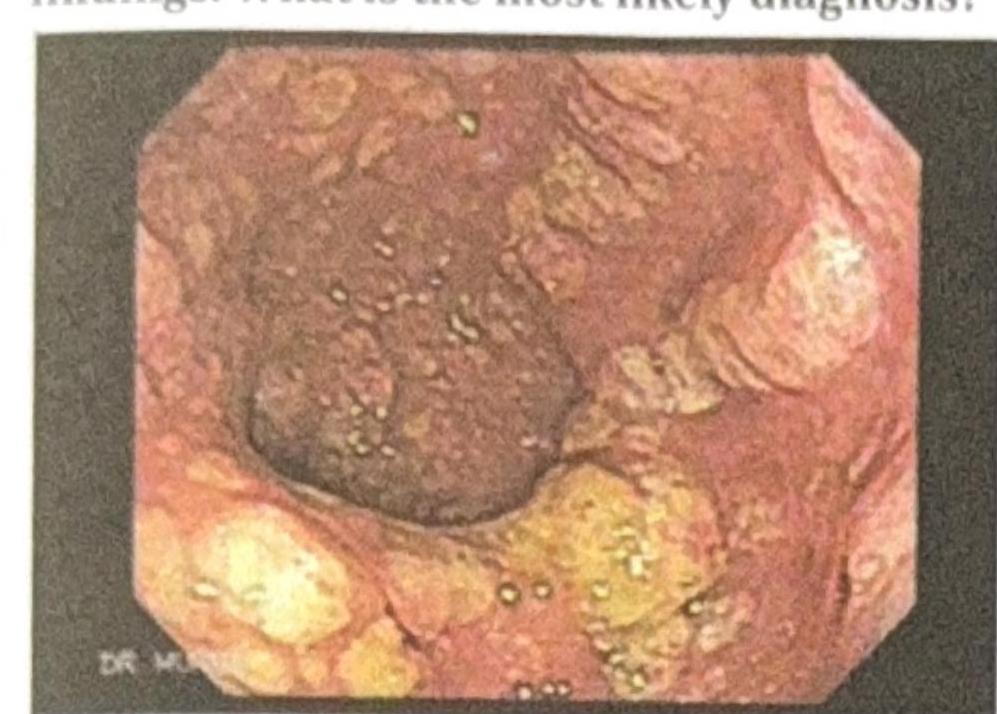
A patient presents to the OPD with recurrent diarrhea, abdominal pain, and foul-smelling stools. The colonoscopy reveals the following findings. What is the most likely diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
What is the most appropriate initial investigation for a solitary thyroid nodule (STN)?
A female presents with a 1 × 1 cm thyroid swelling. What is the next best step in management?
A patient presents to the OPD with recurrent diarrhea, abdominal pain, and foul-smelling stools. The colonoscopy reveals the following findings. What is the most likely diagnosis?

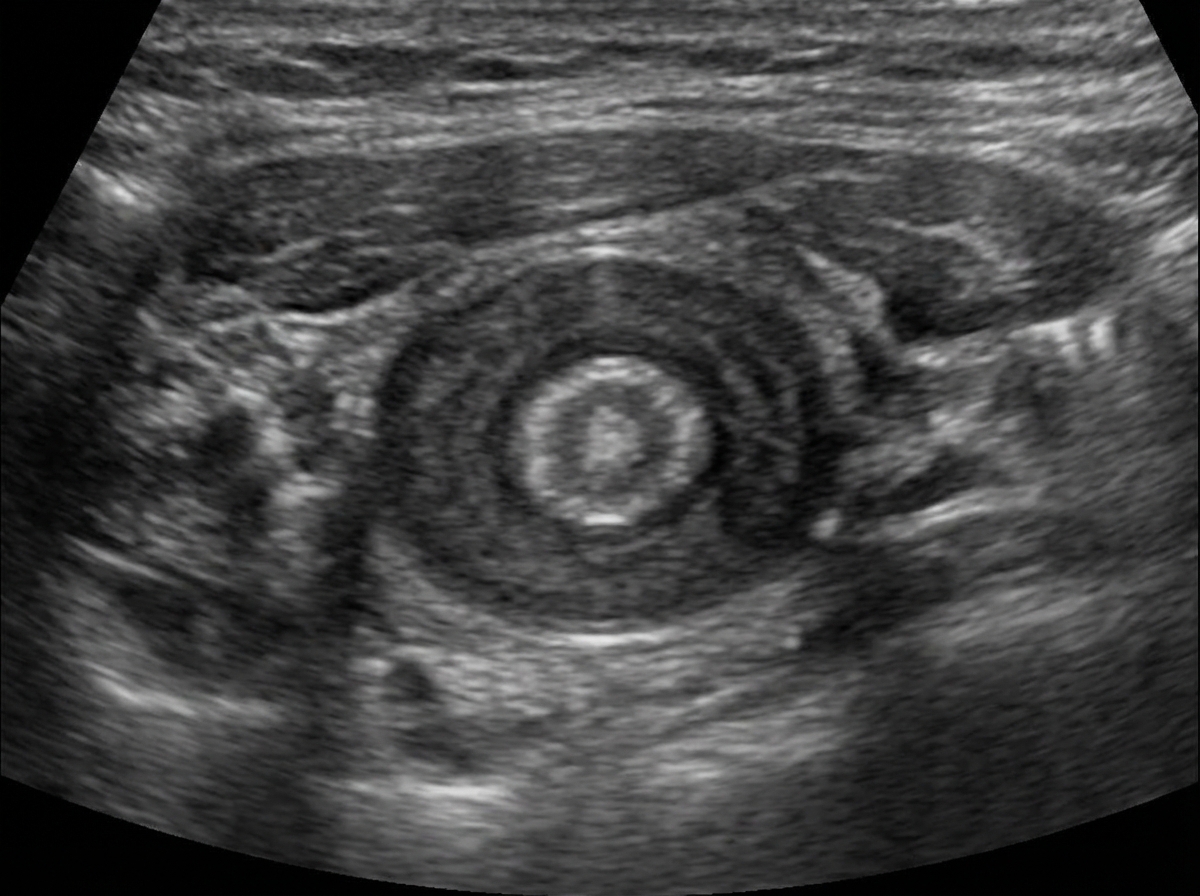
A 6-week-old child with a history of vomiting undergoes an ultrasound, which shows an antral nipple sign or target sign, as shown in the image. What is the diagnosis?
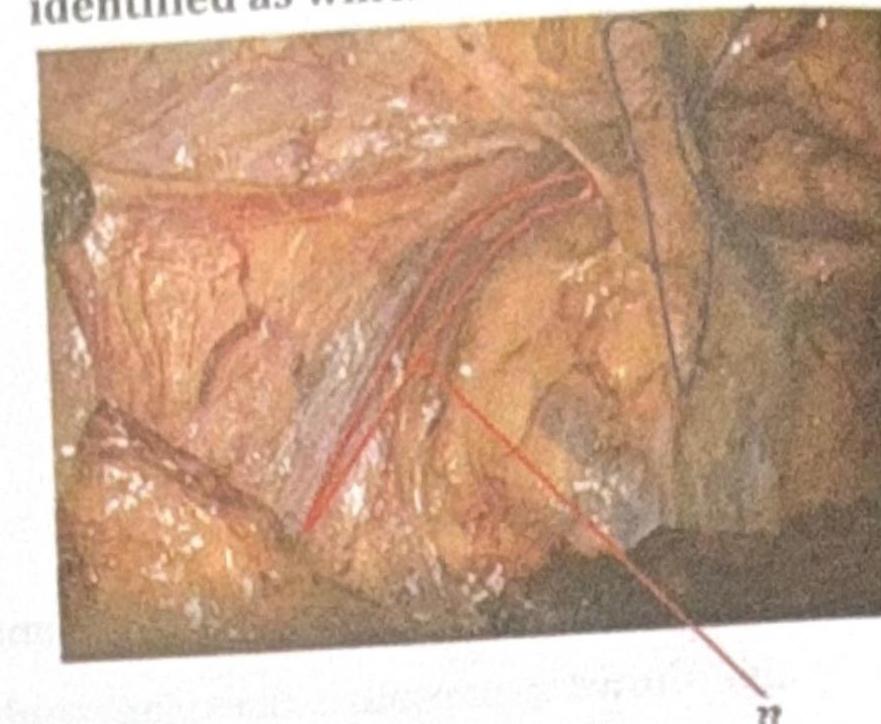
In the intraoperative image of congenital hernia repair, the structure marked by the red arrow is identified as which of the following?
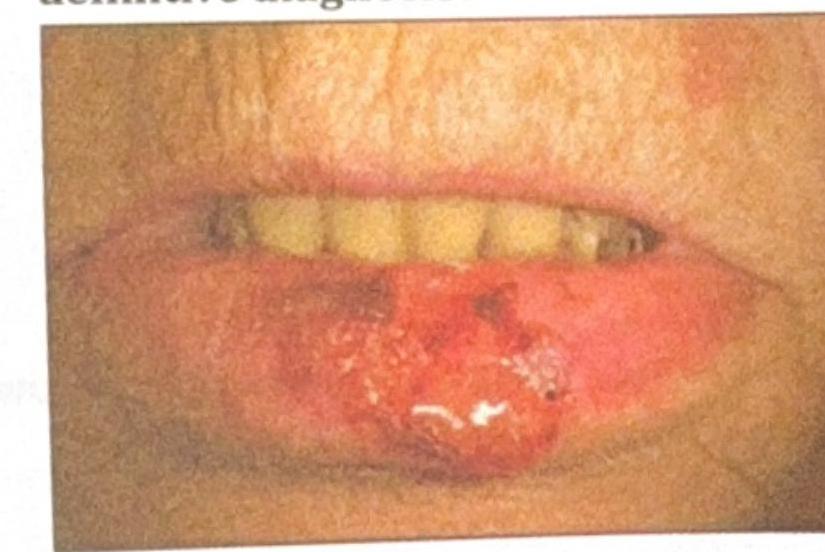
An elderly patient presents with a non-healing ulcerative lesion on the lower lip, as shown in the image. The lesion has been gradually enlarging over the past few months. Suspecting squamous cell carcinoma (SCC), what is the most appropriate method to obtain a biopsy for definitive diagnosis?
How does a skin graft receive nutrition on day 3 after transplantation?
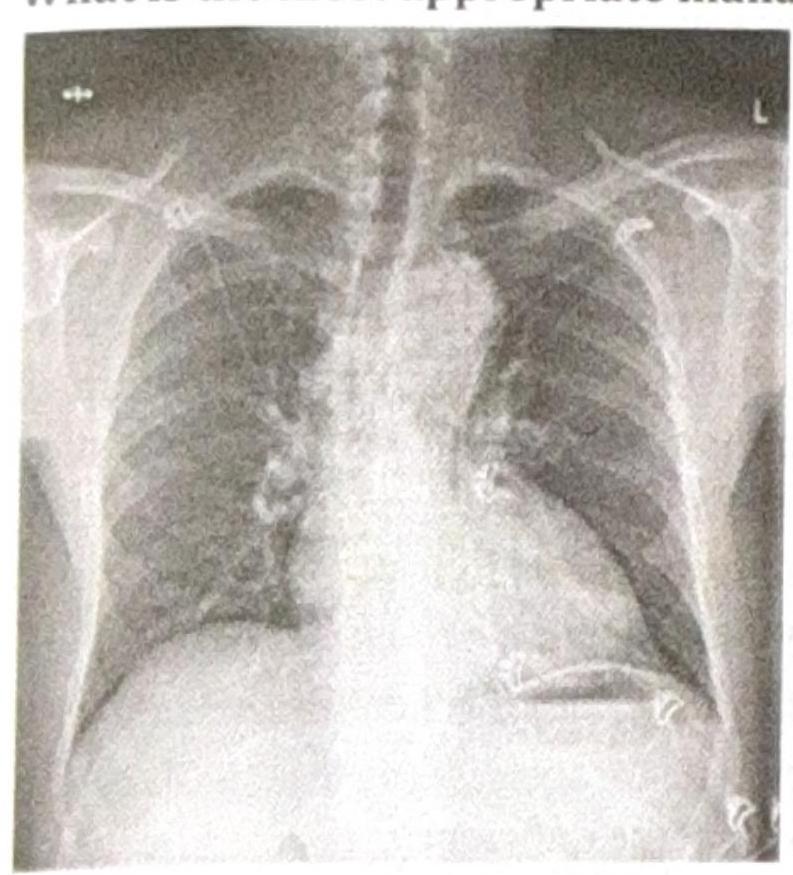
A patient presents with constant chest pain, and the radiological finding is as shown in the image. What is the most appropriate management?
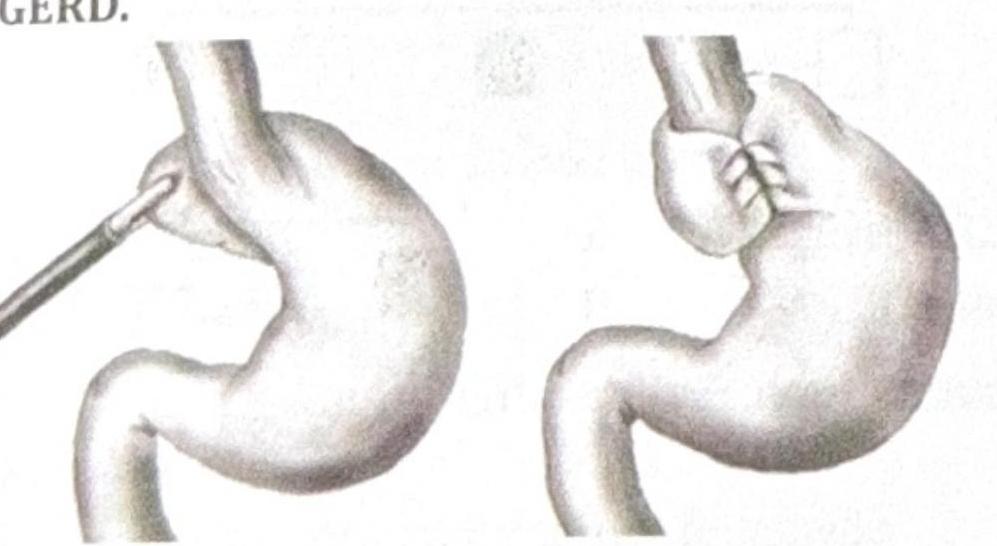
Identify the procedure shown in the image, which is performed in a patient with recurrent GERD.
A patient presents with a penile lesion staged as T3, with clinically palpable lymph nodes. What is the most appropriate management?