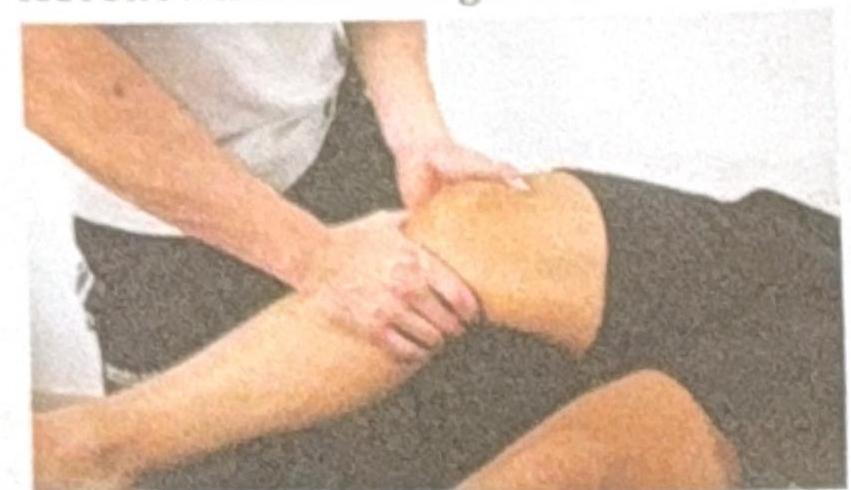
A football player experienced a twist in the ankle and knee. Clinically, no bone injury was appreciated. The examiner is performing the test shown in the image. Which test is this?
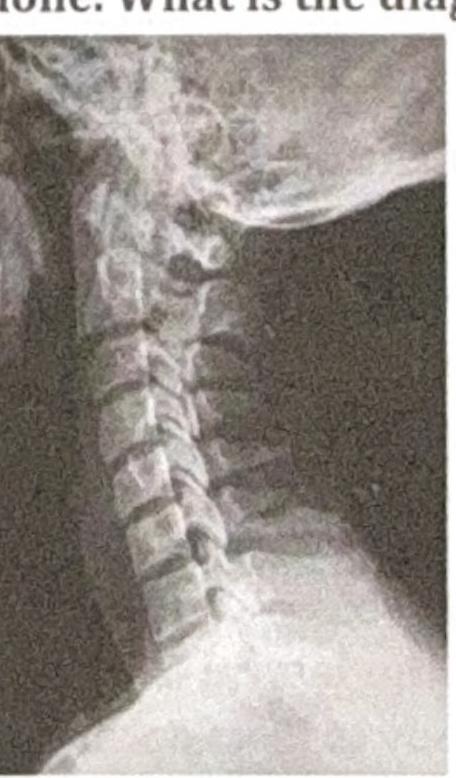
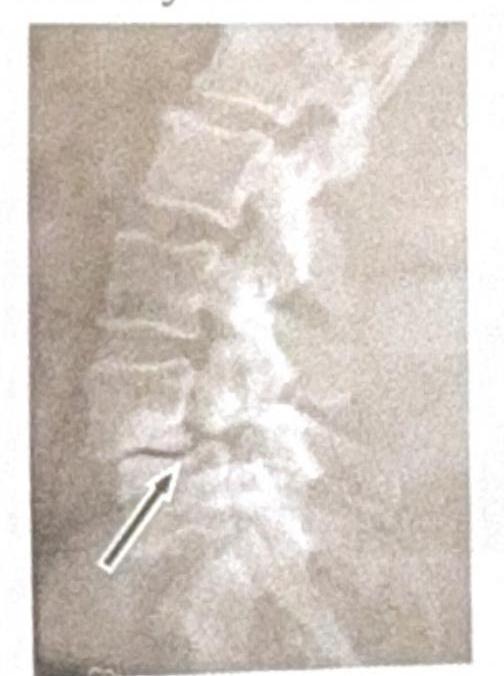
Identify the condition shown in the given X-ray:
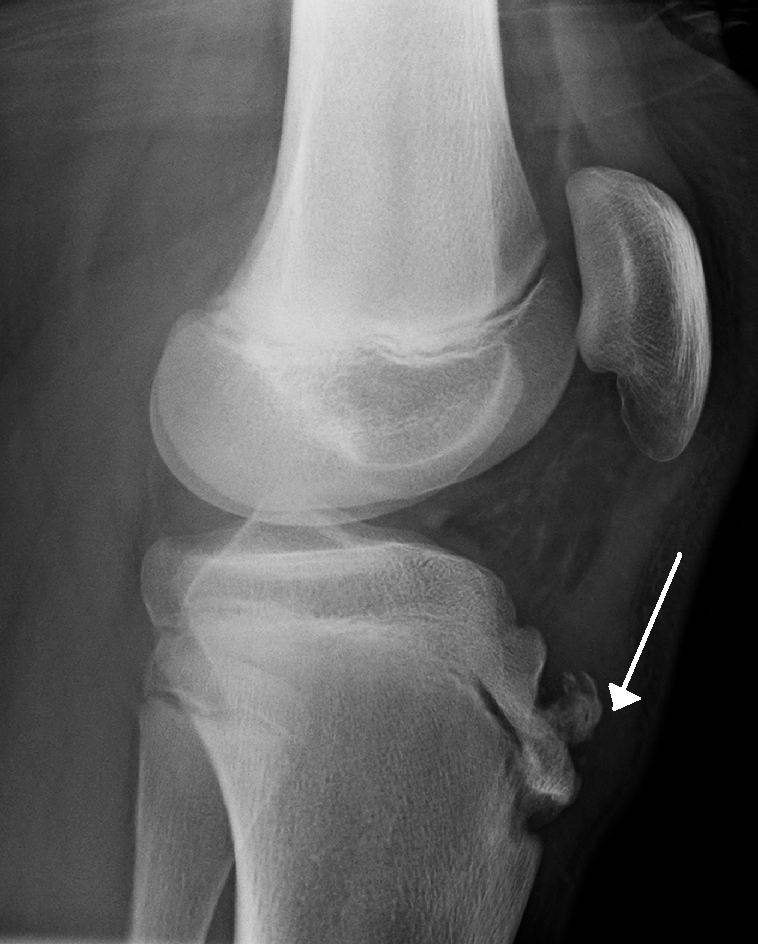
The X-ray shows plating done for a fracture. How does this fracture heal?
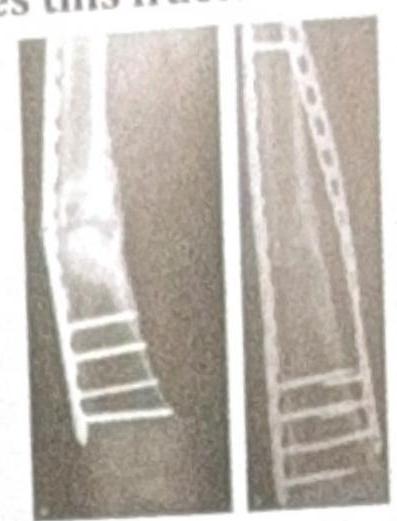
Identify the condition shown in the image:
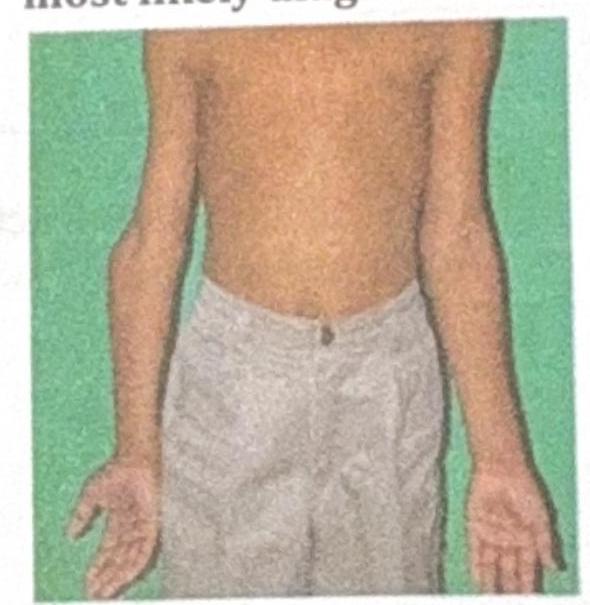
A 10-year-old boy presents with the physical findings shown in the image, characterized by inward angulation of the elbows. What is the most likely diagnosis?