What is the purpose of Positive End-Expiratory Pressure (PEEP)?
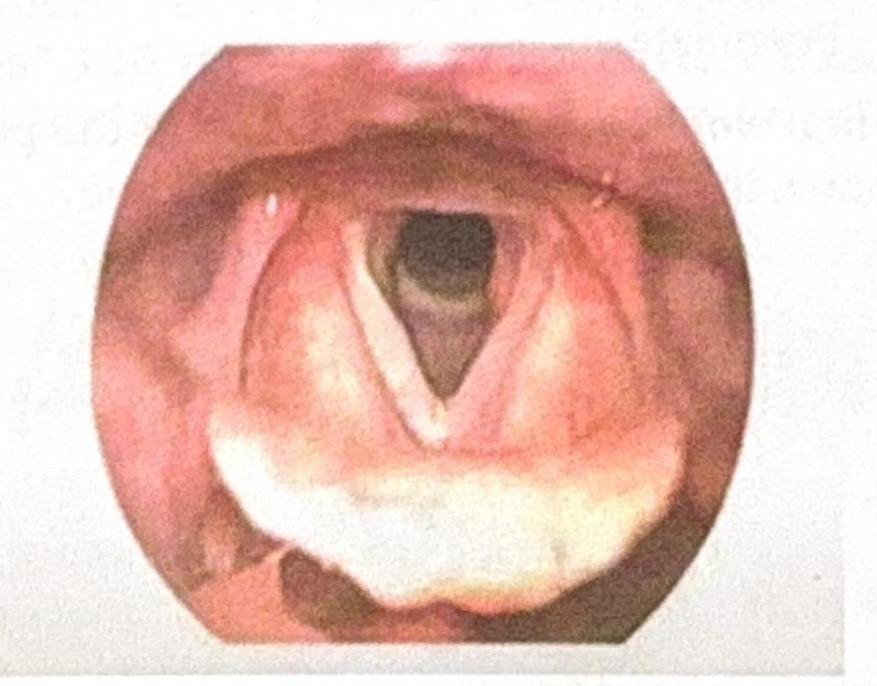
What is the staging system used for the condition seen in the patient after a history of intubation, as shown in the image?
What is the name of the nerve block technique shown in the image?
A patient presented with rigidity, tremors, and trismus after being administered an anesthetic agent. Which anesthetic agent is most likely to have been administered?
In which clinical scenario would you find a patient requiring the vital signs assessment technique shown in the image?