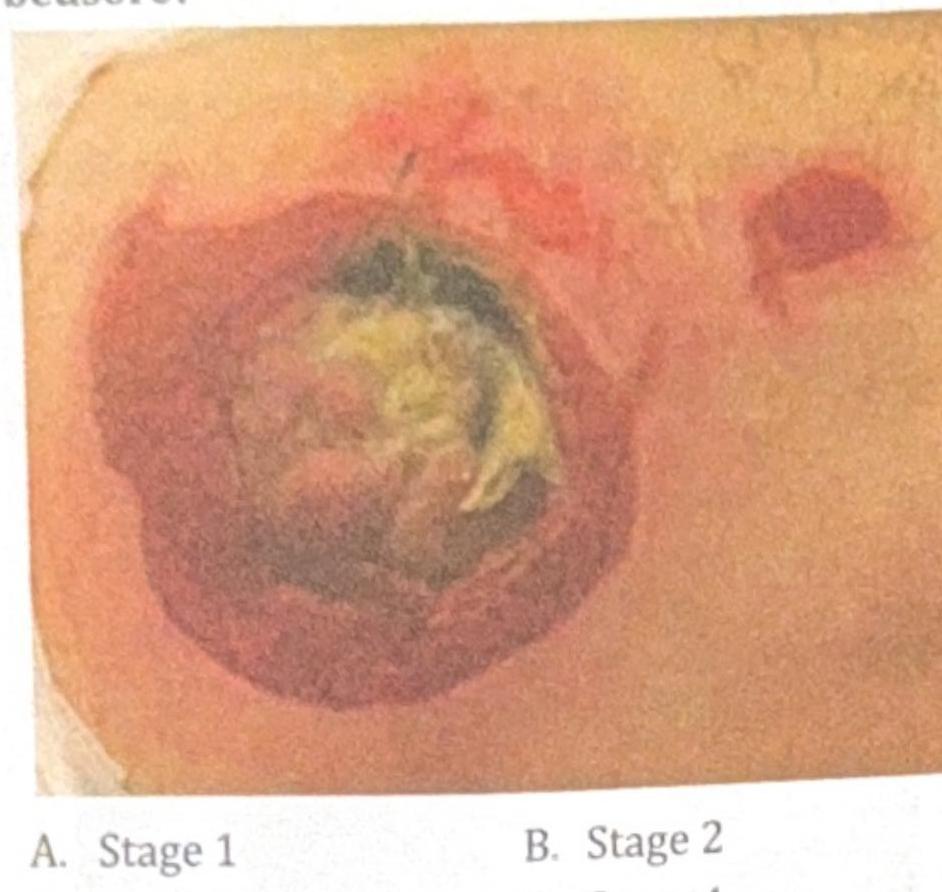
A young patient presents to the OPD with recurrent colicky abdominal pain. Urine examination shows the presence of red blood cells (RBCs) and the following crystal shape in the figure. What is the most likely diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A young patient presents to the OPD with recurrent colicky abdominal pain. Urine examination shows the presence of red blood cells (RBCs) and the following crystal shape in the figure. What is the most likely diagnosis?

A patient presents with large sweaty hands, macroglossia, and frontal bossing. What is the best test for confirmation of the diagnosis?
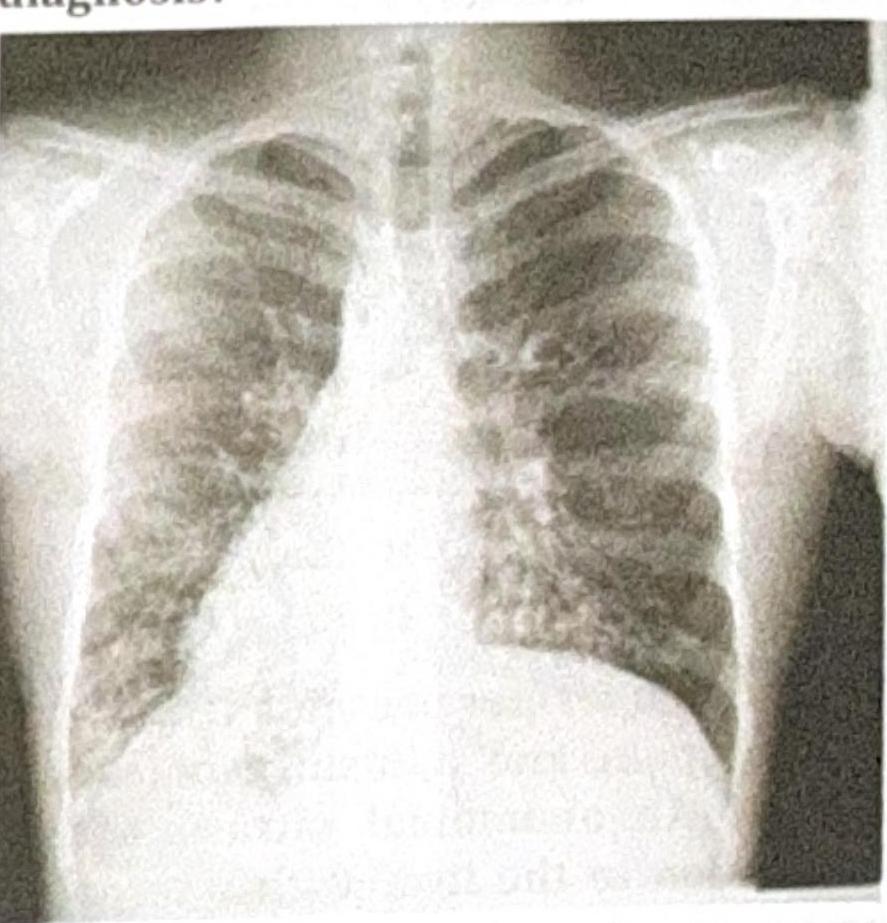
A patient presents with recurrent lung infections, and the chest X-ray provided shows a characteristic finding. What is the most likely diagnosis?
Which of the following statements regarding von Willebrand disease is incorrect?
A patient presents with headache, confusion, and a diagnosis of a brain tumor. The family history reveals brain and kidney tumors. What is the most likely diagnosis?
A 26-year-old woman presents to the OPD with distended neck veins and difficulty in breathing. On further evaluation, the patient is diagnosed with myasthenia gravis. Radiological imaging reveals an anterior mediastinal mass on CT. What is the most likely diagnosis?
A patient underwent a gastrectomy. Which vitamin replacement is required?
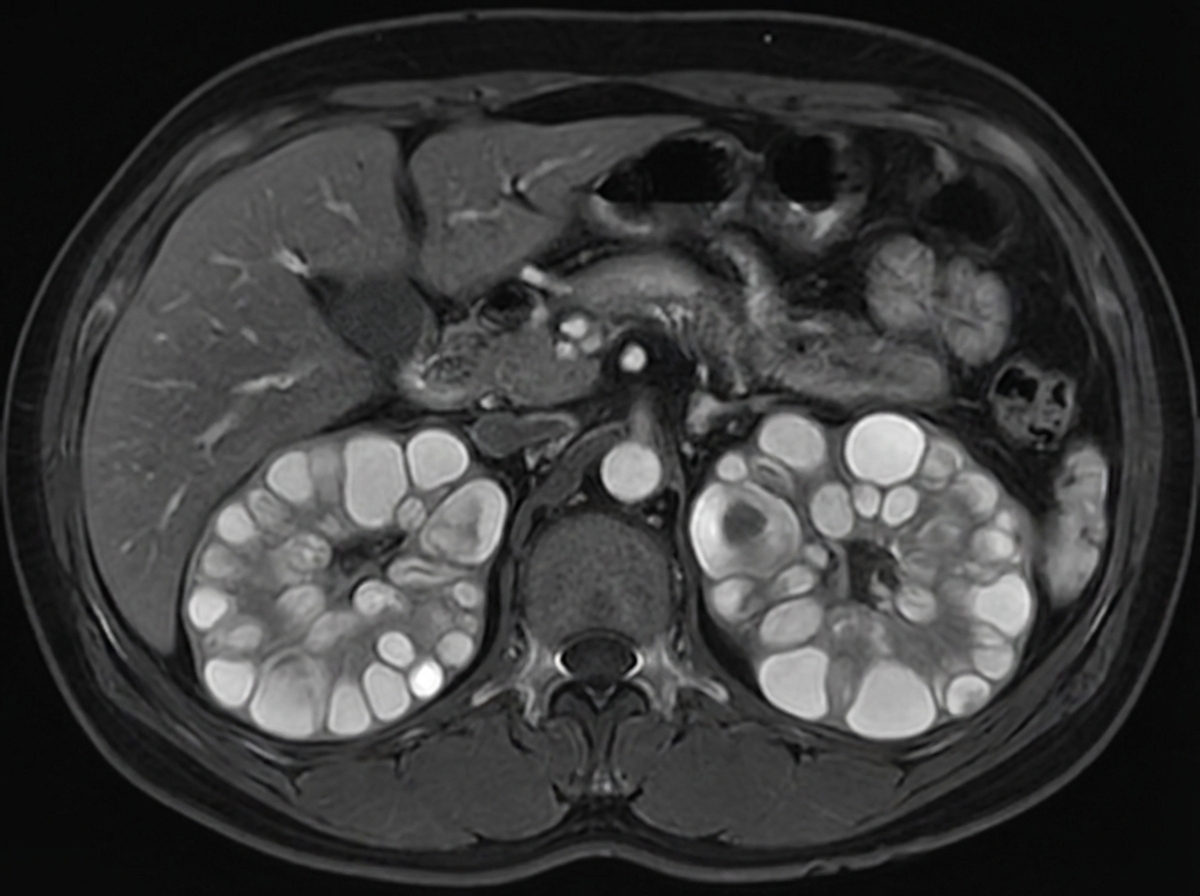
A 45-year-old patient presents with hypertension, hematuria, and flank pain. An MRI scan is performed, and the image provided shows multiple cystic lesions in both kidneys. What is the most likely diagnosis?
A 45-year-old farmer presents with right upper quadrant pain and a history of exposure to livestock. An abdominal ultrasound shows a cystic lesion in the liver with internal floating membranes, described as the "Water lily sign." Based on this finding, what is the most likely Gharbi classification stage of the hydatid cyst?

A 78-year-old immobile patient presents with a pressure ulcer on the sacral area, as shown in the image below. How would you grade this bedsore?