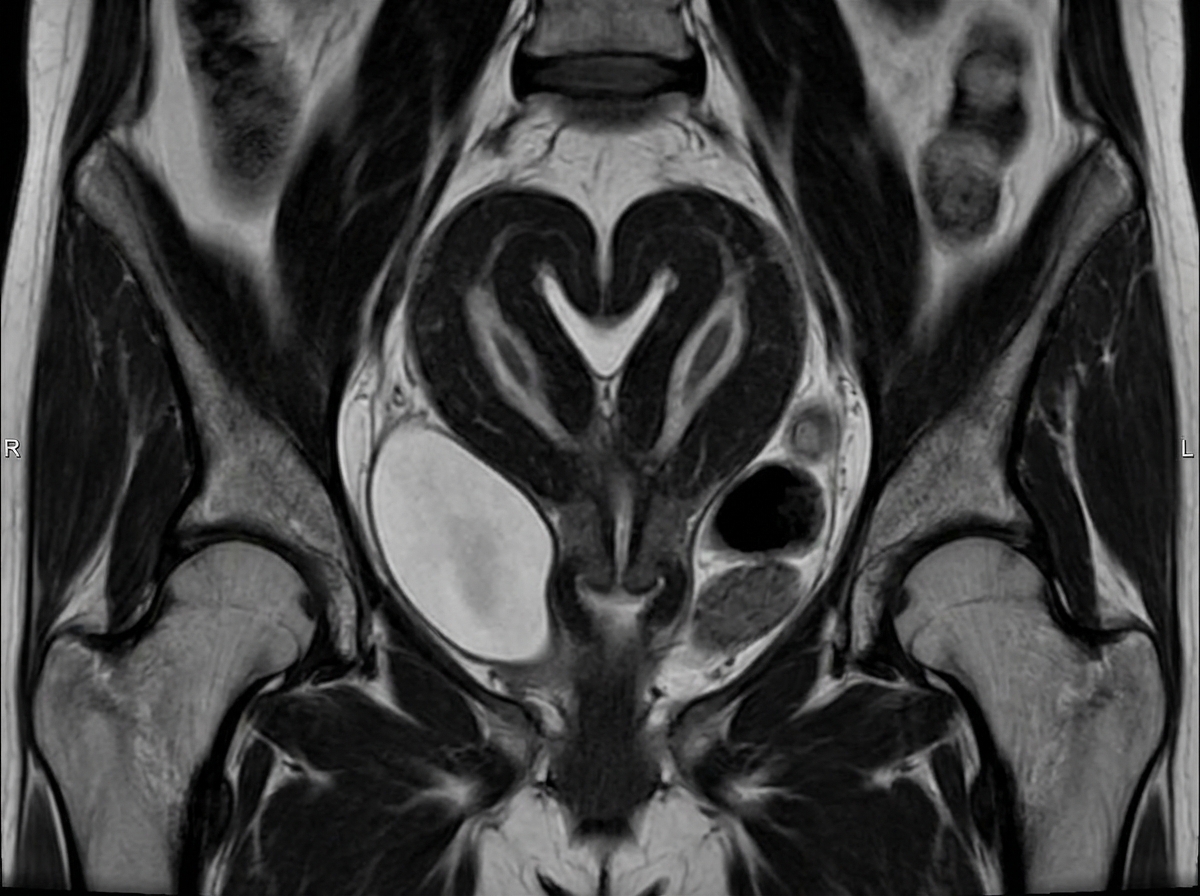
Identify the uterus shown in the image?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Identify the uterus shown in the image?

What is the typical time between fertilization and implantation?
A pregnant woman with a known case of asthma is experiencing postpartum hemorrhage (PPH). Which drug is contraindicated?
In fertility-preserving prolapse surgery, which bony landmark is used for suspension?
A 45-year-old woman presents with a history of cervical erosion and spotting for the past 2 months. What is the next best step?
Identify the instrument shown in the image below:

Which of the following is not a contraindication for External Cephalic Version (ECV)?
A 30-year-old female, G2L2, with a history of cervical elongation presents for surgical consultation. What is the surgery of choice?
A pregnant woman presents with an IUD in place, and the thread is clearly visible. She wishes to continue the pregnancy. What is the most appropriate next step?
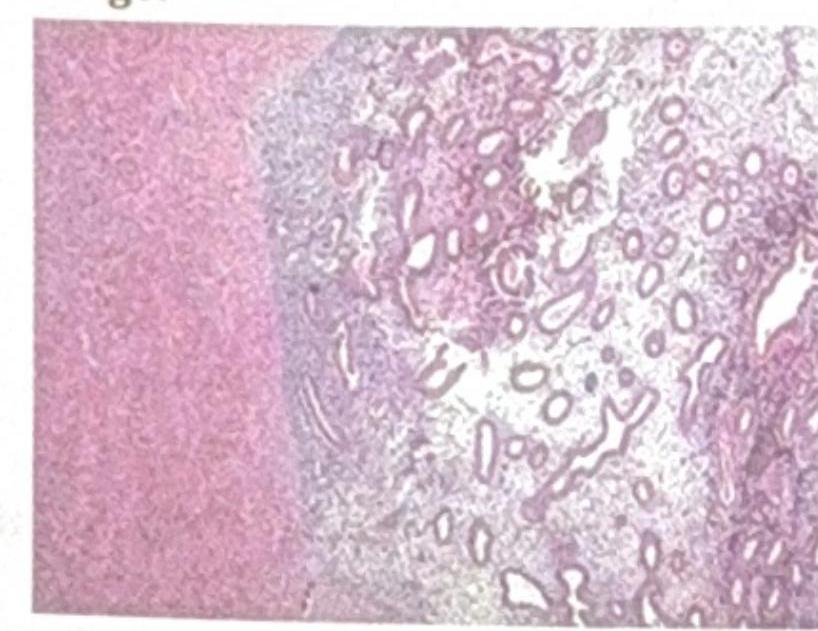
Identify the pathological condition shown in the image: