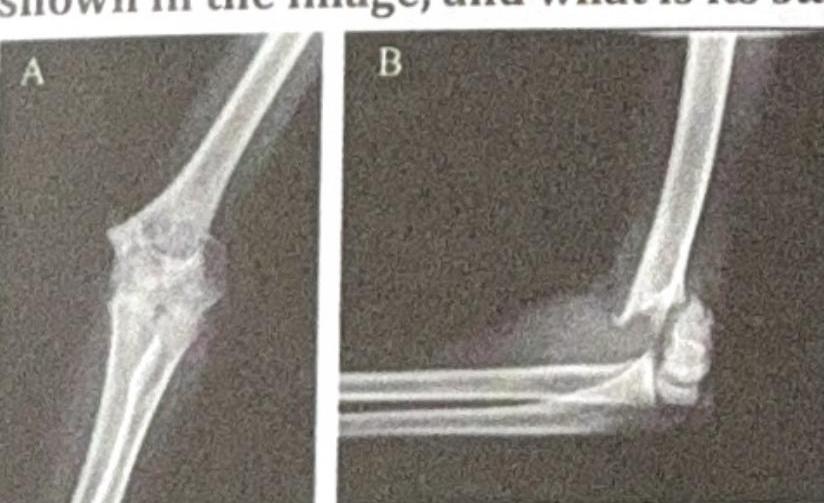
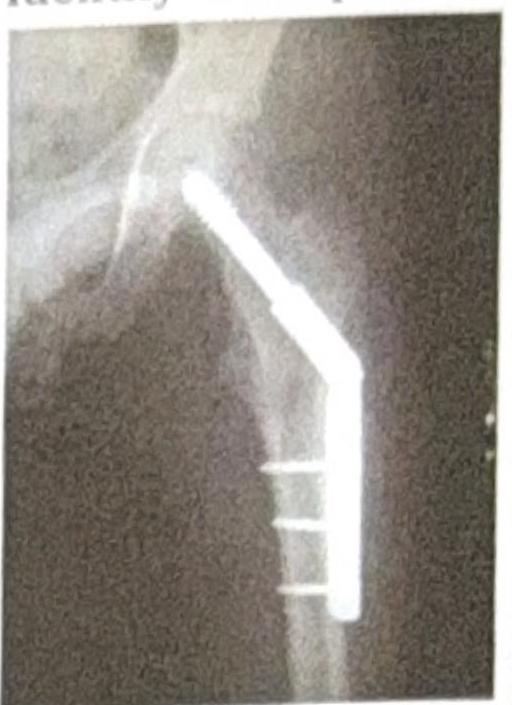
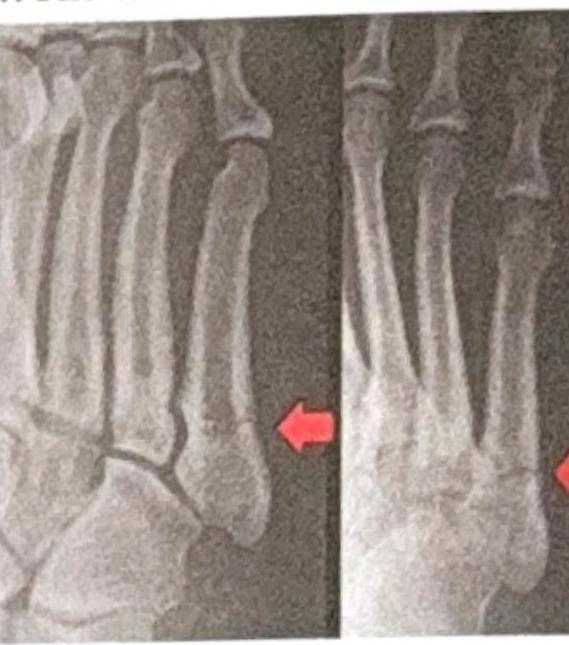
A GSP4 woman comes for routine sonography for the first time. She has four daughters and expresses a desire for a boy this time, asking for sex determination. To abide by ethical guidelines, what should you do?
A young woman presents with prolapse, and a mesh is being placed. Where is this mesh typically fixed to?
Which of the following is a tumor marker associated with ovarian solid-cystic masses?
A 32-year-old woman presents with a new 2 cm black nodular mass near her episiotomy scar. She reports that the mass is painful and tends to increase in size during menstruation. What is the most likely diagnosis?
A teenage girl presents with a history of amenorrhea. Local examination is shown in the image. What karyotype analysis would you consider for further evaluation?
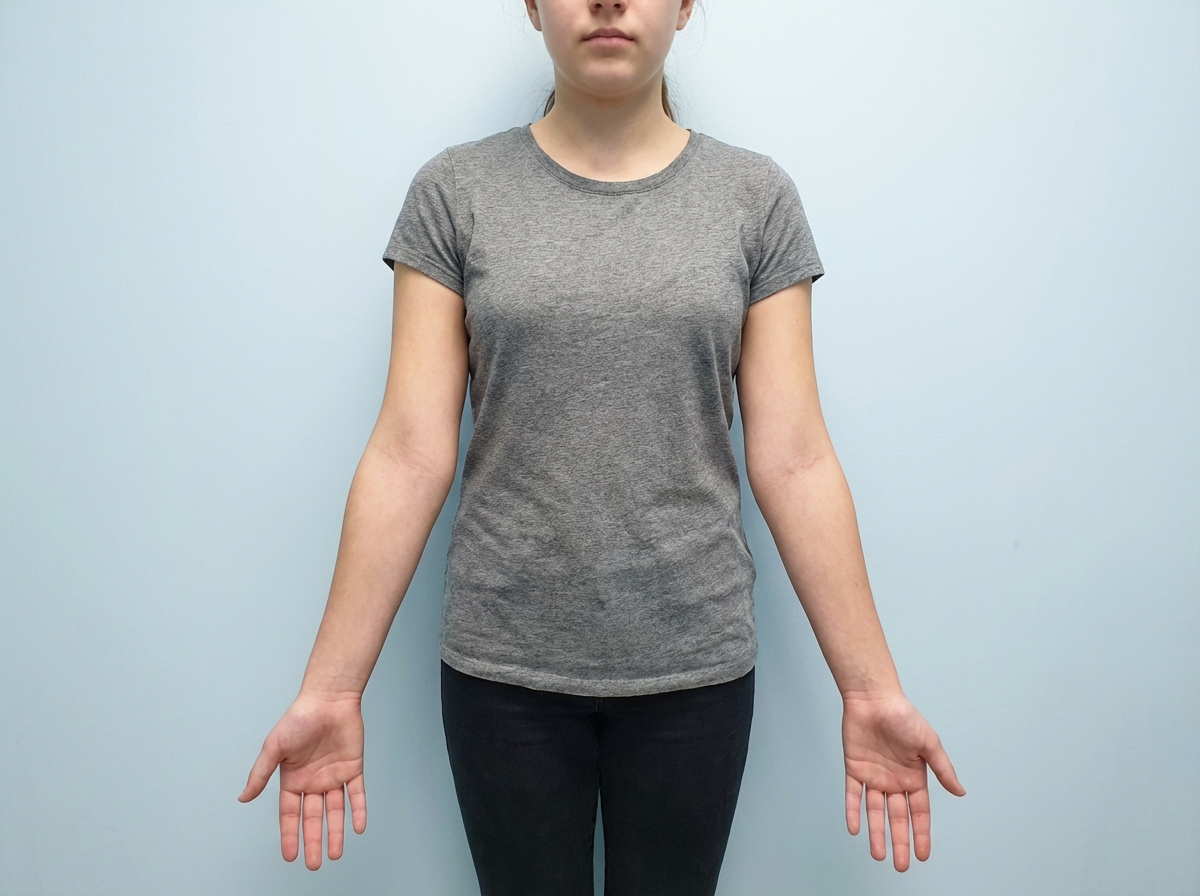
A female presents with postcoital bleeding. Which of the following is the most appropriate investigation?