Medical management of tubal ectopic pregnancy can be done in the following EXCEPT:
Which of the following genital infections is associated with preterm labour?
Multiple pregnancy is associated with an increased incidence of the following EXCEPT:
Surgical staging is done for all the genital malignancies EXCEPT:
B-Lynch suture for atonic postpartum haemorrhage:
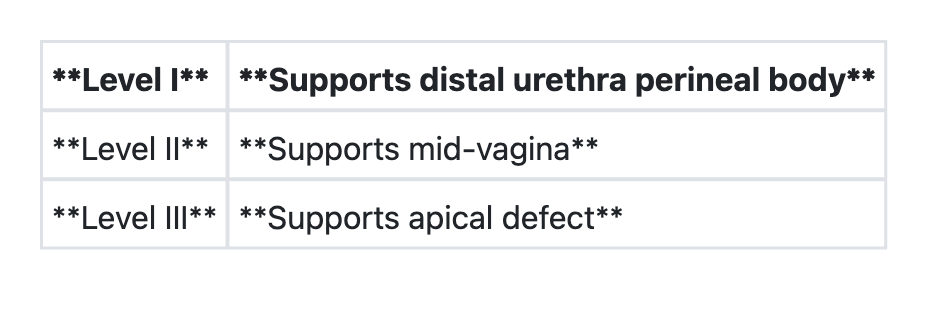
Regarding 'DeLancey's levels of vaginal support', consider the following pairs:
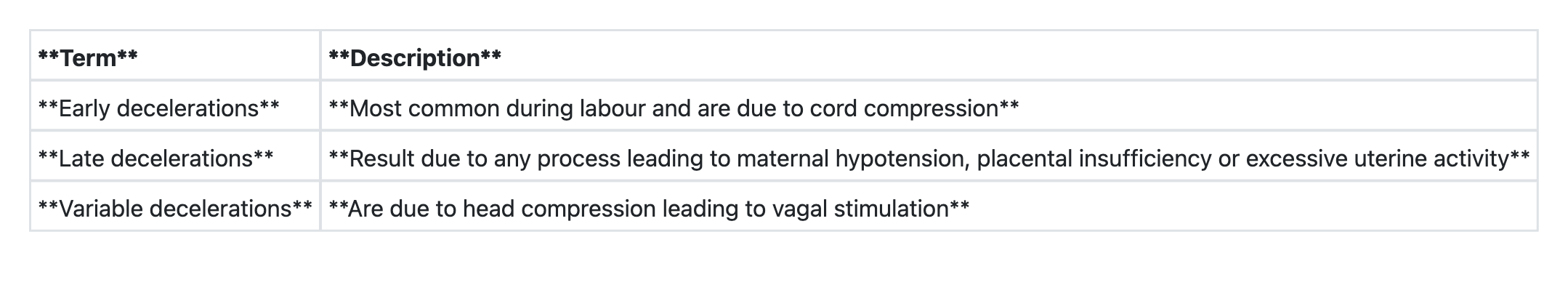
Consider the following pairs regarding foetal heart during labour: