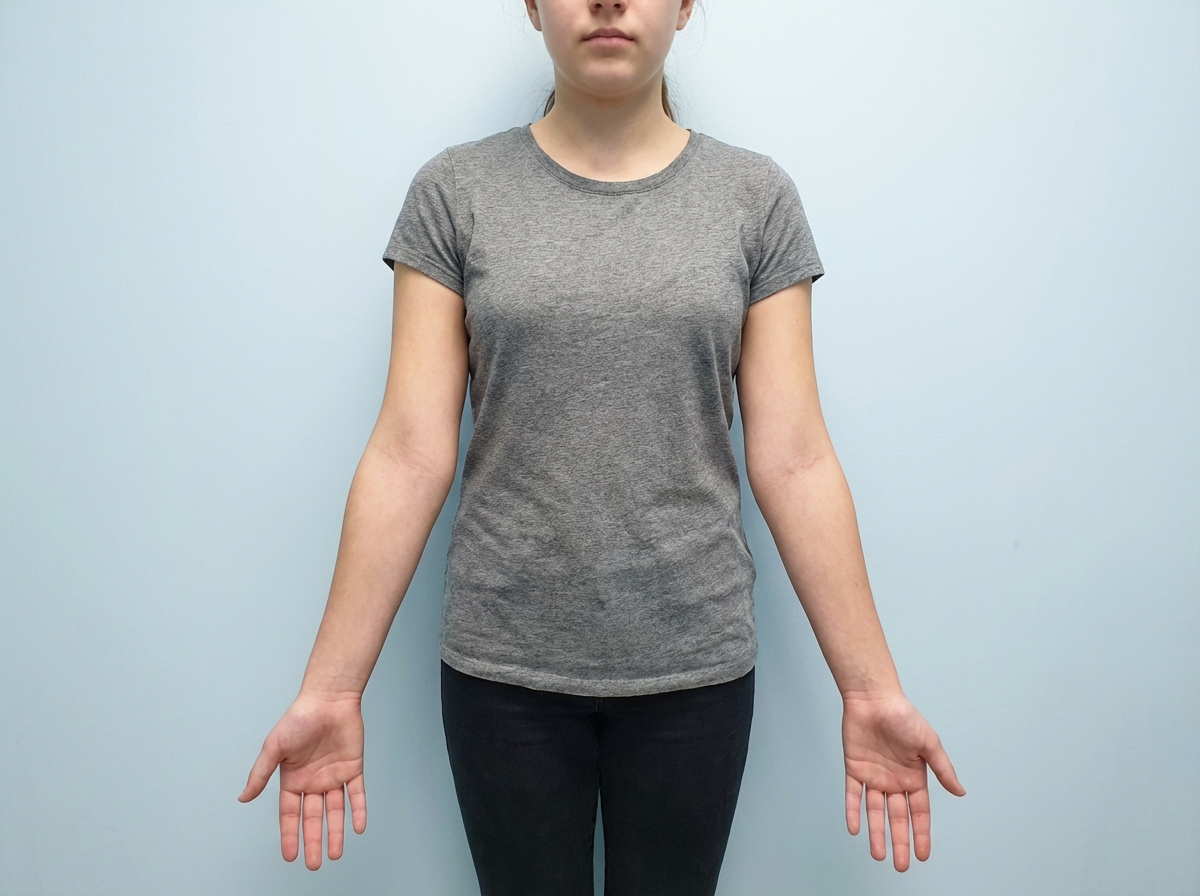
A teenage girl presents with a history of amenorrhea. Local examination is shown in the image. What karyotype analysis would you consider for further evaluation?
A female presents with postcoital bleeding. Which of the following is the most appropriate investigation?
A woman at 8 weeks of gestation is diagnosed with hyperthyroidism. Which of the following is the most appropriate treatment option?
A 32-year-old female in late pregnancy presents with seizures and high blood pressure. She is diagnosed with eclampsia and started on magnesium sulfate therapy. As part of her management, certain parameters require close monitoring to prevent magnesium toxicity. Which of the following is the MOST important parameter to monitor during magnesium sulfate therapy in this patient?
A 27 -week pregnant woman with a fetus diagnosed with congenital anomalies is considering a Medical Termination of Pregnancy (MTP). Whose presence is not required for the authorization of MTP in this case?
A USG (ultrasound) shows two babies, one of whom appears to be one month older than the other. What is the term for this condition?