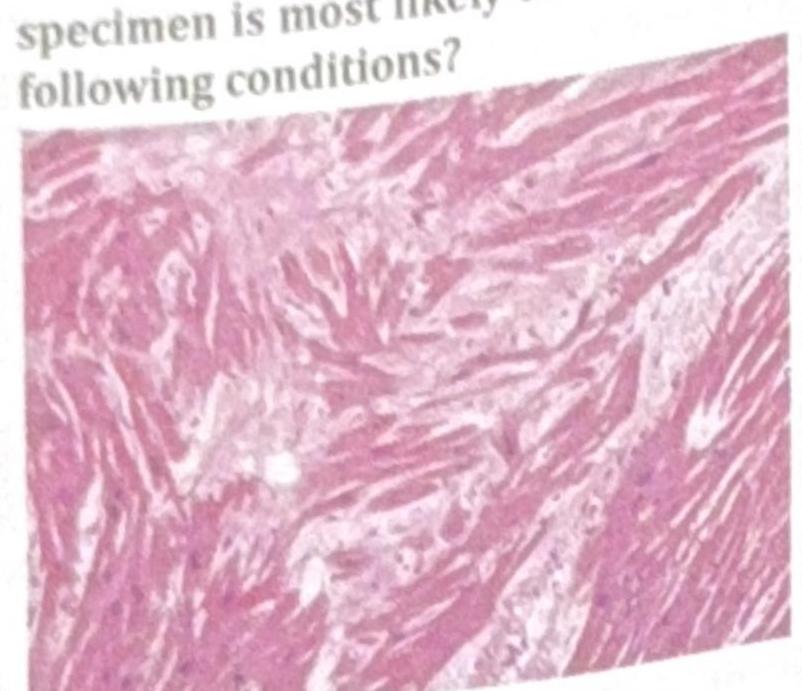
A young patient in an endemic area presents with pleural fluid showing LDH level greater than 0.6 times the serum LDH, protein level greater than 0.5 times the serum protein, and lymphocytic predominance. What is the most likely diagnosis?
A patient presents with acute epigastric pain and an increase in serum lipase. Several days after stabilization, a chest X-ray shows bilateral diffuse infiltrates. What is the most common pathology explaining the chest X-ray findings?
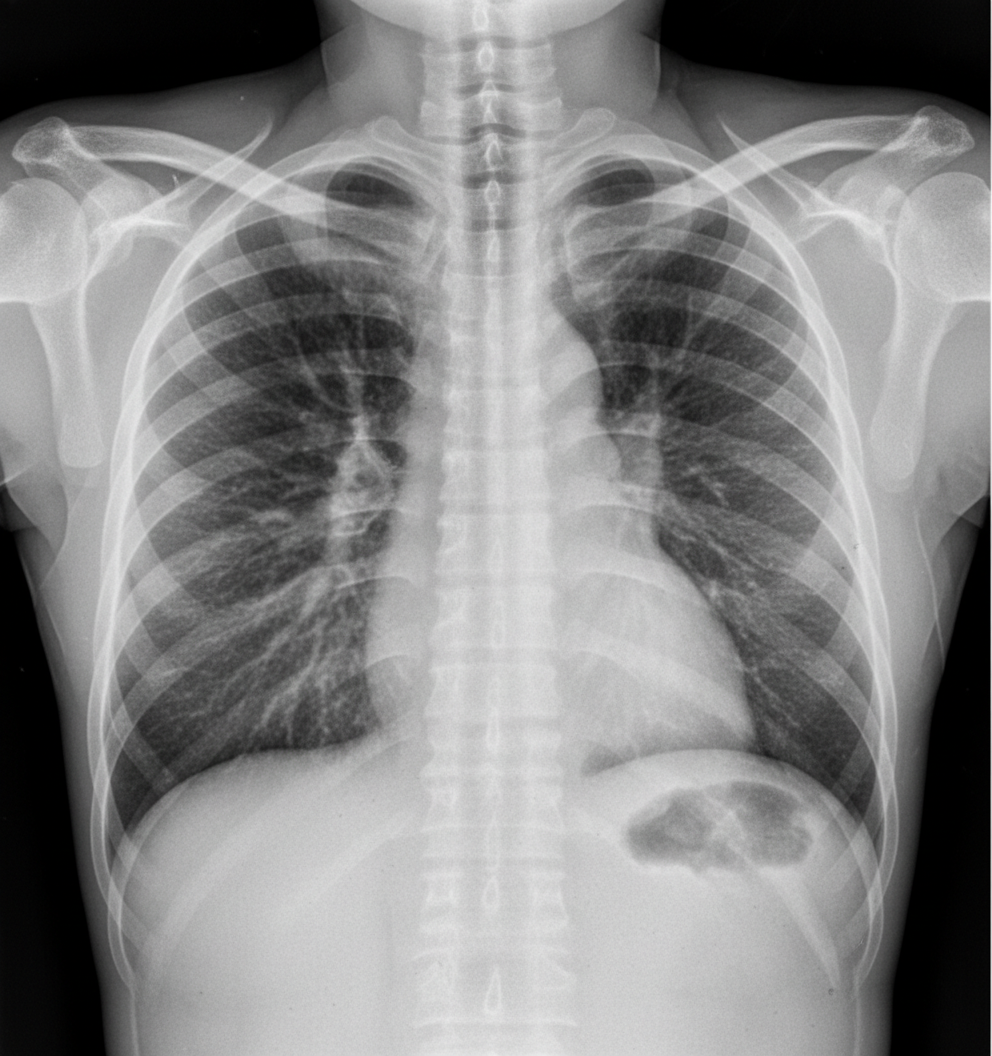
A 62-year-old patient presents with left-sided arm and leg weakness, right-sided facial paralysis with lateral rectus gaze palsy, and nystagmus. Based on the clinical presentation, which of the following syndromes is most consistent with these symptoms?
A patient with a history of hypertension presents with atrial fibrillation, shortness of breath, and bilateral basal crackles on auscultation. Which of the following would be the least important in the management of this patient?
The PR interval was measured at 0.21 seconds on a routine ECG of a patient. What is the correct interpretation?
In Type 1 Diabetes Mellitus (DM) stage 3 beta cell destruction, which of the following is the most likely presentation?
What is the most common cause of death in idiopathic pulmonary fibrosis (IPF)?