NEET-PG 2024 — Anesthesiology
7 Previous Year Questions with Answers & Explanations
What is the purpose of Positive End-Expiratory Pressure (PEEP)?
What is the staging system used for the condition seen in the patient after a history of intubation, as shown in the image?
What is the name of the nerve block technique shown in the image?
A patient presented with rigidity, tremors, and trismus after being administered an anesthetic agent. Which anesthetic agent is most likely to have been administered?
In which clinical scenario would you find a patient requiring the vital signs assessment technique shown in the image?

A patient with mild to moderate renal failure requires reversal of muscle relaxation induced by vecuronium. Which of the following drugs is appropriate for this purpose?
What is the pressure required to open the device shown in the image?

NEET-PG 2024 - Anesthesiology NEET-PG Practice Questions and MCQs
Question 1: What is the purpose of Positive End-Expiratory Pressure (PEEP)?
- A. To prevent atelectasis (Correct Answer)
- B. To decrease preload
- C. To increase venous return
- D. To increase respiratory rate (RR)
Explanation: ***To prevent atelectasis*** - PEEP maintains a positive pressure in the airways at the end of exhalation, which helps to keep **alveoli open** and prevents their collapse. - This recruitment of collapsed alveoli improves **oxygenation** and reduces the work of breathing. *To decrease preload* - While PEEP can indirectly decrease cardiac preload by increasing intrathoracic pressure, its primary purpose is not cardiovascular but rather respiratory. - The impact on preload is a potential side effect that requires careful monitoring, especially in patients with compromised cardiac function. *To increase venous return* - PEEP actually tends to **decrease venous return** due to increased intrathoracic pressure compressing the vena cava and reducing the pressure gradient for blood flow back to the heart. - This can lead to a reduction in cardiac output, which is a potential adverse effect. *To increase respiratory rate (RR)* - PEEP does not directly increase the respiratory rate; instead, it is a setting on a mechanical ventilator that affects lung volumes and oxygenation. - Respiratory rate is typically set independently or influenced by the patient's ventilatory drive.
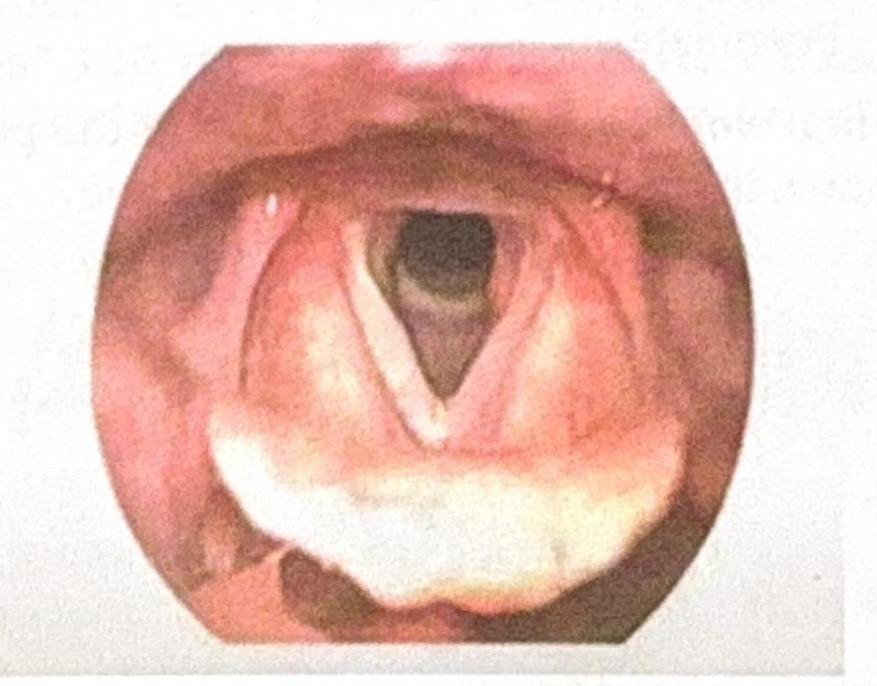
Question 2: What is the staging system used for the condition seen in the patient after a history of intubation, as shown in the image?
- A. Cormack and Lehane (Correct Answer)
- B. AJCC
- C. TNM
- D. Radkowski
Explanation: ***Cormack and Lehane*** - The **Cormack and Lehane classification** system is used to grade the view of the **larynx** during **direct laryngoscopy** for intubation. - Given the history of intubation and the image showing the laryngeal view, this system is the most appropriate for staging the visual difficulty or success of intubation. *AJCC* - The **American Joint Committee on Cancer (AJCC) staging system** is primarily used for **oncological staging**, classifying the extent of cancer. - It is not relevant for assessing the view of the larynx during intubation. *TNM* - **TNM staging** (Tumor, Node, Metastasis) is a widely used system for classifying the **progression of cancer**. - This system is specific to cancer staging and is not applicable to the assessment of airways for intubation. *Radkowski* - The **Radkowski staging system** is used to classify **pediatric subglottic stenosis**, a narrowing of the airway below the vocal cords. - While it deals with airway issues, the question focuses on the view during intubation, not the severity of subglottic stenosis, and the image does not specifically point to this condition.
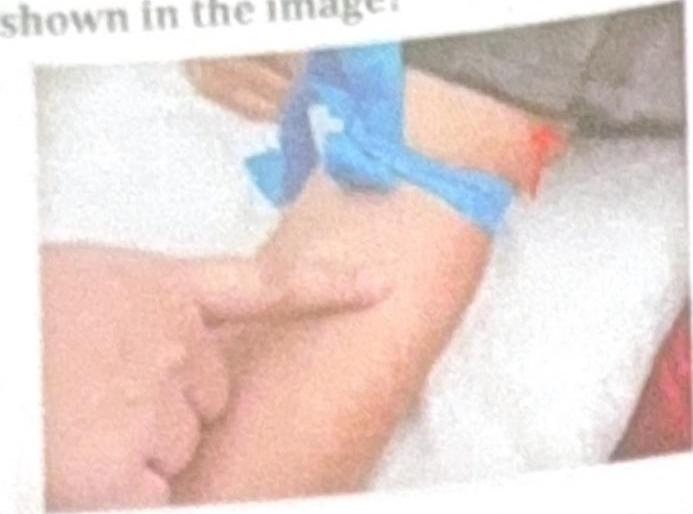
Question 3: What is the name of the nerve block technique shown in the image?
- A. Intra-arterial anesthesia (Correct Answer)
- B. Bier's block
- C. Regional anesthesia
- D. Axillary block
Explanation: ***Intra-arterial anesthesia*** - The image shows a **cannula inserted directly into an artery**, indicated by the blood reflux and the context of anesthesia, suggesting direct drug delivery into the arterial system. - This method is used for specific types of regional pain management or diagnostic procedures where direct arterial access is required for **localized drug distribution**. *Bier's block* - A Bier's block, or **intravenous regional anesthesia**, involves injecting local anesthetic into a **vein** in an extremity after it has been exsanguinated and isolated by a tourniquet. - The image clearly shows a **bright red blood flash**, characteristic of arterial cannulation, not venous. *Regional anesthesia* - This is a broad term referring to the **anesthesia of a specific region** of the body and encompasses various techniques. - While intra-arterial anesthesia is a type of regional anesthesia, "regional anesthesia" itself is too general to specifically describe the technique shown. *Axillary block* - An **axillary block** is a type of peripheral nerve block targeting the brachial plexus in the axilla to anesthetize the arm. - The image does not depict the axillary region or the characteristic needle placement for an axillary block; instead, it shows direct vascular access.
Question 4: A patient presented with rigidity, tremors, and trismus after being administered an anesthetic agent. Which anesthetic agent is most likely to have been administered?
- A. Halothane (Correct Answer)
- B. Nitrous Oxide (N2O)
- C. Thiopentone sodium
- D. Etomidate
Explanation: ***Halothane*** - The combination of **rigidity**, **tremors**, and **trismus** after an anesthetic agent suggests **malignant hyperthermia (MH)**, a rare but life-threatening inherited condition. - **Halothane (and other volatile anesthetics)**, along with succinylcholine, are known triggers for malignant hyperthermia. *Nitrous Oxide (N2O)* - While an anesthetic agent, **nitrous oxide** is not a known trigger for **malignant hyperthermia**. - It works by modulating **NMDA receptors** and does not typically cause rigidity, tremors, or trismus as a side effect. *Thiopentone sodium* - **Thiopentone sodium** is a **barbiturate** anesthetic and is not associated with triggering **malignant hyperthermia**. - Its effects primarily involve potentiation of **GABA-A receptors**, leading to sedation and hypnosis. *Etomidate* - **Etomidate** is a short-acting intravenous anesthetic that is not a known trigger for **malignant hyperthermia**. - It is typically associated with minimal cardiovascular depression but can cause **adrenocortical suppression** with prolonged use.
Question 5: In which clinical scenario would you find a patient requiring the vital signs assessment technique shown in the image?
- A. Pulse absent, breath present
- B. Pulse and breath both not present
- C. Pulse and breath present
- D. Pulse present, breath absent (Correct Answer)
Explanation: ***Pulse present, breath absent*** - The image depicts a **mouth-to-mouth resuscitation** technique, specifically rescue breaths being administered by one person to another. - This technique is applied when a person has a **detectable pulse** but is **not breathing** or is only gasping, indicating respiratory arrest while the heart is still circulating blood. *Pulse absent, breath present* - This scenario would represent **cardiac arrest** where the heart has stopped, but the person is still attempting to breathe. This is a rare, transient state. - In such a case, the primary intervention would be **chest compressions**, not just rescue breathing, as circulation is the immediate priority. *Pulse and breath both not present* - This describes **cardiopulmonary arrest (CPA)**, where both the heart and lungs have ceased functioning. - The appropriate intervention is **cardiopulmonary resuscitation (CPR)**, which involves a combination of **chest compressions and rescue breaths (30:2 ratio)**, not just rescue breaths alone. *Pulse and breath present* - If both vital signs are present, the person is **conscious and breathing adequately**, or unconscious but breathing normally. - No advanced respiratory intervention like mouth-to-mouth resuscitation is needed; the priority would be maintaining their airway and monitoring their condition.
Question 6: A patient with mild to moderate renal failure requires reversal of muscle relaxation induced by vecuronium. Which of the following drugs is appropriate for this purpose?
- A. Physostigmine
- B. Rivastigmine
- C. Sugammadex (Correct Answer)
- D. Succinylcholine
Explanation: ***Sugammadex*** - **Sugammadex** is a modified gamma-cyclodextrin that forms a tight, water-soluble complex with **steroidal non-depolarizing neuromuscular blocking agents** like vecuronium, effectively encapsulating and inactivating them. - Its elimination is primarily renal, but even in **mild to moderate renal failure**, its rapid binding to vecuronium and lack of active metabolites make it a safe and effective choice for reversal. *Physostigmine* - **Physostigmine** is an anticholinesterase that indirectly increases acetylcholine at the neuromuscular junction, but it is not commonly used for reversing **neuromuscular blockade** due to its widespread muscarinic and nicotinic effects. - It can cause significant side effects like **bradycardia**, **bronchospasm**, and increased secretions, and its efficacy for non-depolarizing blockers is limited. *Rivastigmine* - **Rivastigmine** is an **acetylcholinesterase inhibitor** primarily used in the treatment of **Alzheimer's disease** and Parkinson's disease dementia. - It does not have a role in reversing neuromuscular blockade induced by vecuronium. *Succinylcholine* - **Succinylcholine** is a **depolarizing neuromuscular blocker** itself, causing muscle relaxation rather than reversing it. - It would prolong paralysis rather than reverse the effects of vecuronium.
Question 7: What is the pressure required to open the device shown in the image?
- A. 10–20 cm H₂O
- B. 30–40 cm H₂O (Correct Answer)
- C. 10–20 mm H₂O
- D. 30–40 mm H₂O
Explanation: ***30–40 cm H₂O*** - This pressure range is generally required to open the **Pop-Off Valve** (Pressure Relief Valve) in an Ambu bag (Bag-Valve-Mask) to prevent **barotrauma** to the patient's lungs. - The Pop-Off Valve is a safety feature that vents excess pressure to minimize the risk of **pneumothorax** or other lung injuries during manual ventilation. *10–20 cm H₂O* - This pressure range is typically within the normal ventilatory pressure used for gently inflating the lungs, not specifically for opening the **safety valve**. - While it's a safe pressure for ventilation, it's usually too low to activate the **overpressure relief mechanism** of the Pop-Off Valve. *10–20 mm H₂O* - This unit of millimeters of water (mm H₂O) is incorrect for standard ventilatory pressure measurements in this context; centimeters of water (cm H₂O) is the standard. - Furthermore, the magnitude is too low to represent the pressure required to open a **safety release valve** on a BVM. *30–40 mm H₂O* - Similar to the previous option, the unit of **millimeters of water (mm H₂O)** is not the standard measurement for this type of pressure in respiratory care. - While the numeric value is appropriate for safety valve activation, the ** गलत इकाई ** (wrong unit) makes this option incorrect.