What is the most common cause of death in idiopathic pulmonary fibrosis (IPF)?
A patient presents with large sweaty hands, macroglossia, and frontal bossing. What is the best test for confirmation of the diagnosis?
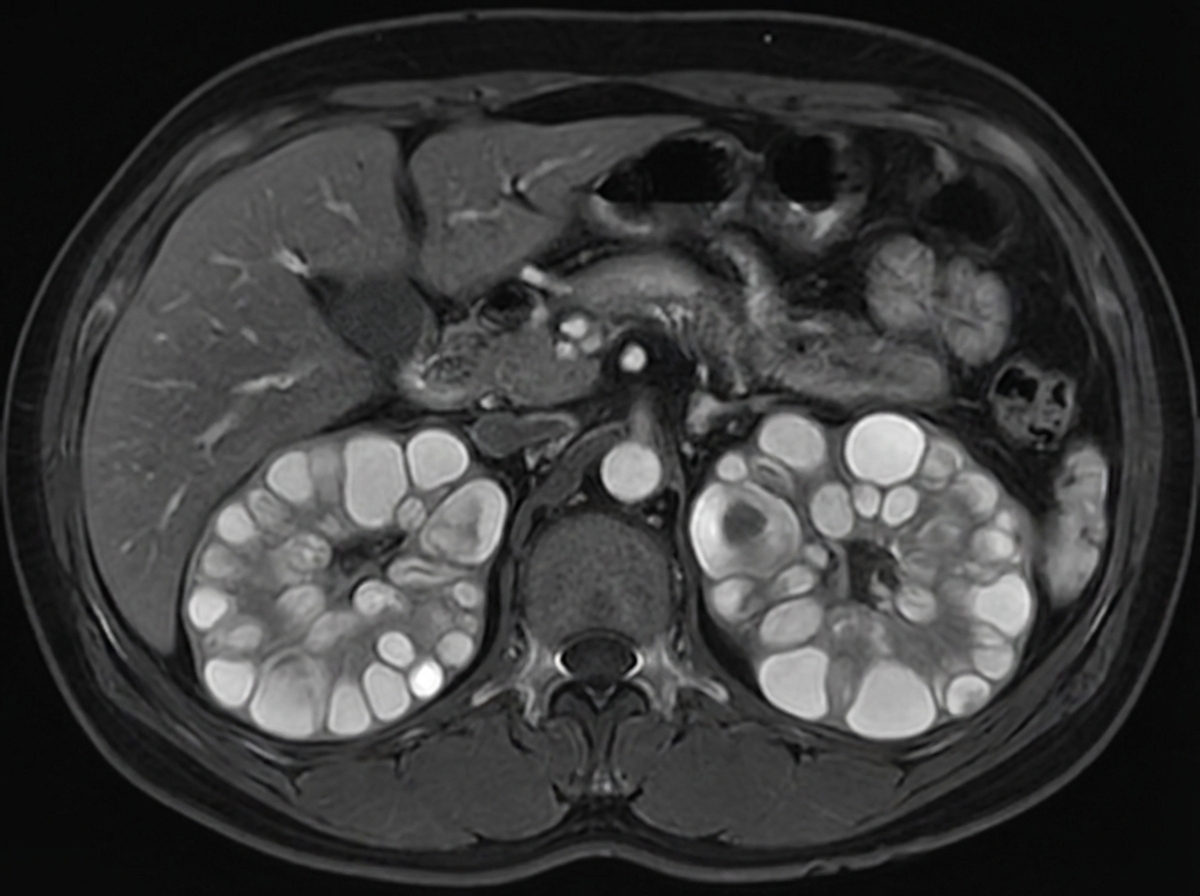
A 45-year-old patient presents with hypertension, hematuria, and flank pain. An MRI scan is performed, and the image provided shows multiple cystic lesions in both kidneys. What is the most likely diagnosis?
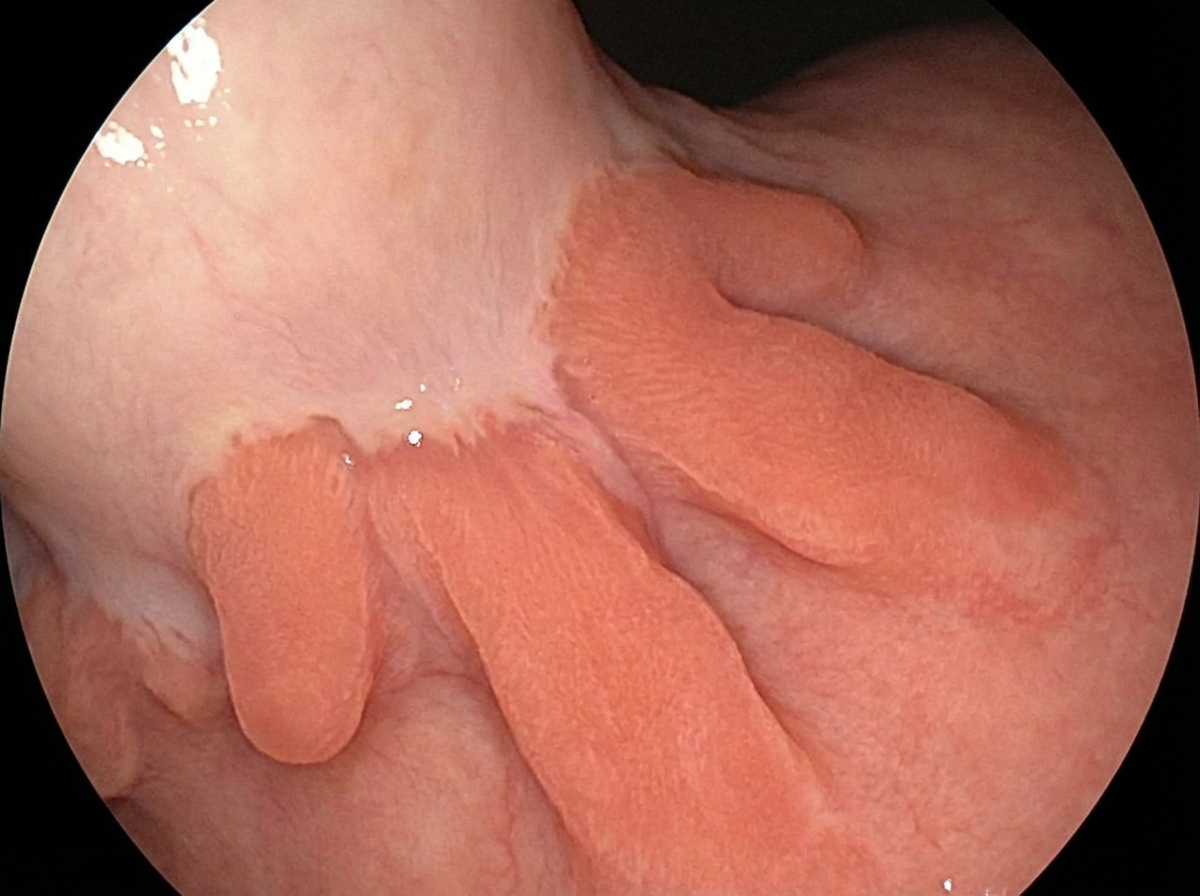
An endoscopic image shows the following finding. What is the most likely diagnosis?
A 40-year-old farmer presents with fever, calf tenderness, conjunctival suffusion, retro-orbital pain, and hypokalemia. What is the diagnosis?
Which of the following antibodies is associated with Celiac disease?
Which of the following is typically observed in the investigation results for a patient with iron deficiency anemia (IDA)?
An adult female presents with pallor and fatigue. Blood investigations show low hemoglobin ( Hb ), low serum iron, low ferritin, low transferrin saturation, and increased total iron-binding capacity (TIBC). What is the likely diagnosis?
A 32-year-old female presents with a 2-month history of progressive, painless swelling in the left side of her neck. She also reports low-grade fever, night sweats, and unintentional weight loss. Physical examination reveals a firm, non-tender, immobile mass in the left cervical region, and multiple smaller lymph nodes in the supraclavicular area. Chest X-ray shows mediastinal widening, and a lymph node biopsy confirms the presence of Reed-Sternberg cells. What is the most appropriate management for this patient?
A patient presents with itchy skin lesions with blistering along with gastrointestinal issues. Which of the following is the most specific serological test for this condition?