Which of the following cardioselective betablockers has been shown to decrease mortality in patients with congestive heart failure?
Aprepitant is a drug used in the treatment of some cases of chemotherapy-induced nausea and vomiting. What is the mechanism of action of this drug?
Which of the following is an inclusion criterion for the shorter bedaquiline regimen in the treatment of tuberculosis?
A patient presents with hypertension and has a history of renal stones, along with several episodes of renal colic. Which diuretic is the most appropriate to use?
Which of the following is the most appropriate treatment for an overactive bladder in a patient with dementia?
Which of the following statements regarding the patch shown in the figure is correct?
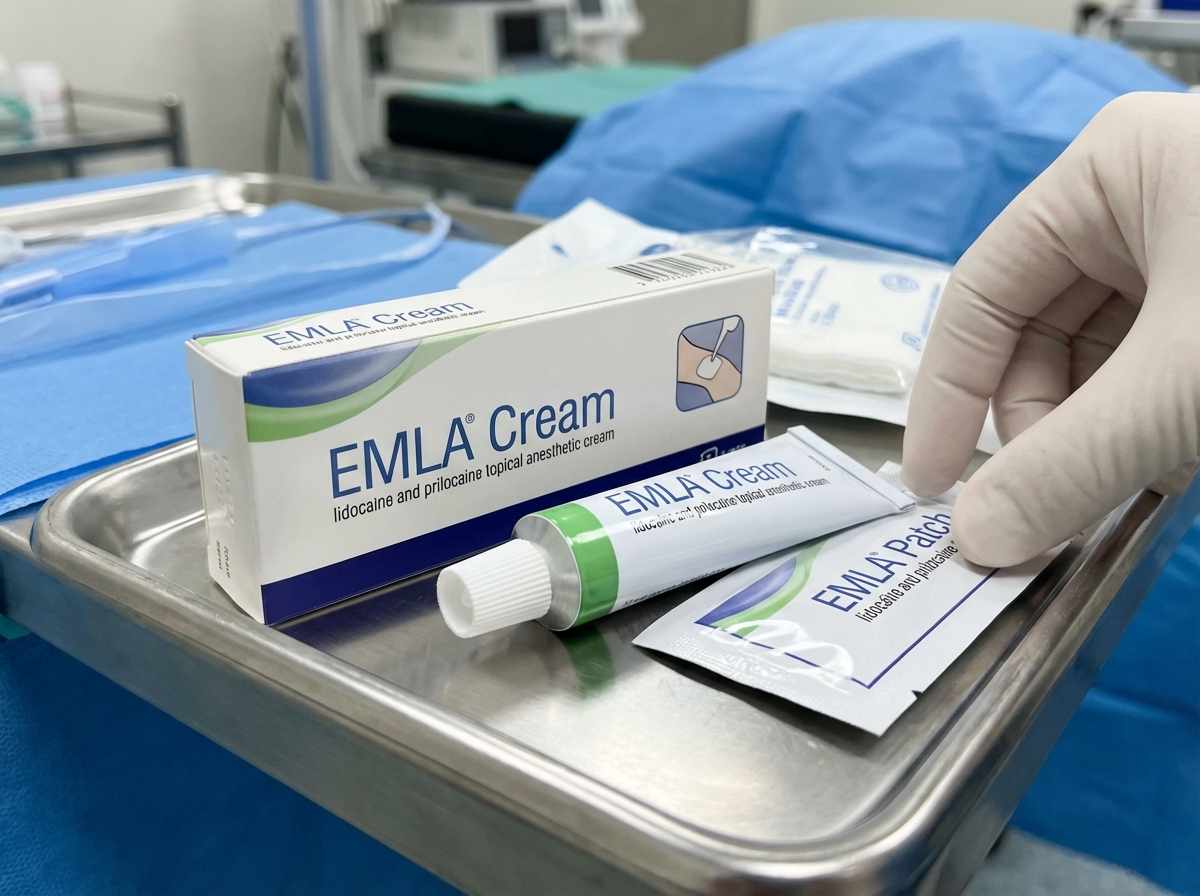
Lidocaine is used in a loading dose for the treatment of arrhythmias. The loading dose of this drug depends upon which of the following factors?