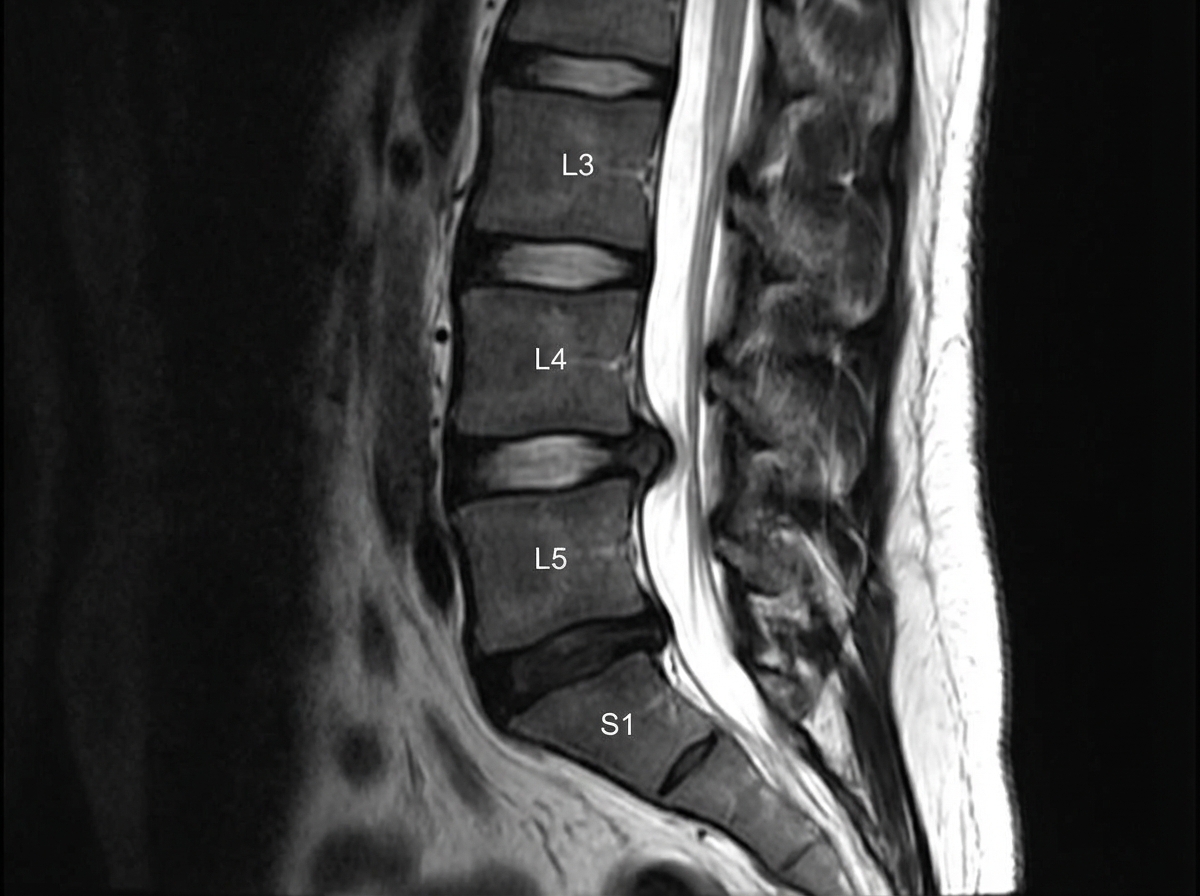
A patient presents with pain in the back of the thigh and leg after lifting heavy weights. Which spinal segment is most likely involved?
Which artery is palpated behind the medial malleolus and in front of the Achilles tendon?
Match the following nerves to their respective areas of supply to the auricle
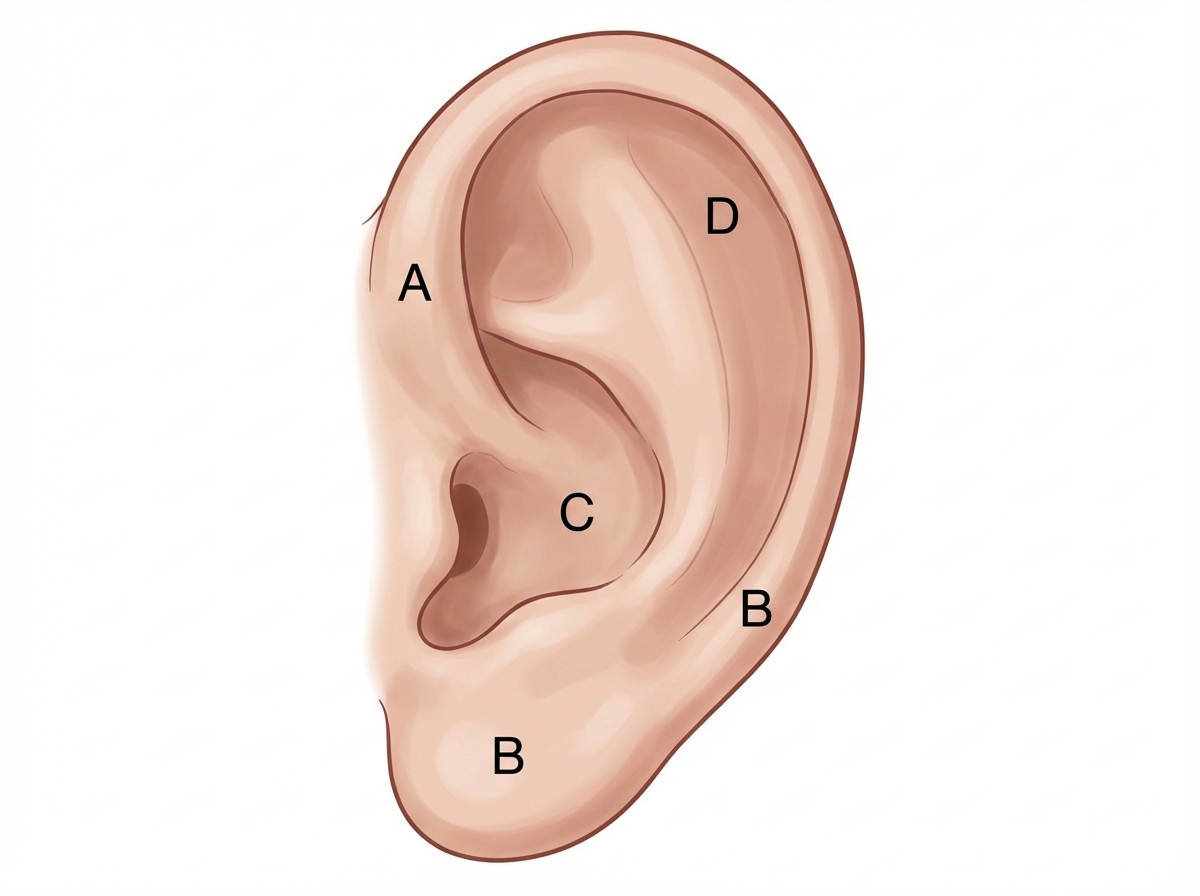
A patient diagnosed with sciatica has tender hamstrings. Which of the following nerves supplies a hybrid muscle that is partially spared in this patient?
What is the most common site of congenital diaphragmatic hernia?
A patient with a nerve injury was asked to form an "O" with their index finger and thumb but was unable to do so. Which muscle is most likely affected?
This type of epithelium is most commonly seen in which of the following organs?
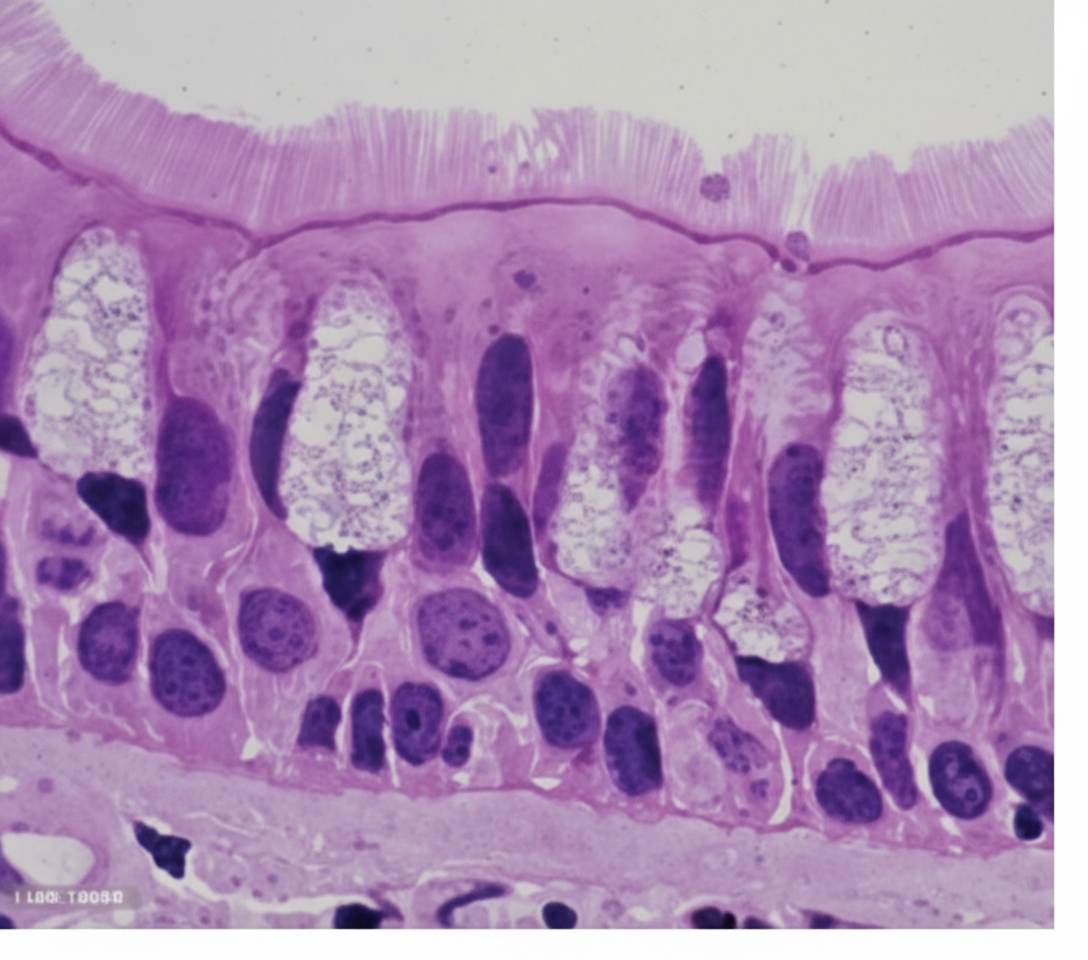
Which tongue papillae do not have taste buds?
Impaired gag reflex is seen due to a lesion in which cranial nerves?
A slipped disc at the level shown in the image would most likely involve which nerve root?