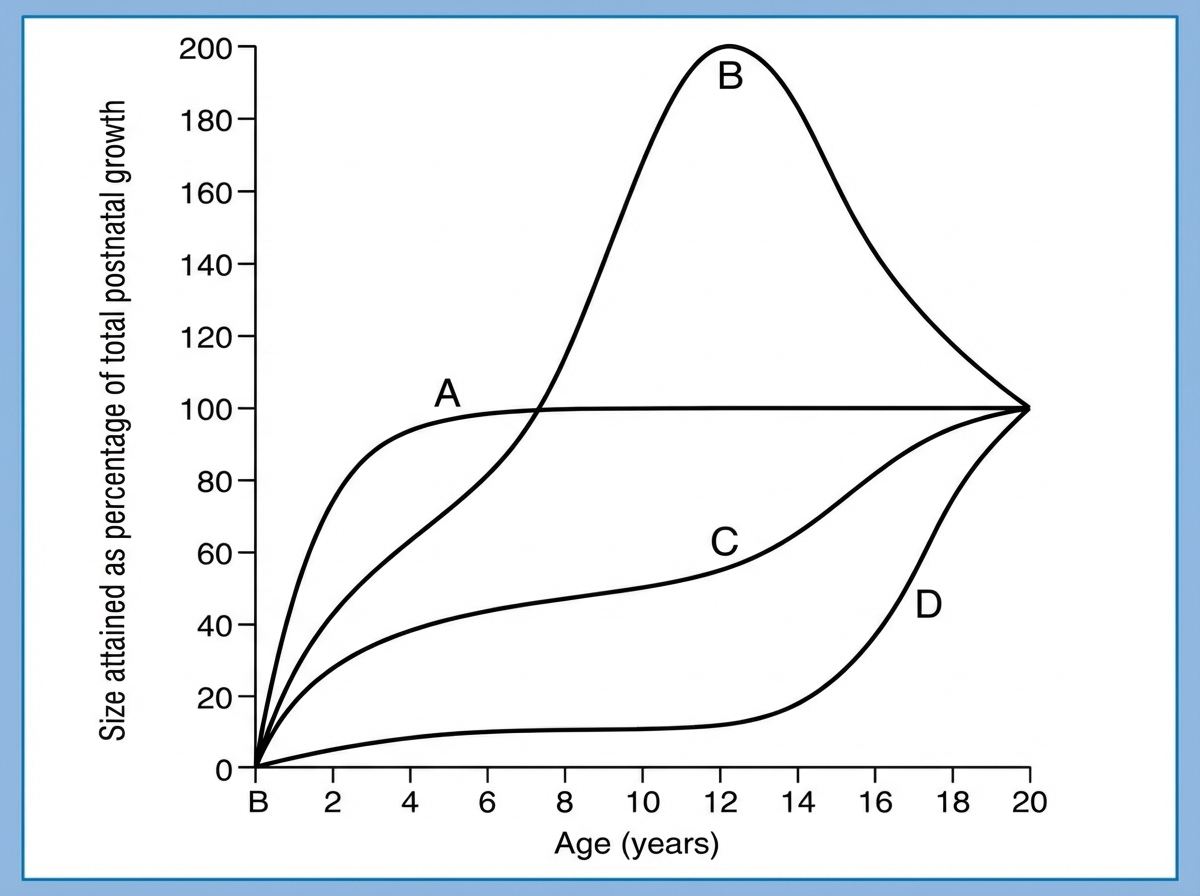
At what age does maximum brain growth occur?
The Image shows the growth curve of different organs with age. Identify A in the graph
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
At what age does maximum brain growth occur?
The Image shows the growth curve of different organs with age. Identify A in the graph

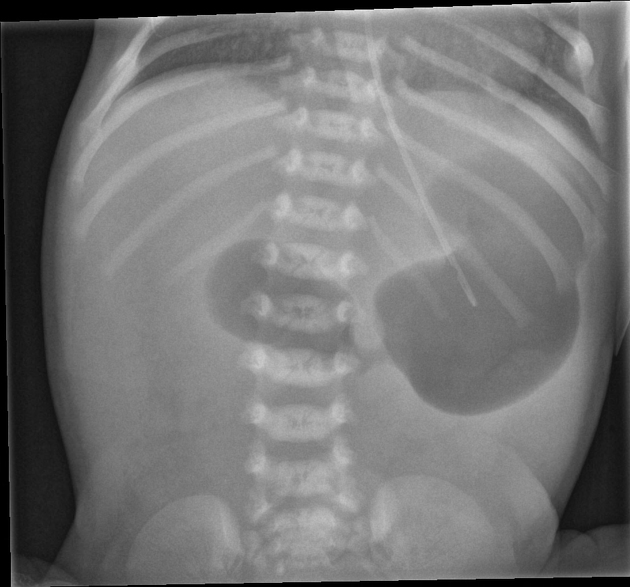
An infant presents with vomiting after feeding. Benedict's test was positive for a non-glucose reducing substance. What is the most likely diagnosis?
Which disease will show the mode of inheritance depicted in this pedigree?
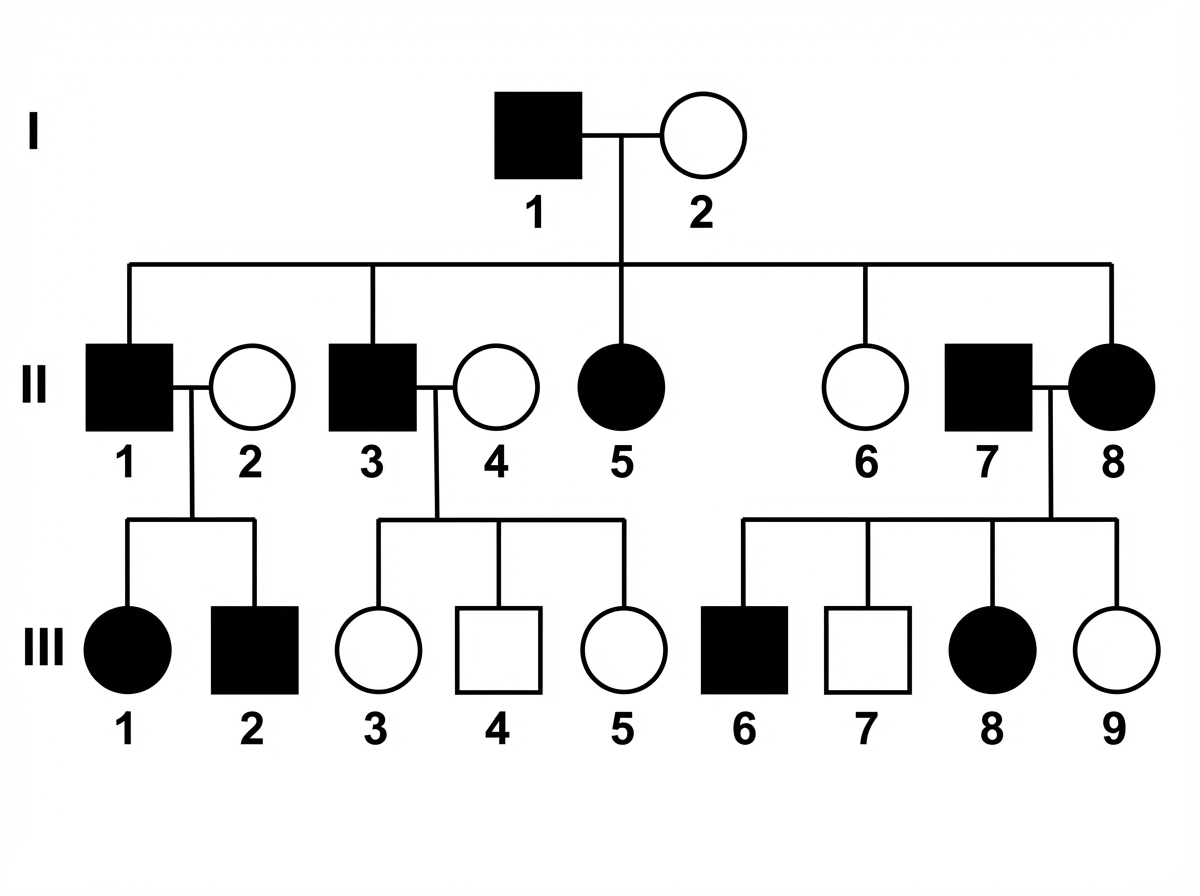
A mother brings her 14 -year-old mentally retarded son to the OPD, who is suffering from joint pain and has an irresistible urge to bite his fingers and lips. His serum uric acid level was found to be elevated. What is the disorder?
The flexion point in ventouse (vacuum) delivery is located at:
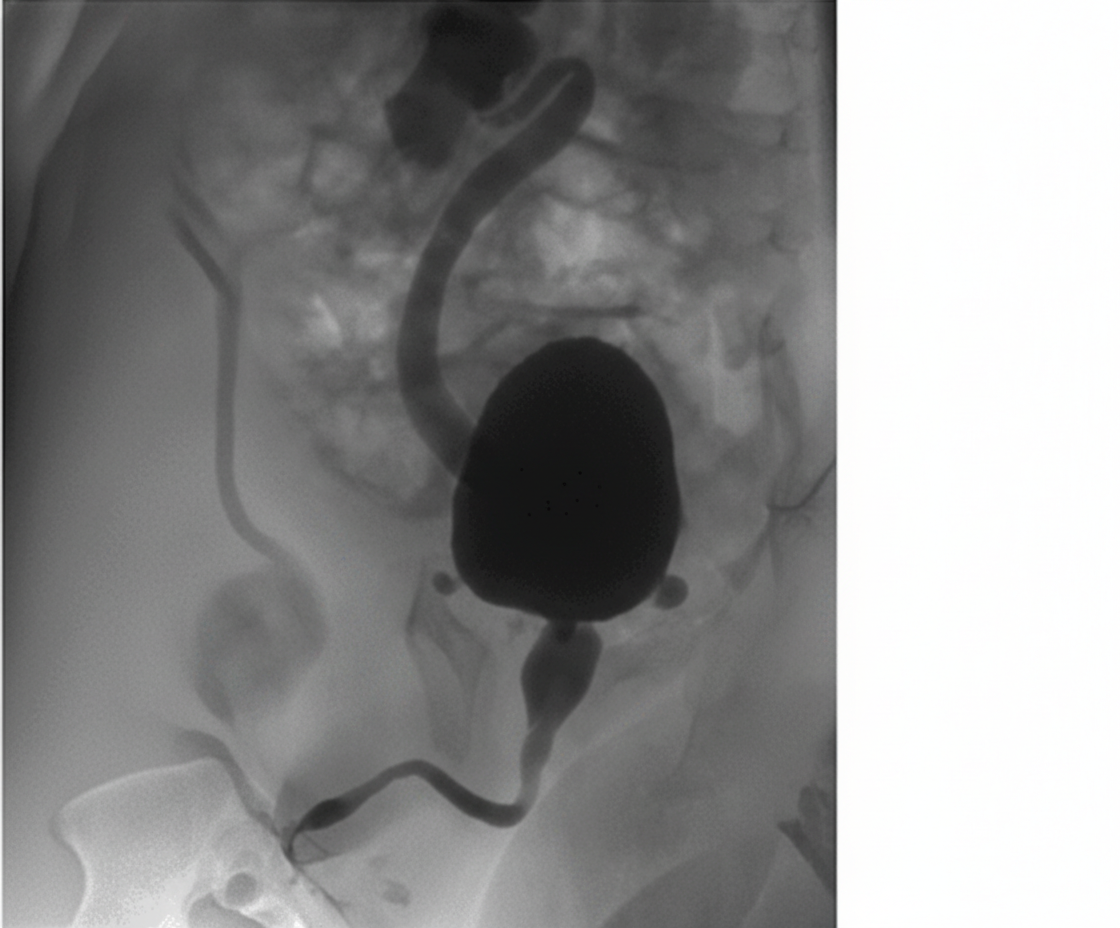
A 3-year-old child presents to the OPD with a history of recurrent urinary tract infections, poor urinary stream, and difficulty voiding. The radiological image is shown below. What is the most appropriate management?
An unimmunized 5 -year-old child presents to the OPD with a white membranous layer on the throat upon inspection. The child's brother is immunized. What is the first step in management?
An unimmunized 5 -year-old child presents to the OPD with a white membranous layer on inspection, suggesting diphtheria. What is the appropriate prophylaxis for a 2 -year-old contact who has completed their vaccination?
A 6-week-old baby is brought in by the mother with complaints of vomiting. An X-ray shows a single bubble appearance. What is the most likely diagnosis?