Match the following ECG findings (1-4) with their corresponding arrhythmias (A-D): 1. Sawtooth pattern in leads II, III, aVF with regular ventricular response 2. Irregularly irregular rhythm with absent P waves 3. Narrow QRS tachycardia with abrupt onset/termination 4. Wide QRS tachycardia with AV dissociation A. Atrial fibrillation B. PSVT (Paroxysmal Supraventricular Tachycardia) C. Atrial flutter D. Ventricular tachycardia What is the correct matching?
A patient presents with shortness of breath. Vitals are HR = 120/min with BP = 90/60 mm Hg. Echocardiography shows diastolic collapse of the ventricles. What is the best management for this patient?
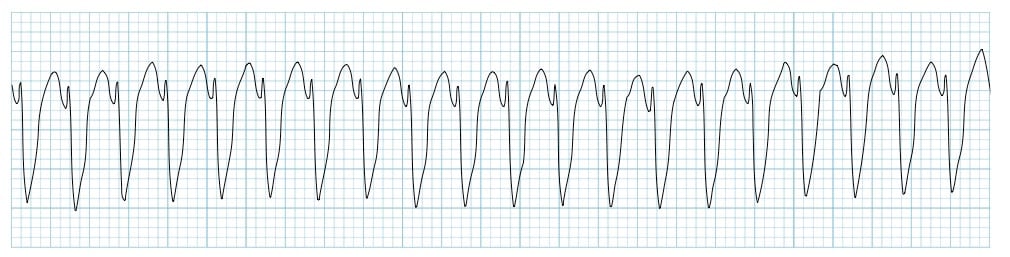
A patient is pulseless with the following rhythm shown in the ECG. What is the next best step in management?
A hypertensive patient presents with an irregularly irregular pulse and a loud P2 on auscultation. Which JVP finding is likely to be seen in this patient?
A 60-year-old lady presents with shortness of breath (SOB) and episodes of angina pectoris. Work-up reveals aortic stenosis. Which of the following is the most likely reason behind these chest pain episodes?
A 15-year-old patient presents with joint swelling, a pan-systolic murmur, negative rheumatoid factor (RF), and elevated ESR. The patient also reports a recent history of sore throat and exhibits subcutaneous nodules and erythema marginatum on physical examination. What is the most likely diagnosis?
A patient presents with wheezing that improves with as-needed use of albuterol. Spirometry shows FEV1 ranging from 70 % to 83 %, and the patient experiences nighttime chest tightening twice a week. What is the most appropriate treatment?
A farmer presents with severe leg pain, fever, chills, retro-orbital pain, and bilateral conjunctival suffusion. What is the most likely diagnosis?
A patient presents with hypotension, hyponatremia, and blackening of the palmar creases. Which of the following conditions is most likely associated with these symptoms?