A patient with a nerve injury was asked to form an "O" with their index finger and thumb but was unable to do so. Which muscle is most likely affected?
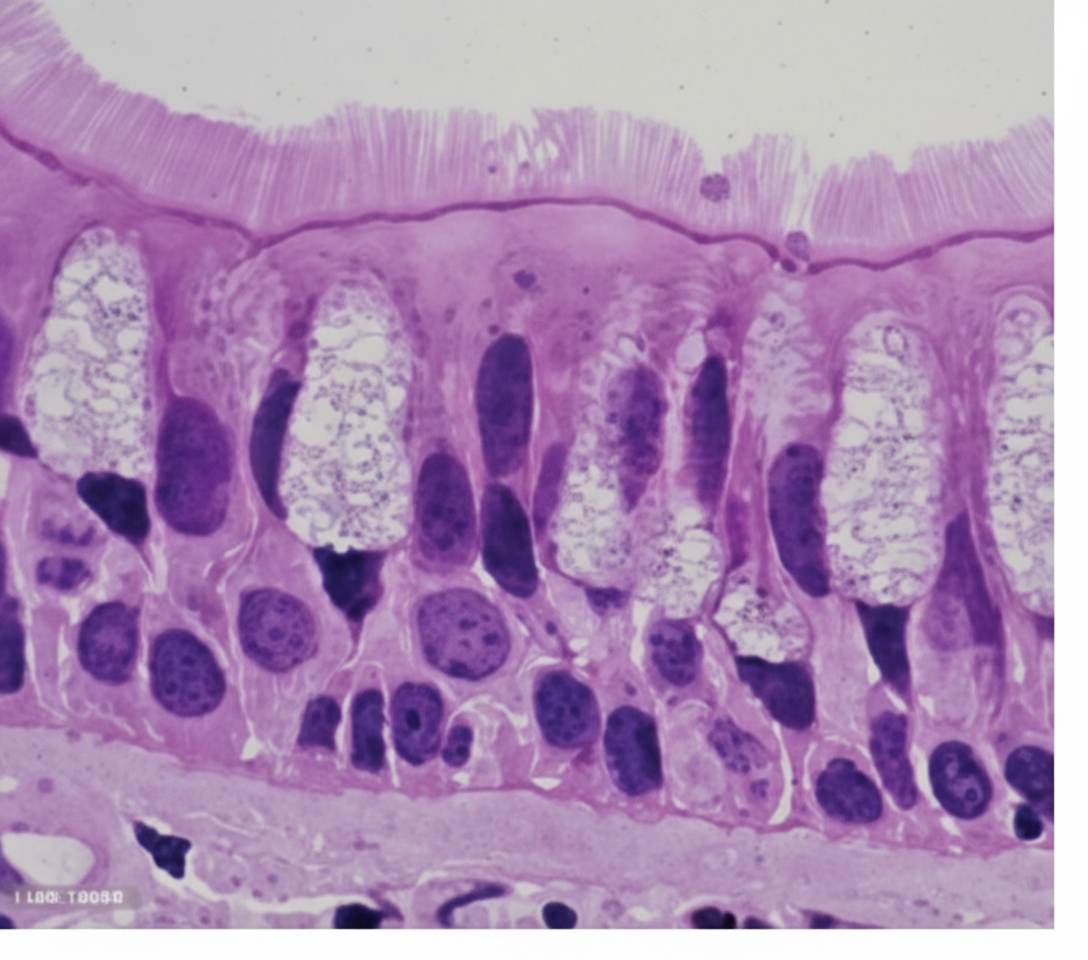
This type of epithelium is most commonly seen in which of the following organs?
Which tongue papillae do not have taste buds?