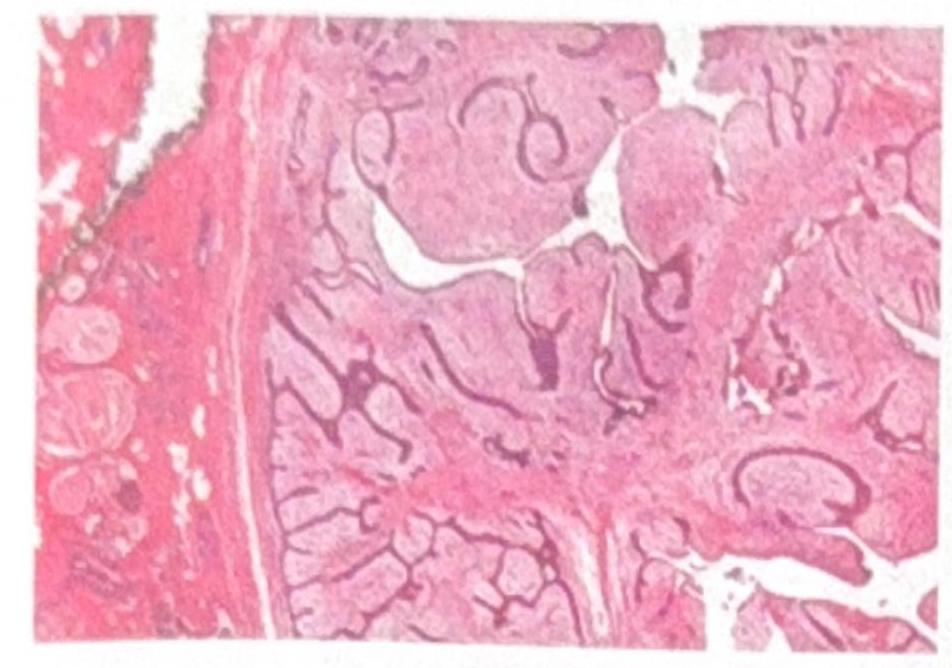
A slipped disc at the level shown in the image would most likely involve which nerve root?
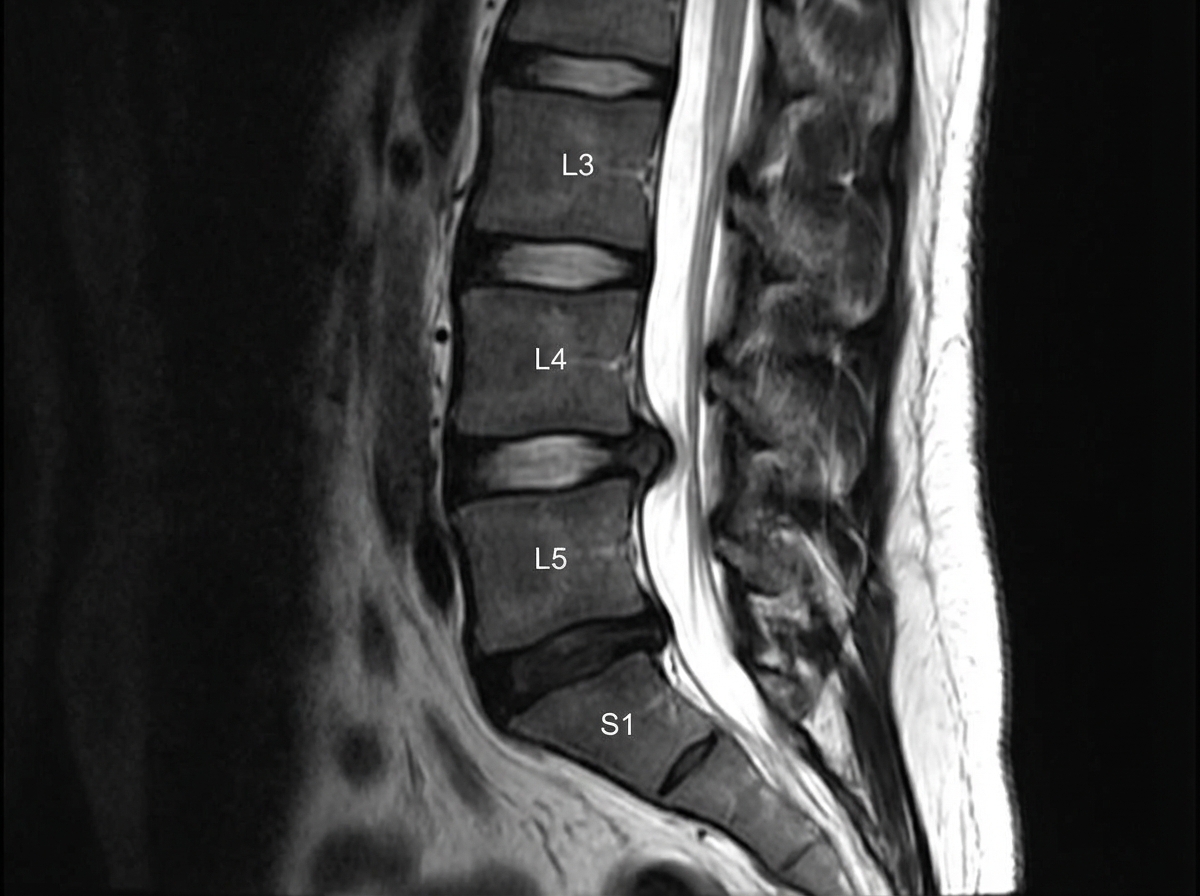
Identify the arrow marked nerve
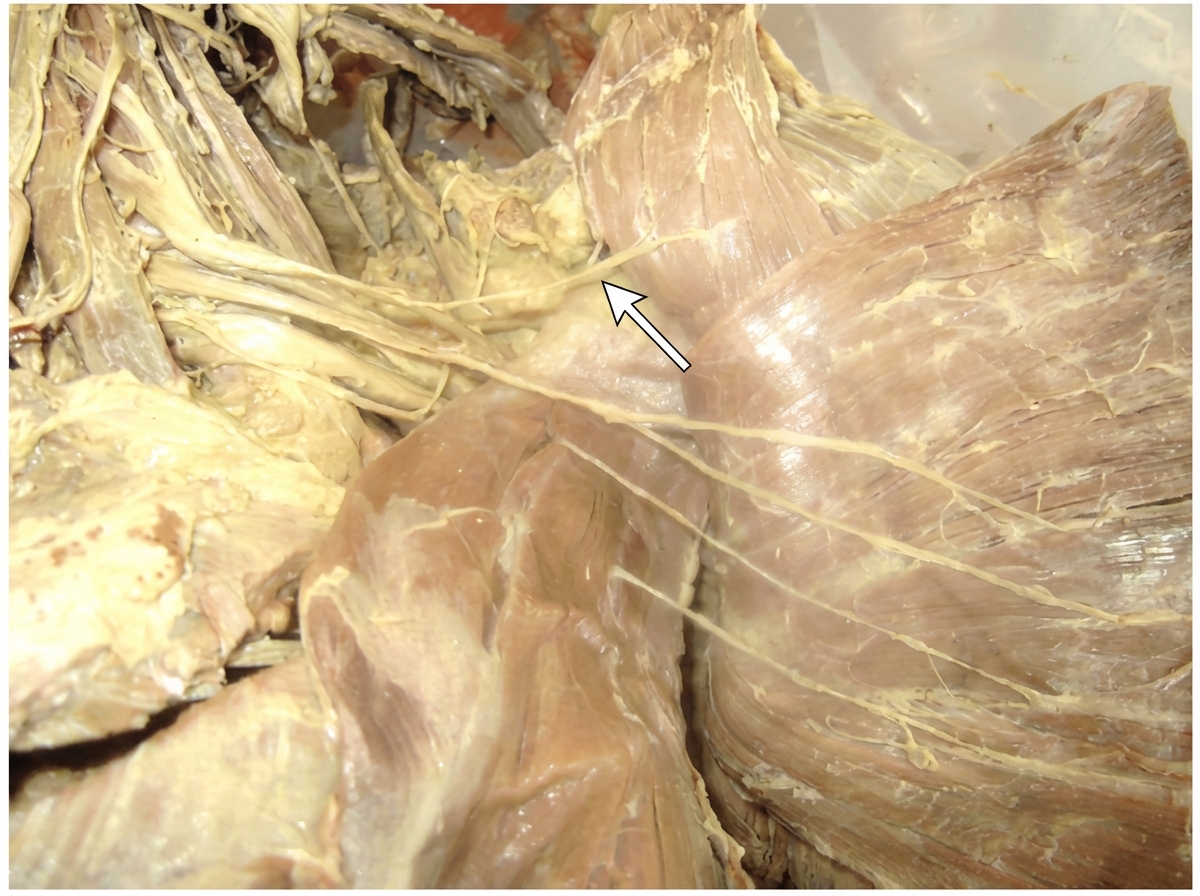
Identify the labeled structures correctly in the axial CT image of the thorax
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A slipped disc at the level shown in the image would most likely involve which nerve root?

Identify the arrow marked nerve

Identify the labeled structures correctly in the axial CT image of the thorax

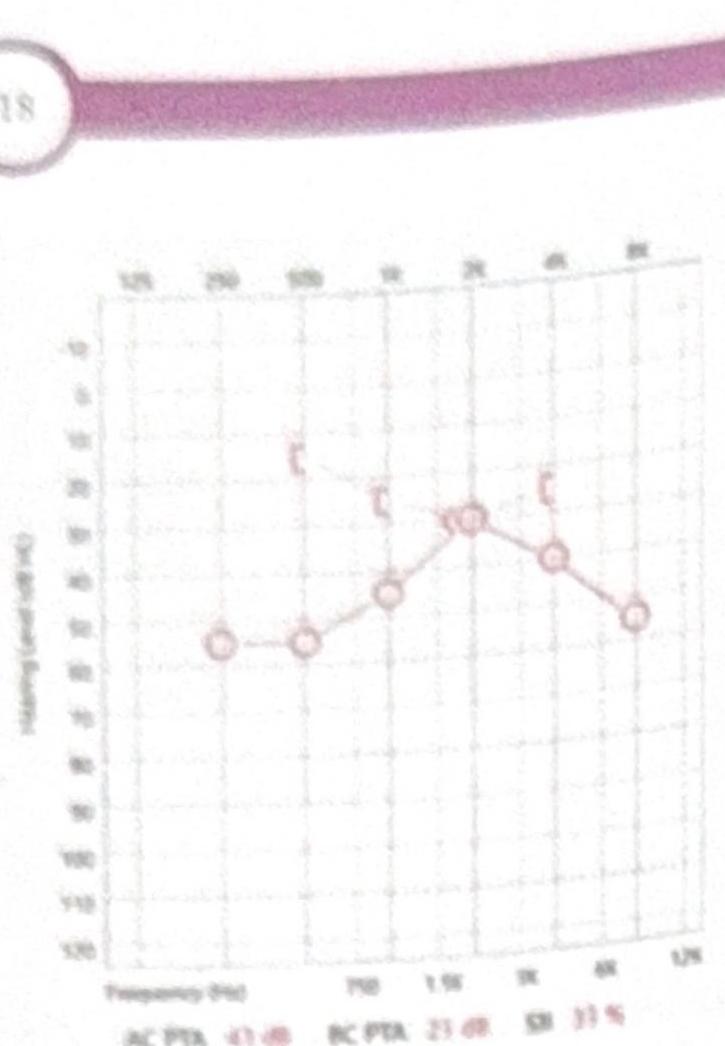
A female patient presents with mild conductive hearing loss (CHL) and tinnitus. Based on the pure tone audiometry (PTA) shown in the image, what is the most likely diagnosis?
A suspicious stain was treated with glacial acetic acid and heated. Examination shows the following crystalline finding. Which confirmatory test is being depicted?
Based on the image provided, identify the range of fire.
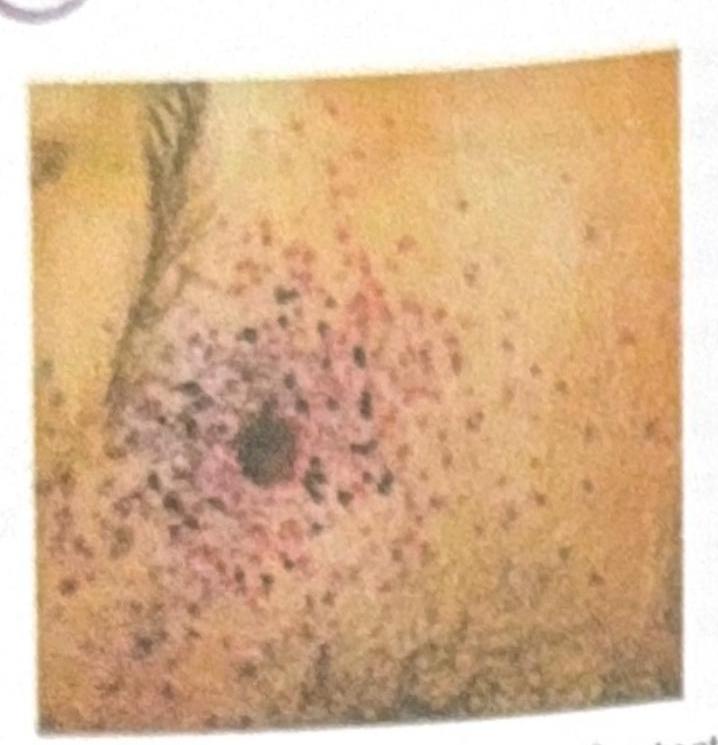
An adult man presents with the clinical condition shown in the image, and a Gram stain reveals Gram-negative diplococci. What is the most appropriate treatment?
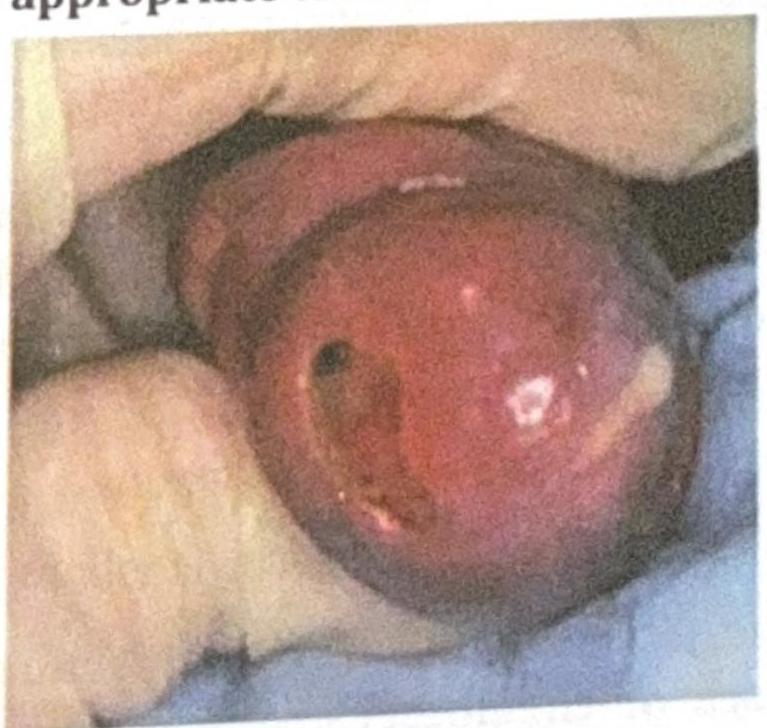
A female presents with dysuria and vaginal discharge. Wet mount examination shows pear-shaped organisms. What is the most likely diagnosis?
A G2P1L1 woman with a history of previous cesarean section presents with complications related to the placenta. The image below shows the gross appearance of the uterus. What is the most likely diagnosis?
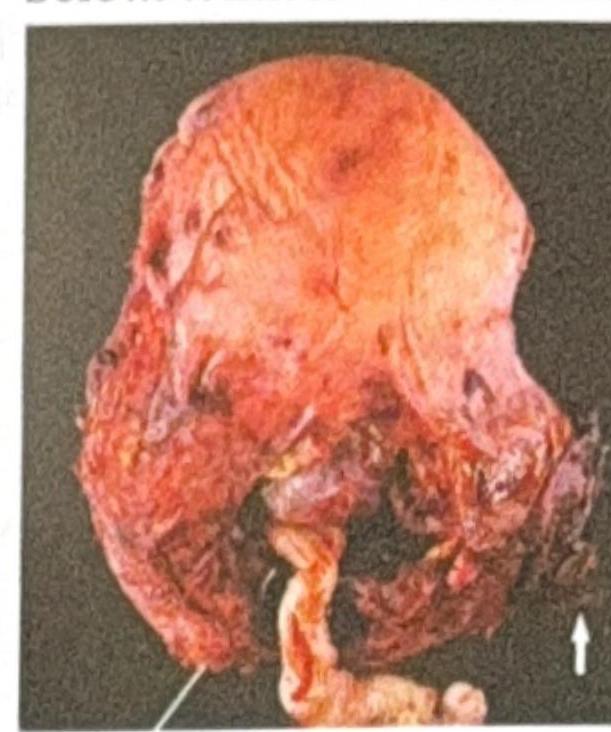
A 40-year-old female presents with an irregular 5 × 6 cm mass in the right breast. Histopathological examination reveals the image shown. What is the most likely diagnosis?