A male patient is not responding to oxygen therapy and has been diagnosed with ARDS (Acute Respiratory Distress Syndrome). What is the role of IL-8 in ARDS?
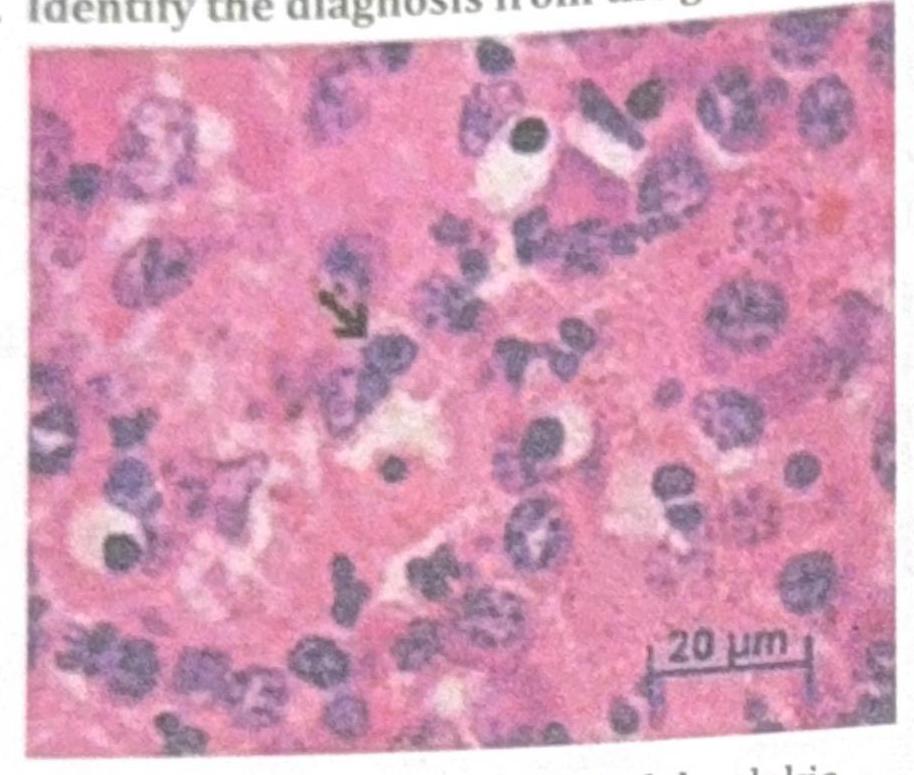
Identify the diagnosis from the given image
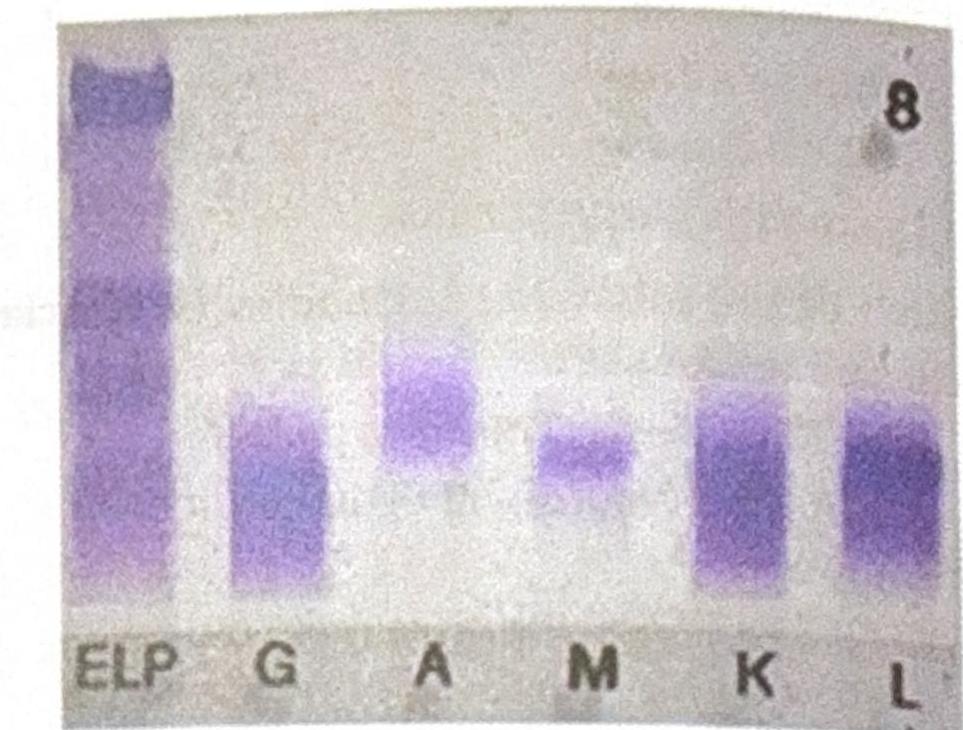
An elderly male patient presented with clinical symptoms and signs consistent with possible multiple myeloma. Electrophoresis shows an M spike, and immunofixation findings are shown below. Which of the following statements best corresponds to the findings?
Which of the following is an intracellular marker or deposition found in Alzheimer's disease?
A child presenting with leukocoria has an intraocular mass. Microscopic examination shows rosettes with scanty cytoplasm and positive synaptophysin. What is the most likely diagnosis?
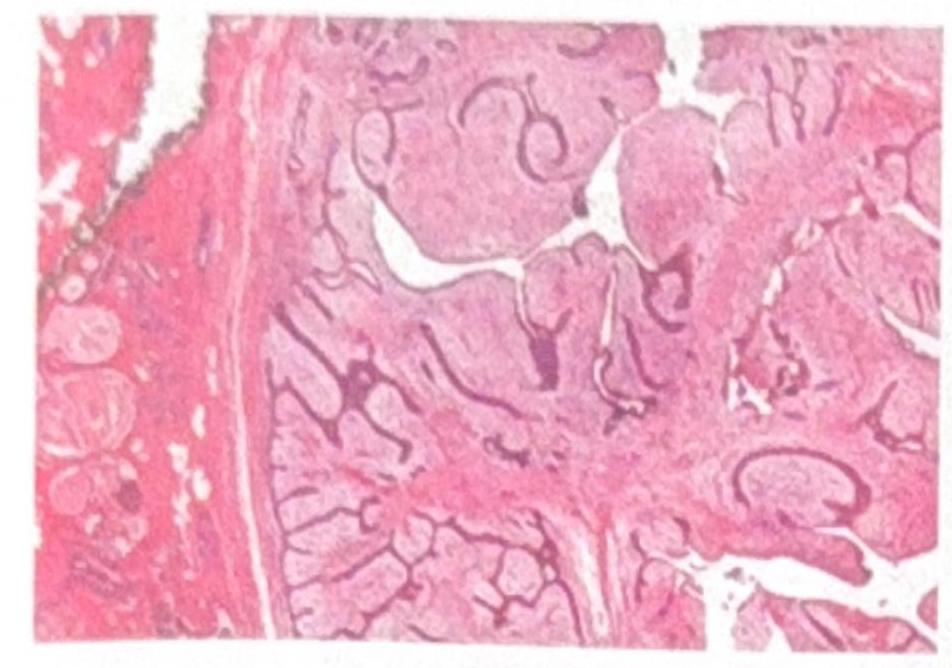
A 40-year-old female presents with an irregular 5 × 6 cm mass in the right breast. Histopathological examination reveals the image shown. What is the most likely diagnosis?