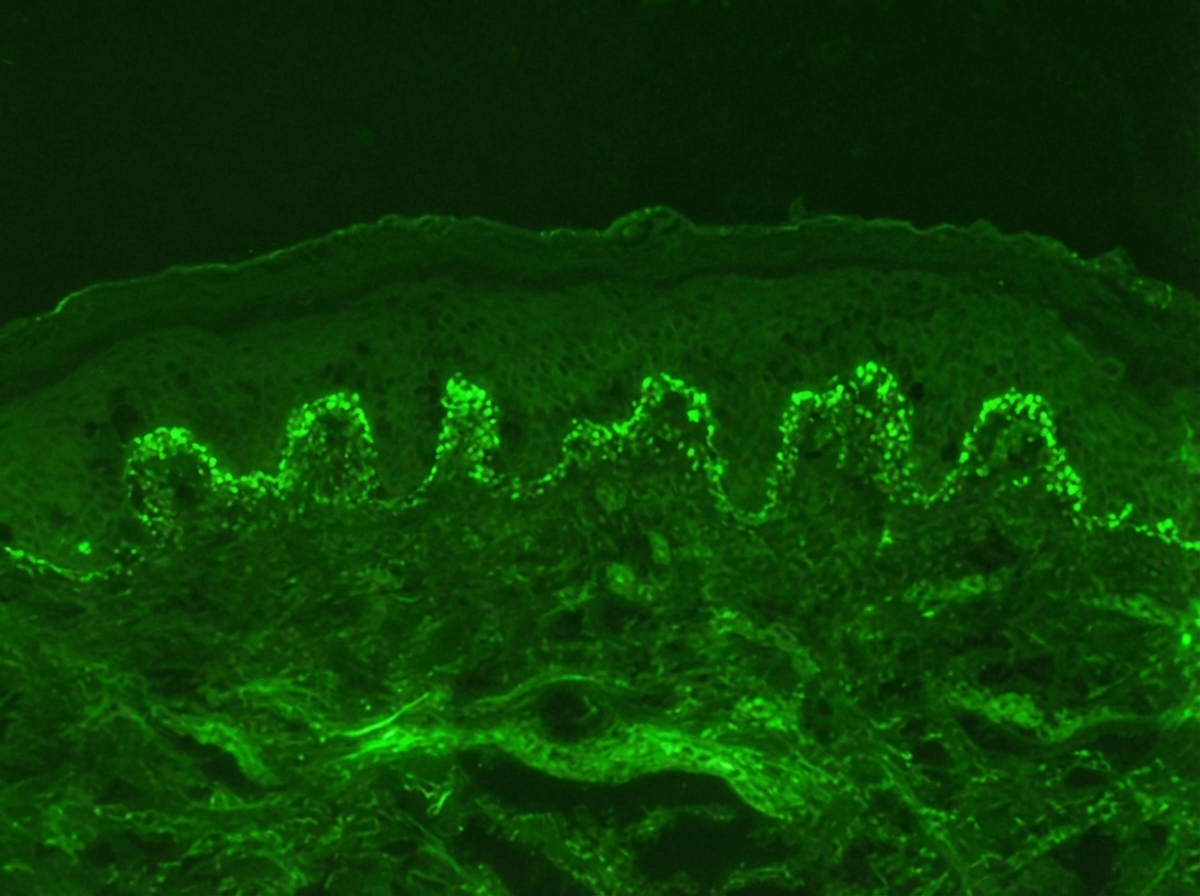
Identify the diagnosis based on the dermatology immunofluorescence (IF) image provided.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
An adult tall male presents with a long arm span, pectus excavatum, and cardiac abnormalities. What is the most likely defective protein?
Identify the diagnosis based on the dermatology immunofluorescence (IF) image provided.

Which of the following statements is correct about Paroxysmal Nocturnal Hemoglobinuria (PNH)?
A patient presents with pulmonary hemorrhage and is P-ANCA positive. What is the most likely diagnosis?
Which of the following is typically observed in the investigation results for a patient with iron deficiency anemia (IDA)?
An adult female presents with pallor and fatigue. Blood investigations show low hemoglobin ( Hb ), low serum iron, low ferritin, low transferrin saturation, and increased total iron-binding capacity (TIBC). What is the likely diagnosis?
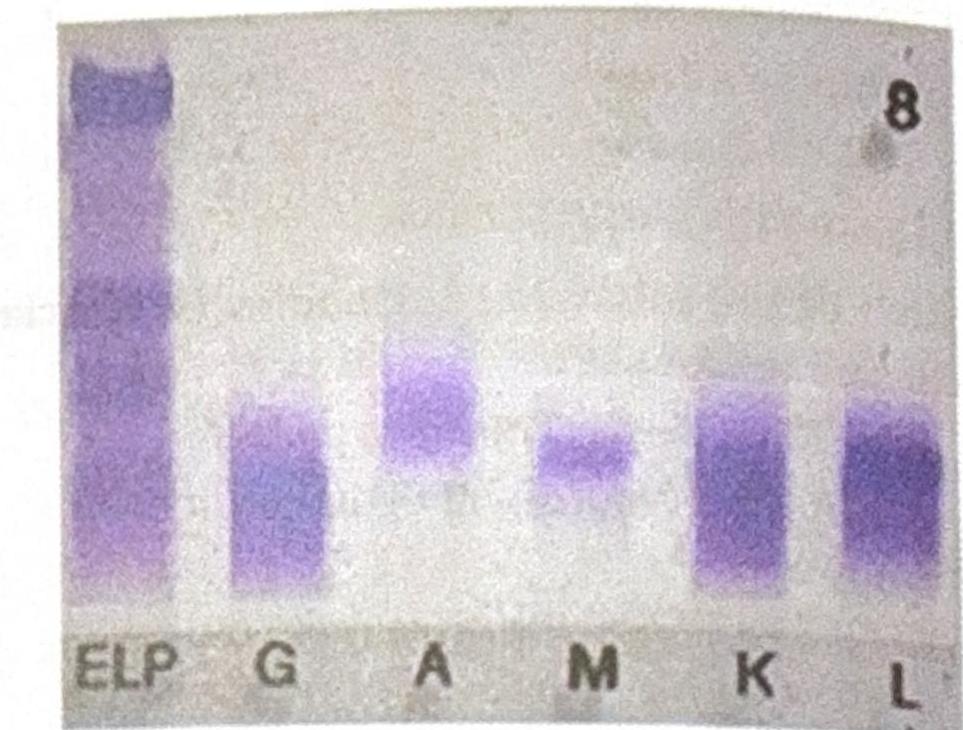
An elderly male patient presented with clinical symptoms and signs consistent with possible multiple myeloma. Electrophoresis shows an M spike, and immunofixation findings are shown below. Which of the following statements best corresponds to the findings?
Which of the following is an intracellular marker or deposition found in Alzheimer's disease?
A child presents with recurrent infections. Mediastinal imaging reveals an absent thymus gland, and further investigations show low ADA (adenosine deaminase) levels. What is the most likely diagnosis?
Which of the following is not seen with ileal resections?