What is the shelf life of Dukoral (wc-rBS) oral vaccine used for cholera prevention, when stored at a temperature of 2 °C to 8 °C?
Which of the following are correct in respect of incidence rate? 1. It is a sum total of new and old cases. 2. It refers to a specified period of time. 3. It refers to a defined population. 4. It must include the unit of time in final expression.
Forty patients with diarrhoeal diseases were studied. Their age distribution is given in the table below : What is the mean age of the patients in this study?
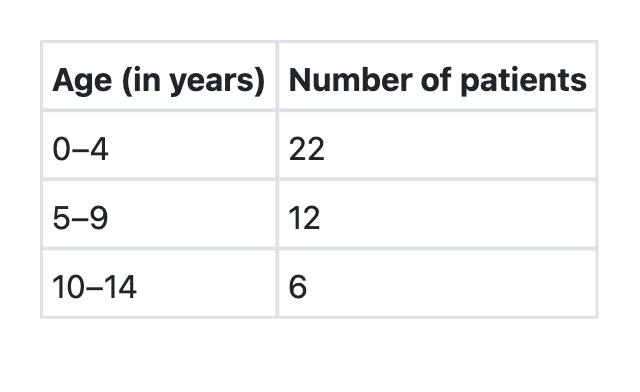
Which of the following international agencies focuses on sustainable development programming that includes health as a key component?
Which of the following statements is true about 'End TB Strategy'?
Consider the protein content of the following food items (in terms of grams per 100 grams of food) : 1. Cow milk 2. Meat 3. Soya bean 4. Sugar What is the correct descending order (highest to lowest) of protein content?