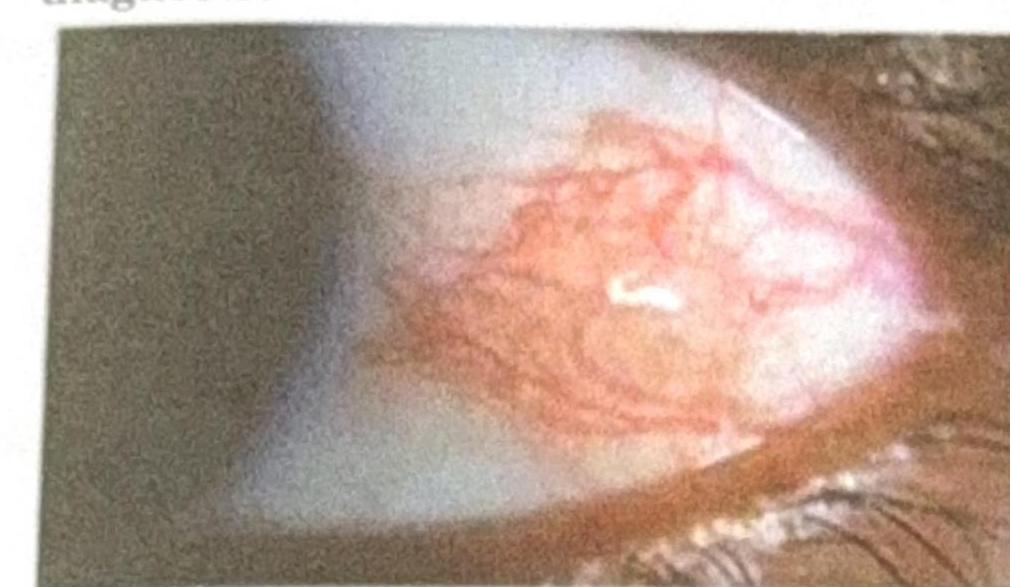
A patient presents with eye ache and difficulty in vision after watching a movie. What will be the first line of management?
A patient presents with sudden painful diminution of vision, difficulty looking in light (photophobia), and circumcorneal congestion with hypopyon. What is the most likely diagnosis?
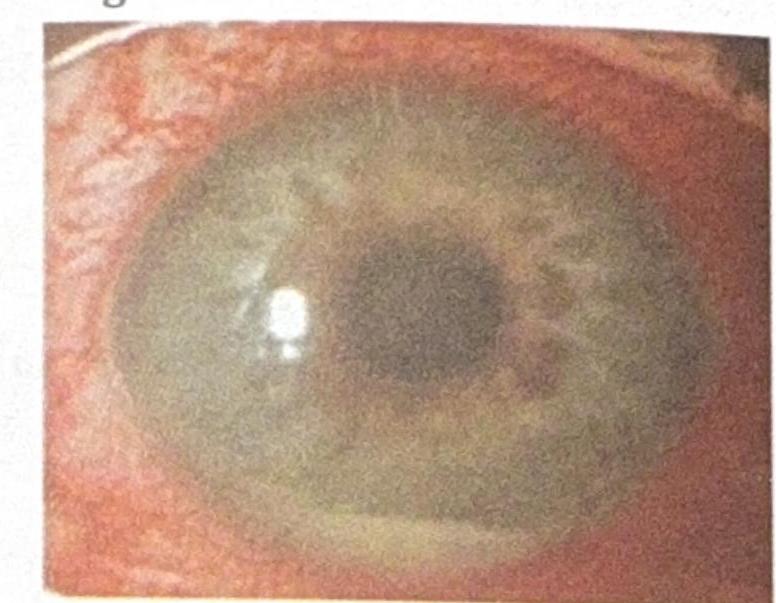
A patient presents with a nodular swelling near the limbus, which does not blanch with topical vasoconstrictors and recurs after treatment. Based on the image and clinical presentation, what is the most probable diagnosis?