NEET-PG 2024 — Ophthalmology
9 Previous Year Questions with Answers & Explanations
Identify the visual field defect shown in the image.

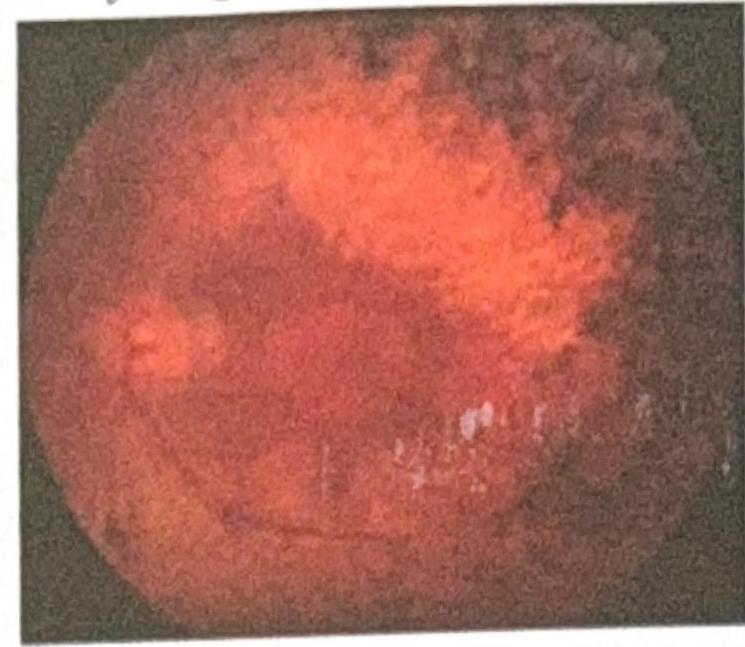
A patient presented with gradual loss in night vision and peripheral vision. Based on the fundoscopic image provided, what is the most likely diagnosis?
What is the diagnosis if a patient can only see 3 green dots on the Worth 4 Dot test?
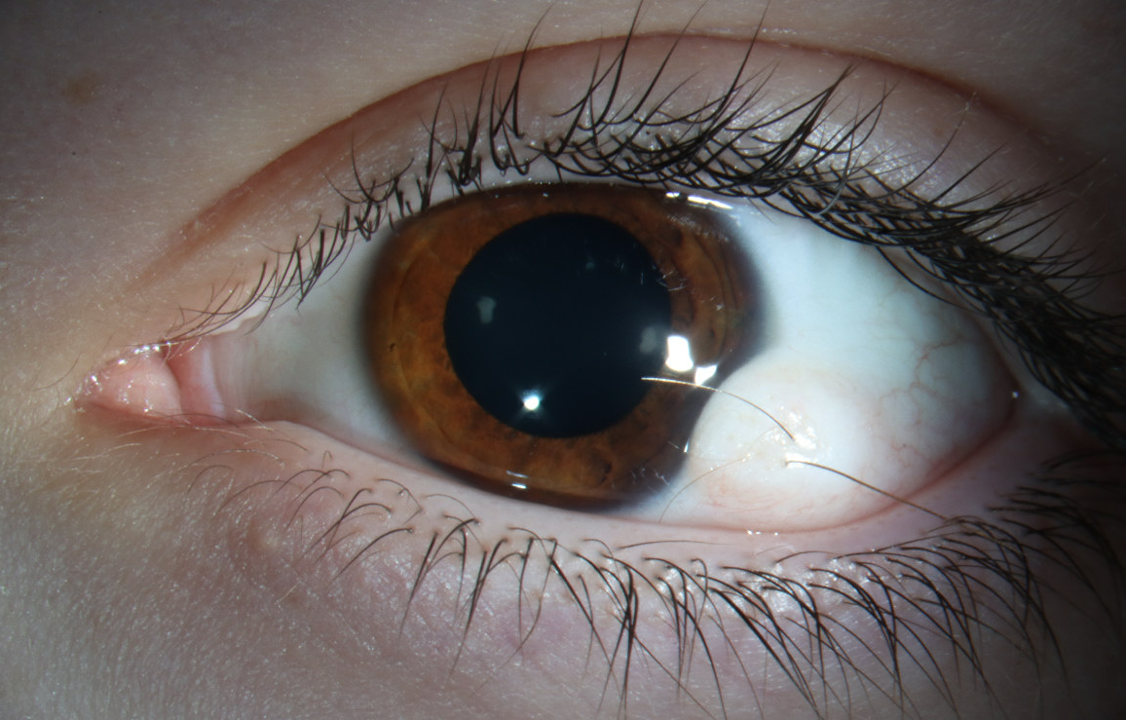
A patient presents to the OPD with the finding shown in the image. What is the most likely diagnosis?
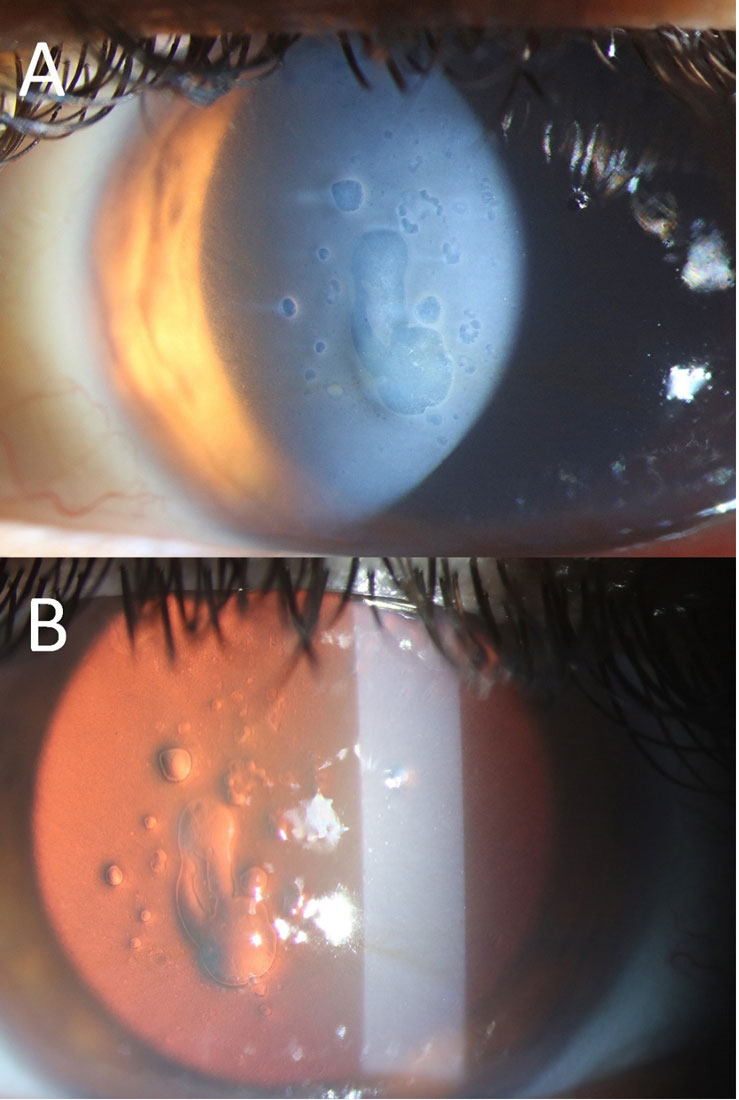
A patient, three years post-surgery, presents with the condition shown in the image and complains of decreased vision. What is the most likely diagnosis?
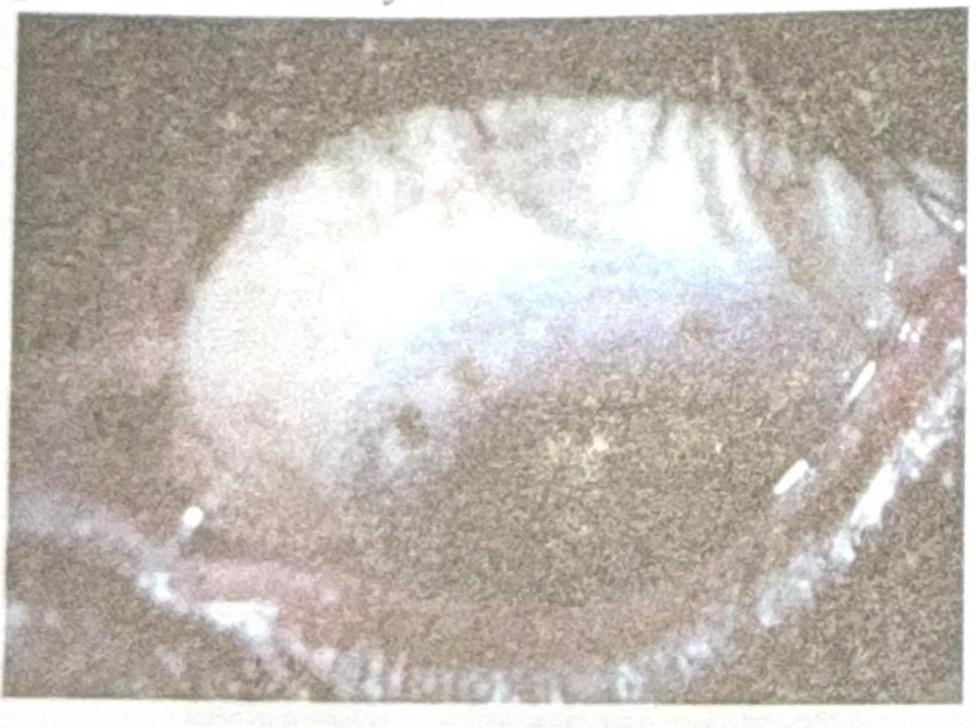
Identify the diagnosis based on the clinical image shown.
A patient presents with eye ache and difficulty in vision after watching a movie. What will be the first line of management?
A patient presents with sudden painful diminution of vision, difficulty looking in light (photophobia), and circumcorneal congestion with hypopyon. What is the most likely diagnosis?
A patient presents with a nodular swelling near the limbus, which does not blanch with topical vasoconstrictors and recurs after treatment. Based on the image and clinical presentation, what is the most probable diagnosis?
NEET-PG 2024 - Ophthalmology NEET-PG Practice Questions and MCQs
Question 1: Identify the visual field defect shown in the image.
- A. Binasal hemianopia
- B. Bitemporal hemianopia (Correct Answer)
- C. Homonymous hemianopia
- D. Altitudinal defect
Explanation: ***Bitemporal hemianopia*** - The image shows loss of vision in the **temporal (outer) halves of both visual fields**, which is characteristic of bitemporal hemianopia. - This defect typically results from a lesion at the **optic chiasm**, compressing the crossing nasal retinal fibers, often due to a **pituitary tumor**. *Binasal hemianopia* - This condition involves visual loss in the **nasal (inner) halves of both visual fields**, which is the opposite of what is depicted. - It is a rare defect that can be caused by lesions affecting the **uncrossed temporal retinal fibers** on both sides, such as from bilateral carotid artery aneurysms. *Homonymous hemianopia* - A homonymous hemianopia involves the **same half of the visual field in both eyes** (e.g., right visual field loss in both eyes), resulting from a lesion posterior to the optic chiasm. - The image clearly shows different halves affected in each eye (temporal fields), not the same half. *Altitudinal defect* - An altitudinal defect involves the **loss of vision in the upper or lower half of the visual field** in one or both eyes, respecting the horizontal midline. - The visual field loss shown in the image is vertical, affecting the temporal halves, not the upper or lower halves.
Question 2: A patient presented with gradual loss in night vision and peripheral vision. Based on the fundoscopic image provided, what is the most likely diagnosis?
- A. Retinitis pigmentosa (Correct Answer)
- B. Retinal hemorrhage
- C. Fundus albipunctatus
- D. Fundus flavimaculatus
Explanation: ***Retinitis pigmentosa*** - The fundoscopic image exhibits **bone spicule-like pigment deposits** in the periphery, **attenuation of retinal vessels**, and a **waxy pallor of the optic disc**, which are characteristic signs of retinitis pigmentosa. The clinical presentation of gradual loss in **night vision (nyctalopia)** and **peripheral vision** (tunnel vision) is classic for this inherited retinal dystrophy, as it primarily affects the **rod photoreceptors** first. *Retinal hemorrhage* - Retinal hemorrhages appear as **red blotches or streaks** on the fundus and are usually associated with conditions like **hypertension**, **diabetes**, or **retinal vein occlusion**. This image does not show acute red hemorrhages, but rather **dark, aggregated pigment**, and the symptoms do not align with sudden vision changes often seen in acute hemorrhages. *Fundus albipunctatus* - This condition is characterized by numerous **small, discrete, white or yellowish dots** scattered throughout the retina, usually sparing the macula. While it can cause night blindness, the fundoscopic image here shows **bone spicule pigmentation** and **vascular attenuation**, not the widespread white dots typical of fundus albipunctatus. *Fundus flavimaculatus* - This refers to Stargardt disease or fundus flavimaculatus, which presents with **yellowish flecks** (pisiform or fish-tail shaped) scattered in the posterior pole and mid-periphery, along with **macular degeneration**. The image does not show these distinct yellow flecks or evident macular changes, and the pigmentary changes are more consistent with retinitis pigmentosa.
Question 3: What is the diagnosis if a patient can only see 3 green dots on the Worth 4 Dot test?
- A. Right eye suppression (Correct Answer)
- B. Crossed diplopia
- C. Uncrossed diplopia
- D. Left eye suppression
Explanation: ***Right eye suppression*** - Seeing **three green dots** exclusively indicates that the patient is only perceiving input from the **left eye**. - In the Worth 4 Dot test, the **left eye** (viewing through a green filter) sees **three green dots**: the white dot at the top (which appears green through the filter) plus the two lateral green dots. - The **right eye** (viewing through a red filter) normally sees **two red dots**: the white dot at the top (which appears red) plus the red dot at the bottom. - Since the patient sees only **three green dots**, the visual input from the **right eye is being suppressed**. *Crossed diplopia* - **Crossed diplopia** (heteronymous diplopia) occurs when the image from the right eye is perceived to the left of the image from the left eye. - This typically occurs with **exotropia** (divergent strabismus) and would result in seeing **five or more dots** (patient perceives both eyes' images but misaligned), not just three green. *Uncrossed diplopia* - **Uncrossed diplopia** (homonymous diplopia) occurs when the image from the right eye is perceived to the right of the image from the left eye. - This is usually associated with **esotropia** (convergent strabismus) and would also lead to the perception of **five or more dots** (both eyes' images perceived but misaligned), not only three green dots. *Left eye suppression* - If there were **left eye suppression**, the patient would see **two red dots** from the right eye only (the white dot appearing red plus the red dot at the bottom). - Seeing **three green dots** confirms the **left eye input is dominant** and the **right eye is suppressed**.
Question 4: A patient presents to the OPD with the finding shown in the image. What is the most likely diagnosis?
- A. Limbal dermoid (Correct Answer)
- B. Pyogenic granuloma
- C. Papilloma
- D. Pinguecula
Explanation: ***Limbal dermoid*** - A **limbal dermoid** is a congenital benign tumor typically found at the **limbus**, the junction between the cornea and sclera. - It appears as a **raised, yellowish-white mass** and may contain elements like hair follicles or sebaceous glands. *Pyogenic granuloma* - A **pyogenic granuloma** is a rapidly growing, benign vascular lesion that typically occurs after trauma or surgery. - It presents as a **red, pedunculated nodule** that bleeds easily, unlike the described finding. *Papilloma* - **Papillomas** are benign epithelial tumors caused by the human papillomavirus (HPV). - They appear as **small, fleshy growths** with a cauliflower-like surface and are less common at the limbus. *Pinguecula* - A **pinguecula** is a common, benign yellowish growth on the conjunctiva, usually located on the nasal side of the cornea. - It does not typically involve the **cornea** or appear as a raised mass like a dermoid tumor.
Question 5: A patient, three years post-surgery, presents with the condition shown in the image and complains of decreased vision. What is the most likely diagnosis?
- A. Corneal Dystrophy
- B. Posterior Subcapsular Cataract (PSC)
- C. Pseudophakic Bullous Keratopathy
- D. Posterior Capsular Opacification (Correct Answer)
Explanation: ***Posterior Capsular Opacification*** - The image (especially part B, the **red reflex view**) shows a cloudy membrane with **Elschnig pearls** and fibrous tissue behind the intraocular lens, which is characteristic of **PCO**. - PCO commonly occurs months to years after cataract surgery and causes **decreased vision** due to scattering of light. *Corneal Dystrophy* - Corneal dystrophies primarily affect the **cornea**, leading to various forms of corneal opacification, and would typically appear as cloudiness or irregularities within the corneal layers. - While it can cause decreased vision, the opacification seen in the image is clearly behind the iris plane and involves the posterior capsule, not the cornea. *Pseudophakic Bullous Keratopathy* - This condition involves **corneal edema** and **bullae formation** due to endothelial cell dysfunction, leading to a hazy cornea. - The image does not show corneal edema or bullae; instead, the primary pathology is located at the **posterior capsule** of the intraocular lens. *Posterior Subcapsular Cataract (PSC)* - A PSC is a type of cataract that forms **before cataract surgery** and affects the natural crystalline lens. - The patient is three years post-surgery, indicating that the natural lens has been replaced, making a PSC (of the natural lens) an impossible diagnosis in this context.
Question 6: Identify the diagnosis based on the clinical image shown.
- A. Horner-Trantas spots
- B. Herbert's pits (Correct Answer)
- C. Pannus
- D. Corneal dystrophy
Explanation: ***Herbert's pits*** - The image displays characteristic **pits at the limbus**, which are a hallmark of healed follicular conjunctivitis, specifically **Herbert's pits**. - These pits are pathognomonic for **trachoma**, a chronic keratoconjunctivitis caused by *Chlamydia trachomatis*. *Horner-Trantas spots* - These are small, raised, gelatinous white dots found at the limbus, typically containing **eosinophils**. - They are characteristic of **vernal keratoconjunctivitis**, an allergic inflammatory condition, and not seen in the provided image. *Pannus* - **Pannus** refers to the growth of **vascularized connective tissue** onto the cornea. - While pannus is also a feature of trachoma, the image specifically shows distinct limbal pits, rather than diffuse vascularization. *Corneal dystrophy* - **Corneal dystrophies** are a group of inherited, bilateral, and progressive corneal disorders that manifest as opacities or structural changes in the cornea. - The findings in the image, such as pits, are inflammatory in origin and distinct from the typically stromal or epithelial changes seen in corneal dystrophies.
Question 7: A patient presents with eye ache and difficulty in vision after watching a movie. What will be the first line of management?
- A. Mannitol with Moxifloxacin
- B. Mannitol with Atropine
- C. Mannitol with lubricating eye drops
- D. Mannitol with Pilocarpine (Correct Answer)
Explanation: ***Mannitol with Pilocarpine*** - This combination is appropriate for **acute angle-closure glaucoma (AACG)**, which can be triggered by pupillary dilation (e.g., in a dark movie theater). **Mannitol** is an osmotic diuretic that rapidly reduces intraocular pressure. - **Pilocarpine** is a miotic agent that constricts the pupil, pulling the iris away from the trabecular meshwork and opening the drainage angle to facilitate aqueous humor outflow. *Mannitol with Moxifloxacin* - While mannitol helps with intraocular pressure, **Moxifloxacin is an antibiotic** used to treat bacterial infections. - There is no indication of an ocular infection in this scenario, so an antibiotic would not be the first-line treatment for sudden eye pain and vision difficulty after watching a movie. *Mannitol with Atropine* - Adding **Atropine, a cycloplegic agent**, would cause further pupillary dilation, which would worsen acute angle-closure glaucoma and increase intraocular pressure. - Atropine is contraindicated in AACG and would exacerbate the patient's condition. *Mannitol with lubricating eye drops* - While mannitol helps with intraocular pressure, **lubricating eye drops** are used for dry eyes or surface irritation, not for acute angle-closure glaucoma. - Lubricating drops do not address the underlying pathology of increased intraocular pressure due to angle closure.
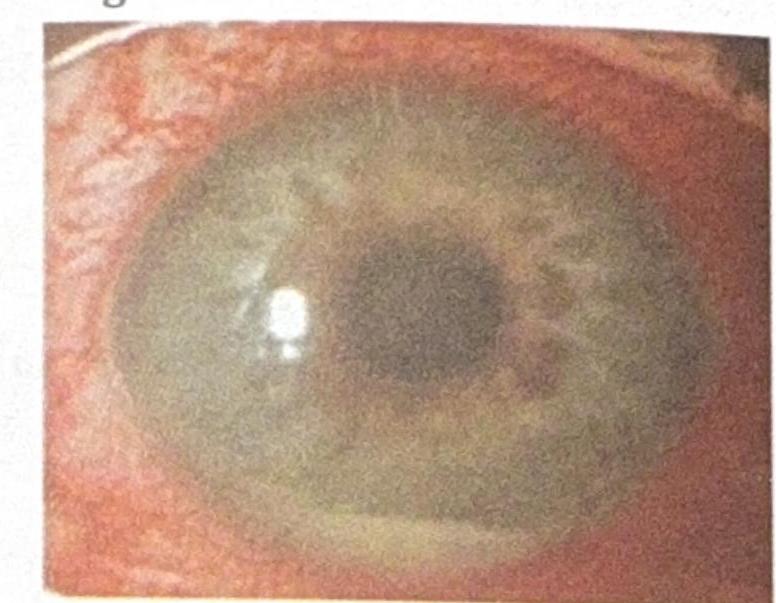
Question 8: A patient presents with sudden painful diminution of vision, difficulty looking in light (photophobia), and circumcorneal congestion with hypopyon. What is the most likely diagnosis?
- A. Acute conjunctivitis
- B. Episcleritis
- C. Acute congestive glaucoma
- D. Acute anterior uveitis (Correct Answer)
Explanation: ***Acute anterior uveitis*** - The constellation of **sudden painful diminution of vision**, **photophobia**, **circumcorneal congestion**, and **hypopyon** (pus in the anterior chamber, visible as a whitish fluid level in the image) is highly characteristic of acute anterior uveitis. - This condition involves inflammation of the iris and ciliary body, leading to these severe symptoms and signs. *Acute conjunctivitis* - Characterized by **redness**, **itching**, and **discharge**, but typically lacks significant pain, photophobia, or vision loss. - Hypopyon is not a feature of acute conjunctivitis; the congestion is diffuse and not pericorneal. *Episcleritis* - Presents with **localized redness** and mild discomfort, but generally without pain, photophobia, or vision changes. - Episcleritis does not typically involve the anterior chamber with hypopyon. *Acute congestive glaucoma* - Involves severe eye pain, blurred vision, ciliary congestion, and often a **fixed, mid-dilated pupil** due to acutely elevated intraocular pressure. - While it shares some symptoms like pain, photophobia, and blurred vision, **hypopyon is not a typical finding** in acute congestive glaucoma, which differentiates it from uveitis.
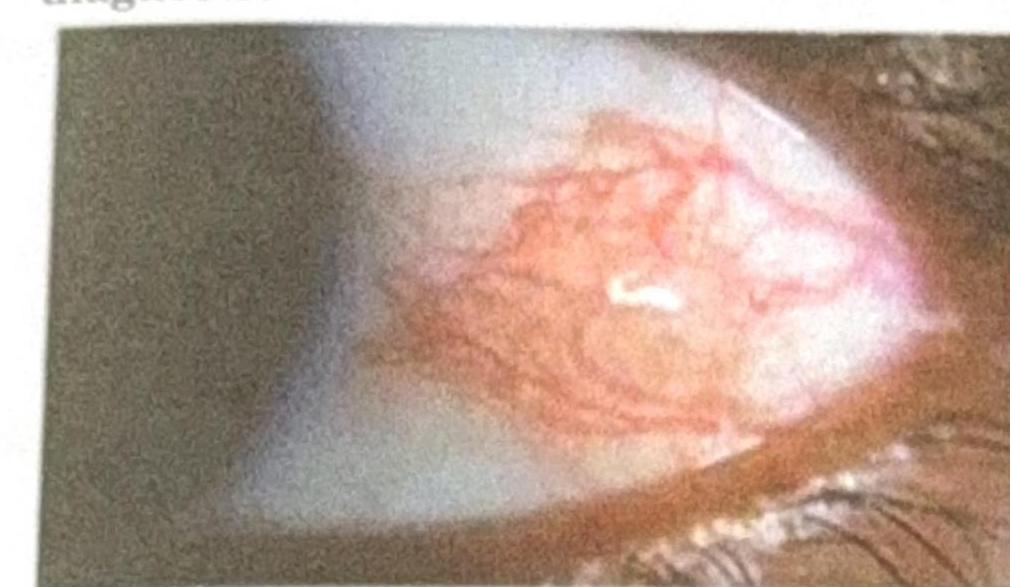
Question 9: A patient presents with a nodular swelling near the limbus, which does not blanch with topical vasoconstrictors and recurs after treatment. Based on the image and clinical presentation, what is the most probable diagnosis?
- A. Scleritis with rheumatoid arthritis (Correct Answer)
- B. Episcleritis with rheumatoid arthritis
- C. Pinguecula
- D. Dry eye
Explanation: ***Scleritis with rheumatoid arthritis*** - The image shows **deep, violaceous conjunctival injection** with surrounding edema and a nodular appearance near the limbus, consistent with **nodular scleritis**. Scleritis is inflammation of the sclera, often characterized by severe pain and association with systemic autoimmune diseases like **rheumatoid arthritis**, which can cause destructive lesions and recurrence. - The characteristic **deep vessel engorgement that does not blanch with phenylephrine** and the history of recurrence further support scleritis. *Episcleritis with rheumatoid arthritis* - Episcleritis presents with a **more superficial, bright red injection** involving the episclera, which generally **blanches with topical phenylephrine** and is less painful than scleritis. - While episcleritis can be associated with rheumatoid arthritis, the clinical features described (nodular swelling, deep injection) are more typical of scleritis. *Pinguecula* - A pinguecula is a **yellowish patch or bump** on the conjunctiva, typically on the nasal side of the eye, that is **not inflamed** unless irritated. - It consists of **degenerated collagen fibers** and elastic tissue, and does not present with the diffuse, deep vascular injection seen in the image. *Dry eye* - Dry eye is characterized by **ocular dryness, irritation, and sometimes a foreign body sensation**, but it typically causes **diffuse conjunctival hyperemia** rather than a localized, nodular, deep inflammation with surrounding edema as shown. - While dry eye can be associated with autoimmune diseases, its appearance is not consistent with the depicted nodular lesion.