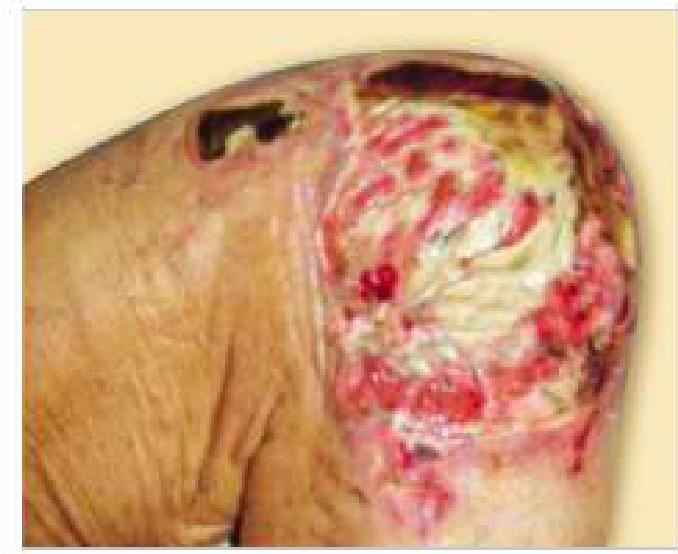
The image below shows a pressure sore. Which stage does this belong to?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A patient presents with an anesthetic patch in areas of the face. Which of the following nerves is the most commonly involved in this condition?
What is the term for a single mutation in a nucleotide base pair that results in a termination codon?
You are working in a primary health center (PHC) situated in a high seismic zone. Which of the following actions should you take as part of preparedness for an emergency?
A patient with diabetes mellitus for the past 5 years presents with vomiting and abdominal pain. She is non-compliant with medication and appears dehydrated. Investigations revealed a blood sugar value of 500 mg/dl and the presence of ketone bodies. What is the next best step in management of this patient?
A farmer presents you with a cauliflower-shaped mass on foot, which developed after a minor injury. Microscopy shows copper penny bodies. What is the most likely diagnosis?
A male child presented with arthralgia and abdominal pain. On examination, there was palpable purpura over the lower limbs. There is a past history of upper respiratory tract infection prior to the onset of presenting symptoms. Which of the following is the treatment for this condition?
A child presents with recurrent chest infections and abdominal pain. There is a history of 1 blood transfusion in the past. On examination, he had icterus and mild splenomegaly. Electrophoresis shows increased HbA2, HbF, and S spike. What is the likely diagnosis?
A woman presenting with symptoms of urinary tract infection was prescribed a drug that causes tendon rupture and arthropathy. What is the mechanism of action of the drug?
A patient comes with a history of asthma and sinusitis. On looking into his medical records, you notice this has been attributed to Samter’s triad. Which drug should be avoided in this patient due to its potential to exacerbate respiratory symptoms?
The image below shows a pressure sore. Which stage does this belong to?
