This instrument is used to measure which of the following?

Which of the following phases are directly involved in the recovery phase of the disaster cycle?
What does JSSK stand for?
Identify the logo?

The formula with the numerator as maternal deaths and the denominator as women of reproductive age is used to calculate which of the following?
Identify the index?
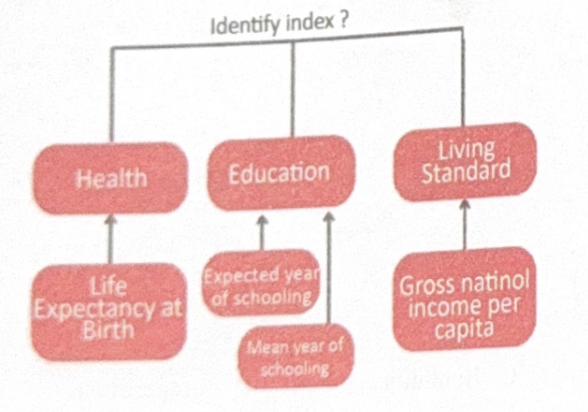
Which of the following is not a component of Physical Quality of Life Index (PQLI)?
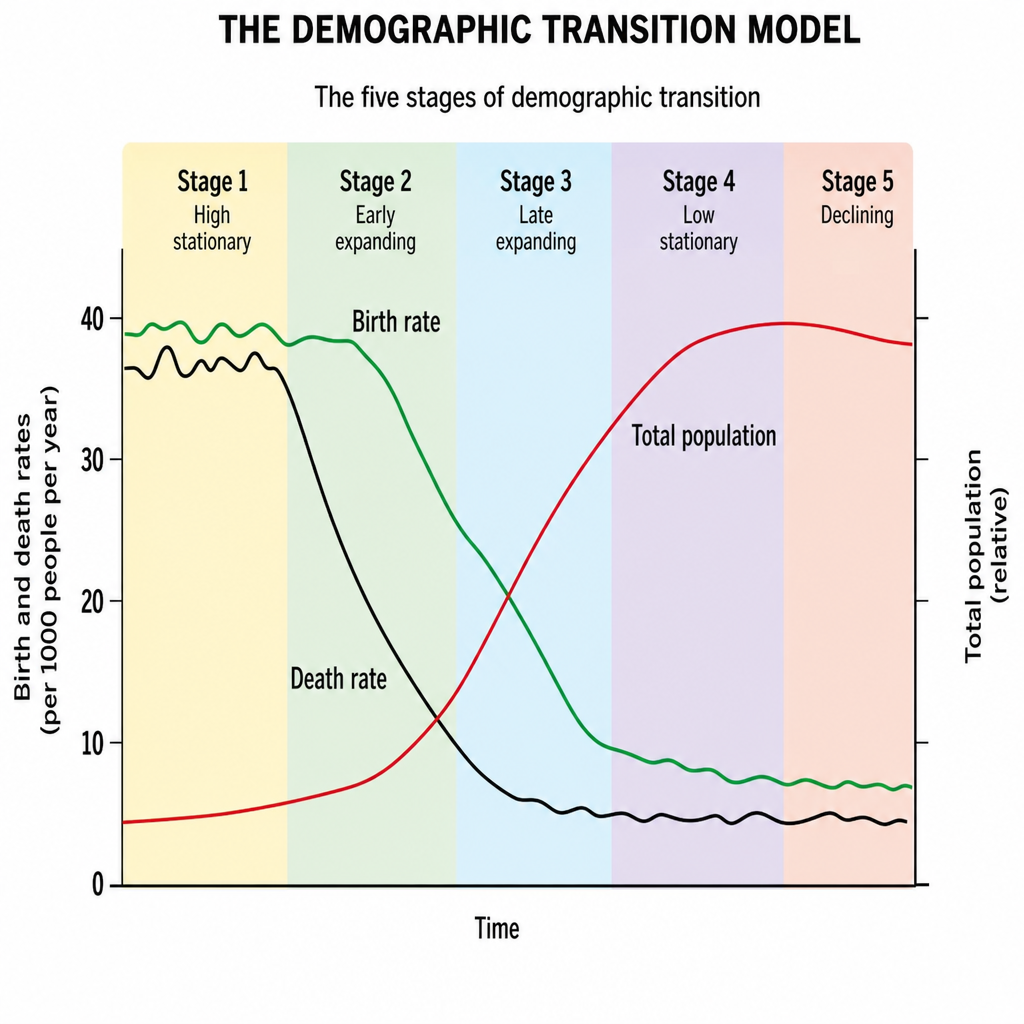
The Black Line in the demographic cycle represents: