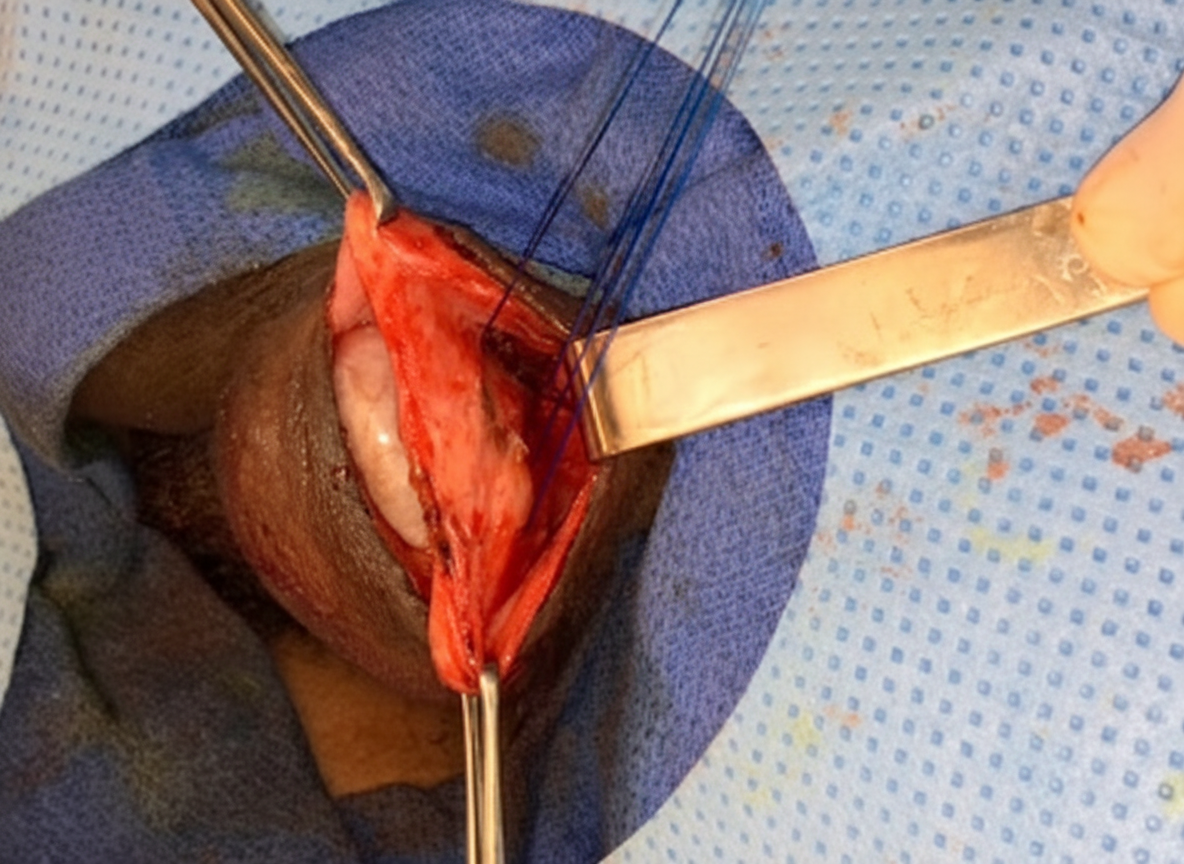
What is correct regarding this suture?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A 46-year-old woman presents with complaints of irregular menstrual cycles and heavy vaginal bleeding for several months. Transvaginal ultrasound reveals an endometrial thickness of 16 mm. What is the most appropriate next step in management?
In managing shoulder dystocia during vaginal delivery, which of the following is the correct sequence of maneuvers?
A 36-year-old woman presents with secondary amenorrhea for the past 8 months. Laboratory investigations reveal FSH of 36 IU/L and AMH of 0.05 ng/mL. What is the most likely diagnosis?
An elderly patient presents with white, dandruff-like deposits on the anterior lens surface, seen during slit-lamp examination. What is the most likely diagnosis?
Which condition is treated using an Intacs ring, as shown in the image?
The essential foundational components of binocular single vision are:
Which of the following is true about orbital cellulitis?
By what primary mechanism does hydrochlorothiazide help prevent the formation of calcium stones?
History of pulsatile mass in the neck. Digital angiography image shown. Not filling on carotid compression. But refilling on releasing pressure. What is the diagnosis?
What is correct regarding this suture?
