing characteristics (flooring type, wall material, roof type), water source, sanitation facilities, cooking fuel, and livestock ownership - **Per capita income is NOT used** because it's difficult to measure accurately in informal economies, has seasonal variations, and suffers from recall bias and underreporting - Asset-based wealth indices are considered more reliable proxies for socioeconomic status in developing countries
Obstetrics and Gynecology
1 questionsAs per the definition of the World Health Organization, 'late maternal death' is defined as the death of a woman from direct or indirect obstetric causes, after more than X days but less than one year after termination of pregnancy. Which one among the following is the correct value of X?
UPSC-CMS 2022 - Obstetrics and Gynecology UPSC-CMS Practice Questions and MCQs
Question 111: As per the definition of the World Health Organization, 'late maternal death' is defined as the death of a woman from direct or indirect obstetric causes, after more than X days but less than one year after termination of pregnancy. Which one among the following is the correct value of X?
- A. 21
- B. 7
- C. 84
- D. 42 (Correct Answer)
Explanation: ***Correct: 42*** - According to the **World Health Organization (WHO)**, **late maternal death** is defined as the death of a woman from direct or indirect obstetric causes occurring **more than 42 days** but less than one year after termination of pregnancy. - This definition helps in categorizing and understanding the timeframe and causes of maternal mortality beyond the immediate postpartum period. - The **42-day threshold** distinguishes between direct maternal deaths (within 42 days) and late maternal deaths (42 days to 1 year). *Incorrect: 21* - This value is not used in the WHO definition for the onset of late maternal death. - The **42-day mark** is the internationally recognized threshold for distinguishing between the immediate postpartum period and late maternal complications. *Incorrect: 7* - Seven days is too short a period for a death to be classified as **"late maternal death"**; deaths within this timeframe fall under **direct maternal deaths** in the immediate postpartum period. - This period is often associated with immediate postpartum complications such as **postpartum hemorrhage**, **eclampsia**, or **early-onset puerperal sepsis**. *Incorrect: 84* - While 84 days (12 weeks) is a significant period in postpartum recovery for some physiological changes, it is not the specific threshold used by the **WHO** to define the beginning of **late maternal death**. - The international standard remains **42 days** (6 weeks) as the transition point between direct and late maternal deaths.
Pathology
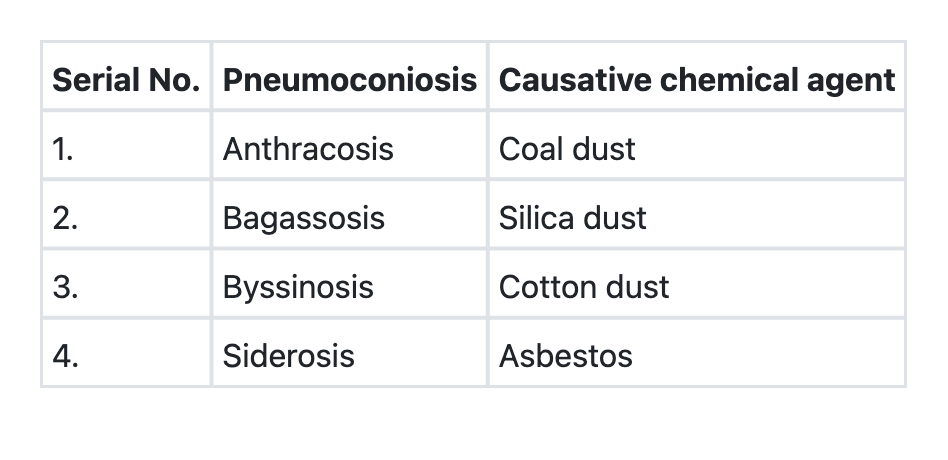
1 questionsThe following table shows some of the pneumoconioses diseases along with the most implicated causative chemical agents. Which among the following represent the correct combinations of diseases and causative chemical agents? Select the correct answer using the code given below.

UPSC-CMS 2022 - Pathology UPSC-CMS Practice Questions and MCQs
Question 111: The following table shows some of the pneumoconioses diseases along with the most implicated causative chemical agents. Which among the following represent the correct combinations of diseases and causative chemical agents? Select the correct answer using the code given below.
- A. 2 and 4
- B. 2 and 3
- C. 1 and 3
- D. 1 and 2 (Correct Answer)
Explanation: ***Correct: 1 and 2*** - **Statement 1 (Anthracosis - Coal dust)** is correct. Anthracosis, also known as **coal worker's pneumoconiosis**, is caused by chronic inhalation of coal dust particles [1]. - **Statement 2 (Byssinosis - Cotton dust)** is correct. Byssinosis is an occupational lung disease affecting **textile workers** exposed to cotton, flax, or hemp dust, causing airway obstruction. *Incorrect: 2 and 4* - Statement 4 is incorrect. **Siderosis** is caused by inhalation of **iron dust** (common in welders and miners), not asbestos [1]. Asbestos exposure causes **asbestosis** [1]. *Incorrect: 2 and 3* - Statement 3 is incorrect. **Bagassosis** is caused by inhalation of **sugarcane bagasse dust** (a hypersensitivity pneumonitis), not silica dust [1]. Silica causes **silicosis** [1]. *Incorrect: 1 and 3* - While statement 1 is correct (Anthracosis - Coal dust), statement 3 is incorrect as explained above (Bagassosis is caused by sugarcane bagasse dust, not silica dust) [1]. **References:** [1] Kumar V, Abbas AK, et al.. Robbins and Cotran Pathologic Basis of Disease. 9th ed. The Lung, p. 695.
Pediatrics
1 questionsIn a newborn, the Apgar score has been recorded at 1 minute of birth. Which one of the following best reflects the Apgar score of this newborn infant on a scale of 0 to 10?
UPSC-CMS 2022 - Pediatrics UPSC-CMS Practice Questions and MCQs
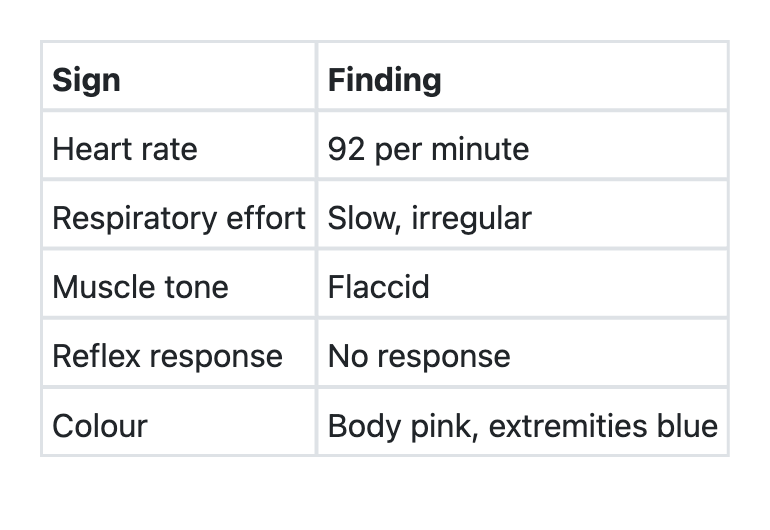
Question 111: In a newborn, the Apgar score has been recorded at 1 minute of birth. Which one of the following best reflects the Apgar score of this newborn infant on a scale of 0 to 10?
- A. 3 (Correct Answer)
- B. 2
- C. 0
- D. 5
Explanation: ***3*** - The Apgar score is calculated based on five criteria: **Appearance**, **Pulse**, **Grimace**, **Activity**, and **Respiration** (APGAR). Each criterion is scored 0, 1, or 2. - Based on the given findings: - **Heart rate (Pulse)**: 92/min scores **1** (below 100/min). - **Respiratory effort (Respiration)**: Slow, irregular scores **1**. - **Muscle tone (Activity)**: Flaccid scores **0**. - **Reflex response (Grimace)**: No response scores **0**. - **Colour (Appearance)**: Body pink, extremities blue (acrocyanosis) scores **1**. - Summing these scores (1 + 1 + 0 + 0 + 1) gives a total Apgar score of **3**. *2* - This score would mean that the newborn has a **more severe depression** in vital signs compared to the actual findings. - A score of 2 would require at least one of the 1-point criteria to be a 0-point criterion or combination of a 0-point criterion become 1. *0* - An Apgar score of 0 would indicate that the infant has **no vital signs** (no heart rate, no respiratory effort, no muscle tone, no reflex response, and completely blue/pale). - This is not consistent with a heart rate of 92/min, slow/irregular respirations, and body pink color. *5* - An Apgar score of 5 would imply a **much healthier** newborn with better scores in most categories. - This would require findings such as a heart rate over 100 bpm, good crying, some flexion of extremities, or an all-pink appearance, which are not present here.