NEET-PG 2024 — OB/GYN
16 Previous Year Questions with Answers & Explanations
A 30-year-old woman presents with a history of pelvic pain and infertility. A transvaginal ultrasound is performed, and the image provided shows a tubular, fluid-filled structure with thin walls. There is no evidence of solid components or internal septations. What is the most likely diagnosis?
A 25-year-old pregnant woman, at 18 weeks of gestation, undergoes a routine ultrasound scan. The ultrasound images provided show below. Based on the imaging findings, what is the most likely diagnosis?
What is the typical time between fertilization and implantation?
A pregnant woman with a known case of asthma is experiencing postpartum hemorrhage (PPH). Which drug is contraindicated?
In fertility-preserving prolapse surgery, which bony landmark is used for suspension?
A 45-year-old woman presents with a history of cervical erosion and spotting for the past 2 months. What is the next best step?
A GSP4 woman comes for routine sonography for the first time. She has four daughters and expresses a desire for a boy this time, asking for sex determination. To abide by ethical guidelines, what should you do?
A young woman presents with prolapse, and a mesh is being placed. Where is this mesh typically fixed to?
Which of the following is a tumor marker associated with ovarian solid-cystic masses?
A 32-year-old woman presents with a new 2 cm black nodular mass near her episiotomy scar. She reports that the mass is painful and tends to increase in size during menstruation. What is the most likely diagnosis?
NEET-PG 2024 - OB/GYN NEET-PG Practice Questions and MCQs
Question 1: A 30-year-old woman presents with a history of pelvic pain and infertility. A transvaginal ultrasound is performed, and the image provided shows a tubular, fluid-filled structure with thin walls. There is no evidence of solid components or internal septations. What is the most likely diagnosis?
- A. Ovarian cyst
- B. Ectopic pregnancy
- C. Hydrosalpinx (Correct Answer)
- D. Endometrioma
- E. Tubo-ovarian abscess
Explanation: ***Hydrosalpinx*** - The ultrasound finding of a **tubular, fluid-filled structure with thin walls** and no solid components or septations is highly characteristic of a **hydrosalpinx**, which is a blocked, fluid-filled fallopian tube. - **Pelvic pain** and **infertility** in a young woman are classic clinical presentations associated with hydrosalpinx, often resulting from previous pelvic inflammatory disease. *Ovarian cyst* - While ovarian cysts are fluid-filled, they typically appear as **rounded or oval structures within or adjacent to the ovary**, not distinctively tubular. - They can cause pain but are not typically associated with a "tubular" morphology on ultrasound. *Ectopic pregnancy* - An ectopic pregnancy would typically present with a **gestational sac** (with or without a fetal pole or yolk sac) outside the uterus, often in the fallopian tube. - While it can be tubular, it usually shows more complex internal echoes representing pregnancy components, and the clinical picture would involve a **positive pregnancy test** and often acute, unilateral pain. *Endometrioma* - An endometrioma is a type of ovarian cyst filled with **endometrial tissue**, often appearing on ultrasound as a **"ground glass" or "chocolate cyst"** with internal echoes due to old blood. - It would not typically present as a thin-walled, anechoic (purely fluid-filled) tubular structure. *Tubo-ovarian abscess* - A tubo-ovarian abscess (TOA) is a **complex inflammatory mass** that typically appears on ultrasound as a **thick-walled, complex structure with internal echoes, septations, or debris**. - TOA patients usually present with **acute symptoms including fever, elevated white blood cell count**, and severe pelvic pain, rather than the chronic presentation described here. - The ultrasound description of thin walls and no solid components makes TOA unlikely.
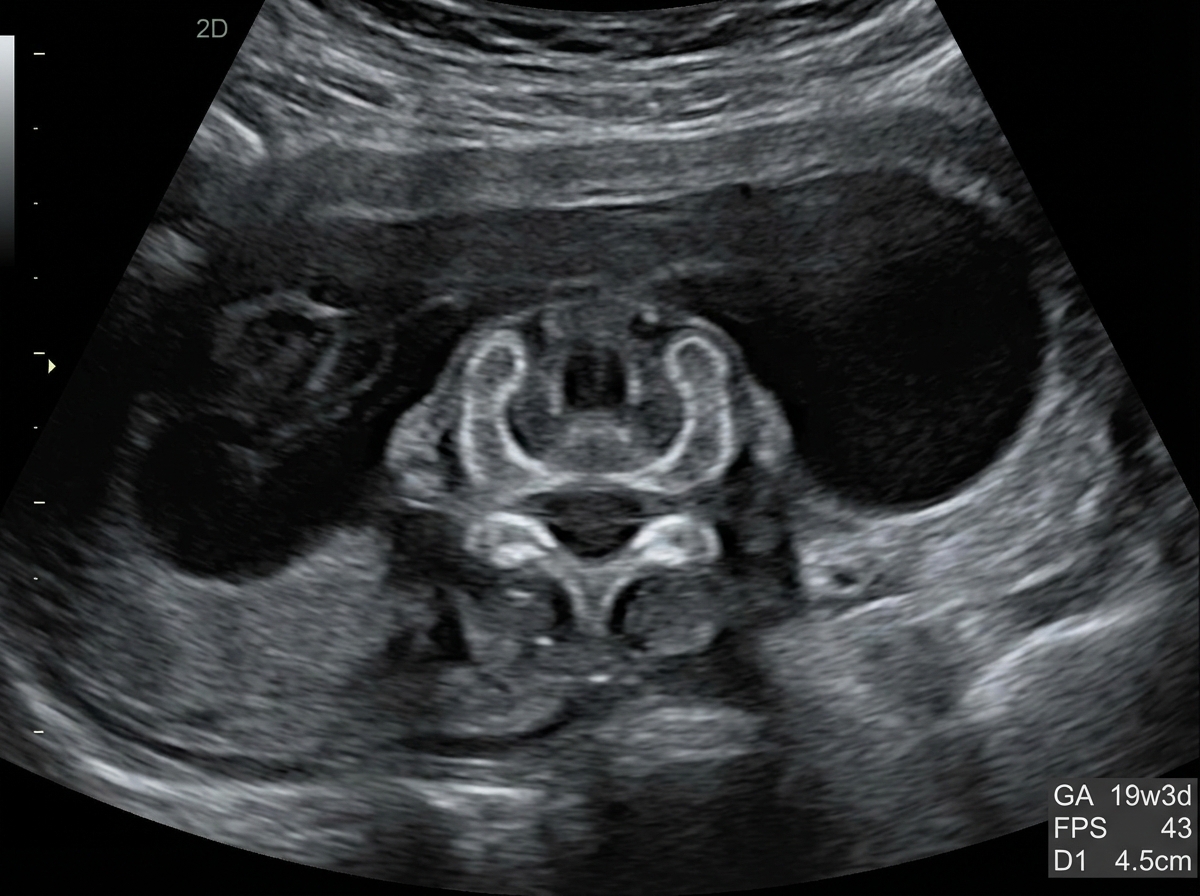
Question 2: A 25-year-old pregnant woman, at 18 weeks of gestation, undergoes a routine ultrasound scan. The ultrasound images provided show below. Based on the imaging findings, what is the most likely diagnosis?
- A. Spina bifida (Correct Answer)
- B. Anencephaly
- C. Encephalocele
- D. Holoprosencephaly
- E. Iniencephaly
Explanation: ***Spina bifida*** - The ultrasound image shows a **defect in the posterior elements of the fetal spine**, with characteristic splaying or widening of the vertebral arches. - This is a **neural tube defect** resulting from incomplete closure of the spinal column during embryonic development. - Associated findings on prenatal ultrasound may include the **"lemon sign"** (scalloping of frontal bones) and **"banana sign"** (abnormal cerebellar shape). - Spina bifida is typically detected on **second-trimester anatomy scan** (18-20 weeks). *Anencephaly* - This condition involves the **absence of a major portion of the brain, skull, and scalp** due to failure of anterior neural tube closure. - On ultrasound, anencephaly presents with **absent calvarium above the orbits** and absent cerebral hemispheres, which is distinctly different from a spinal defect. - This would be a **cranial abnormality**, not a spinal column defect. *Encephalocele* - An **encephalocele** is a protrusion of brain tissue and meninges through a defect in the skull, most commonly at the **occipital region**. - On ultrasound, this appears as a **cranial mass** extending beyond the skull contour, not a spinal defect. *Holoprosencephaly* - This condition results from **failure of forebrain (prosencephalon) to divide properly** into two hemispheres. - Ultrasound findings include **single ventricle**, fused thalami, and absent midline structures, often with associated **facial anomalies**. - The imaging would show **brain abnormalities**, not spinal column defects. *Iniencephaly* - This is a rare **neural tube defect** characterized by extreme retroflexion of the head with severe spinal defects in the cervical and thoracic regions. - On ultrasound, iniencephaly shows the fetal head in extreme **hyperextension** with the face looking upward, creating a characteristic "stargazing" appearance. - This differs from the typical spinal defect pattern seen in spina bifida.
Question 3: What is the typical time between fertilization and implantation?
- A. 2 days
- B. 8 days (Correct Answer)
- C. 14 days
- D. 16 days
Explanation: ***8 days*** - **Fertilization** typically occurs in the **fallopian tube**, and the resulting **zygote** then undergoes several cell divisions while migrating towards the uterus. - Implantation, the process by which the **blastocyst embeds into the uterine wall**, usually begins around day 6 post-fertilization and is completed by day 8-10. *2 days* - At 2 days post-fertilization, the embryo is typically in the **2-cell to 4-cell stage** and is still located within the fallopian tube, far from the implantation site. - This stage is too early for implantation to occur, as the embryo has not yet reached the **blastocyst stage** or the uterus. *14 days* - By 14 days post-fertilization, implantation would have long been completed, and the initial stages of **trophoblast development** and formation of the **placenta** would be underway. - This time frame represents a more advanced stage of pregnancy, whereas implantation is an early event. *16 days* - Sixteen days post-fertilization is well past the window for initial implantation; at this point, significant embryonic development has occurred, and the woman might even be experiencing early signs of **pregnancy**, such as a missed period. - Implantation is a much earlier process, concluding by day 10 at the latest.
Question 4: A pregnant woman with a known case of asthma is experiencing postpartum hemorrhage (PPH). Which drug is contraindicated?
- A. Methyl ergometrine
- B. Carboprost (Correct Answer)
- C. Misoprostol
- D. Oxytocin
Explanation: ***Carboprost*** - **Carboprost** is a **prostaglandin F2-alpha analog** that causes strong uterine contractions but also leads to **bronchoconstriction** and increased airway resistance. - Due to its potent bronchoconstrictive effects, **carboprost** is **absolutely contraindicated in patients with asthma** as it can precipitate a severe asthmatic attack. *Methyl ergometrine* - **Methyl ergometrine** is an **ergot alkaloid** that causes sustained uterine contractions and is effective for PPH. - It is contraindicated in patients with **hypertension** or **pre-eclampsia** due to its vasoconstrictive properties, but not typically in asthma. *Misoprostol* - **Misoprostol** is a **prostaglandin E1 analog** used for PPH management, causing uterine contractions. - It is generally safe for use in patients with asthma as it does not have significant bronchoconstrictive side effects. *Oxytocin* - **Oxytocin** is a first-line uterotonic agent for PPH, working by causing rhythmic uterine contractions. - It is generally considered safe in patients with asthma and is not known to exacerbate respiratory conditions.
Question 5: In fertility-preserving prolapse surgery, which bony landmark is used for suspension?
- A. Sacral promontory
- B. Ischial spine (Correct Answer)
- C. Pubic symphysis
- D. Ischial tuberosity
Explanation: ***Ischial spine*** - The **ischial spine** serves as a crucial anatomical landmark for **suspension in fertility-preserving prolapse surgery**, particularly for procedures like sacrospinous ligament fixation. - Fixation to the ischial spine helps in supporting the vaginal apex or uterus, maintaining the natural vaginal axis and reducing the risk of recurrence. *Sacral promontory* - The **sacral promontory** is used in sacrocolpopexy or sacrohysteropexy, which traditionally involves mesh fixation and may not be ideal for **fertility preservation** due to potential future pregnancy complications or mesh-related issues. - While it provides strong support, its use might reduce vaginal elasticity and increase risk for future deliveries. *Pubic symphysis* - The **pubic symphysis** is primarily involved in procedures for **stress urinary incontinence** (e.g., tension-free vaginal tape) and is not a primary point for suspending the uterus or vaginal apex in prolapse surgery. - Using it for prolapse repair could alter the normal anatomical relationship and lead to dyspareunia or chronic pain. *Ischial tuberosity* - The **ischial tuberosity** is a bony prominence that provides attachment for various ligaments and muscles of the pelvis and perineum but is **too inferior and lateral** to be effectively used for uterine or vaginal vault suspension. - Its location makes it unsuitable for achieving appropriate apical support in prolapse surgery.
Question 6: A 45-year-old woman presents with a history of cervical erosion and spotting for the past 2 months. What is the next best step?
- A. LBC + HPV (Correct Answer)
- B. Pap smear + HSV
- C. Pap smear + HBV
- D. LBC + HSV
Explanation: ***LBC + HPV*** - Cervical erosion and spotting are concerning for **cervical intraepithelial neoplasia (CIN)** or **cervical cancer**, making **Liquid-Based Cytology (LBC)** the appropriate screening method. - **Human Papillomavirus (HPV) testing** is crucial as persistent high-risk HPV infection is the primary cause of cervical cancer and helps in risk stratification and management. *Pap smear + HSV* - A **routine Pap smear** (conventional cytology) is less sensitive than LBC for detecting abnormal cervical cells and is generally being phased out by LBC. - **Herpes Simplex Virus (HSV)** causes genital herpes and is not directly associated with cervical cancer, thus testing for it in this context is not the most appropriate immediate next step. *Pap smear + HBV* - As mentioned, a **routine Pap smear** is not the preferred method for cervical cancer screening compared to LBC. - **Hepatitis B Virus (HBV)** causes liver disease and is entirely unrelated to cervical pathology; therefore, testing for it would be irrelevant to the patient's symptoms. *LBC + HSV* - While **LBC** is the correct advanced cytology method, adding **HSV testing** is not indicated as HSV does not cause cervical cancer or intraepithelial lesions that present with cervical erosion and spotting. - Focus should be on identifying potential malignancy or pre-malignant changes with HPV co-testing, not sexually transmitted infections unrelated to cancer risk.
Question 7: A GSP4 woman comes for routine sonography for the first time. She has four daughters and expresses a desire for a boy this time, asking for sex determination. To abide by ethical guidelines, what should you do?
- A. Check routine ANC and sex for developmental abnormalities and do not reveal gender to the patient (Correct Answer)
- B. Check routine ANC and sex for developmental abnormalities and do reveal gender to the patient
- C. Do reveal gender if a girl
- D. Check only routine ANC, do not check sex
Explanation: ***Check routine ANC and sex for developmental abnormalities and do not reveal gender to the patient*** - It is **illegal** and **unethical** to reveal the sex of the fetus in many countries, including India, to prevent **sex-selective abortions**. - The primary purpose of a routine antenatal ultrasound is to assess fetal **health** and **developmental abnormalities**, not to determine sex for parental preference. *Check routine ANC and sex for developmental abnormalities and do reveal gender to the patient* - Revealing the gender to the patient directly facilitates **sex-selective abortion**, which is medically unethical and illegal due to the potential for harm to the fetus and society. - This practice would violate the **Pre-Conception and Pre-Natal Diagnostic Techniques (PCPNDT) Act** in India, which prohibits gender determination. *Do reveal gender if a girl* - Revealing the gender, regardless of whether it is a boy or a girl, can lead to **gender-biased selective abortions**, particularly in cultures with a strong preference for male offspring. - This action undermines the ethical principles of **non-maleficence** and **justice** by potentially facilitating harm based on gender preference. *Check only routine ANC, do not check sex* - While the primary focus is routine antenatal care, avoiding the assessment of fetal sex entirely could lead to **missing potential developmental abnormalities** that might be identifiable through observation of external genitalia. - A thorough ultrasound examination routinely includes a visual check of fetal anatomy, which can incidentally reveal gender, but this information should not be shared with the parents for selection purposes.
Question 8: A young woman presents with prolapse, and a mesh is being placed. Where is this mesh typically fixed to?
- A. Ischial spine
- B. Ischial tuberosity
- C. Sacral promontory (Correct Answer)
- D. Pubic symphysis
Explanation: ***Sacral promontory*** - In **sacrocolpopexy**, a common surgical procedure for vaginal prolapse, a mesh is attached from the vaginal apex to the **anterior longitudinal ligament** overlying the **sacral promontory**. - This anatomical landmark provides a strong, stable point of fixation to support the vagina and prevent recurrence of prolapse. *Ischial spine* - The **ischial spine** is a common landmark for identifying the **pudendal nerve** and for performing a **pudendal nerve block**, not for mesh fixation in prolapse repair. - It is also relevant in measuring the **interspinous diameter** of the pelvis during childbirth, but not for surgical mesh attachment in this context. *Ischial tuberosity* - The **ischial tuberosity** is the bony prominence on which one sits and is an attachment point for various muscles of the **thigh** and **pelvic floor**. - It is not used as a primary fixation point for mesh in vaginal prolapse repair due to its position and lack of direct support for the vaginal apex. *Pubic symphysis* - The **pubic symphysis** is a cartilaginous joint connecting the two **pubic bones** in the anterior pelvis. - While part of the pelvic framework, it does not provide the appropriate superior posterior support needed for **vaginal apex suspension** in prolapse surgery.
Question 9: Which of the following is a tumor marker associated with ovarian solid-cystic masses?
- A. CEA
- B. HCG
- C. HER2/neu
- D. AFP (Correct Answer)
Explanation: ***AFP (Alpha-fetoprotein)*** - **AFP** is a reliable tumor marker for differentiating **germ cell tumors**, especially **yolk sac tumors**, which often present as an ovarian solid-cystic mass. - Elevated **AFP** levels help in diagnosis, monitoring treatment response, and detecting recurrence of these specific ovarian malignancies. *CEA (Carcinoembryonic antigen)* - **CEA** is primarily associated with **gastrointestinal cancers**, such as colorectal cancer, and is less specific for ovarian masses. - While it can be elevated in some mucinous ovarian carcinomas, it's not the most specific marker for a general solid-cystic ovarian mass. *HCG (Human chorionic gonadotropin)* - **HCG** is a key marker for **gestational trophoblastic disease** and some **germ cell tumors**, such as choriocarcinoma. - It is not typically elevated in most common solid-cystic ovarian masses, especially those of epithelial origin. *HER2/neu (Human Epidermal growth factor Receptor 2)* - **HER2/neu** is primarily associated with **breast cancer** and some gastric cancers, playing a role in targeted therapy. - It is not a standard tumor marker for the general evaluation or diagnosis of ovarian solid-cystic masses.
Question 10: A 32-year-old woman presents with a new 2 cm black nodular mass near her episiotomy scar. She reports that the mass is painful and tends to increase in size during menstruation. What is the most likely diagnosis?
- A. Melanoma
- B. Foreign body granuloma
- C. Inclusion cyst
- D. Endometriosis (Correct Answer)
Explanation: ***Endometriosis*** - The location near an **episiotomy scar**, the **painful black nodular mass**, and its tendency to **increase in size during menstruation** are highly characteristic of an **episiotomy scar endometriosis**, also known as cutaneous endometriosis. - This condition involves the presence of **endometrial tissue** outside the uterus, which responds to hormonal fluctuations, explaining the cyclical pain and size changes. *Melanoma* - While a **black nodular mass** could suggest melanoma, the key differentiating factor here is the **cyclical pain and growth with menstruation**, which is not typical for melanoma. - Melanoma is a **malignant tumor** of melanocytes and usually presents with irregular borders, asymmetry, and color variation, without a direct correlation to the menstrual cycle. *Foreign body granuloma* - A **foreign body granuloma** is an inflammatory reaction to non-degradable foreign material, which could be seen at a surgical site like an episiotomy. - However, this condition typically doesn't exhibit the **cyclical pain and growth with menstruation** that is a hallmark of endometriosis. *Inclusion cyst* - An **inclusion cyst** is a benign cyst that develops when epithelial cells become trapped under the skin surface after trauma or surgery. - While it can occur at an episiotomy site, it is usually a **slow-growing mass** that is typically painless (unless infected) and does not fluctuate in size or pain with the menstrual cycle.