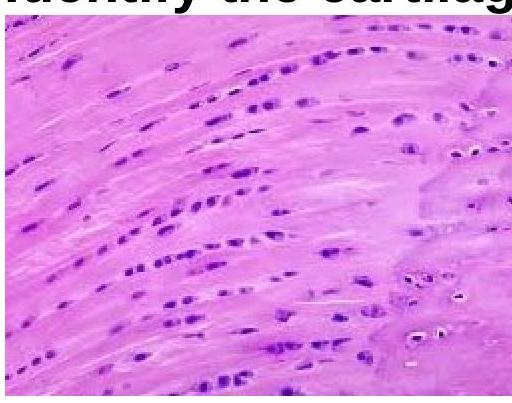
Identify the type of cartilage shown in the image.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Identify the type of cartilage shown in the image.

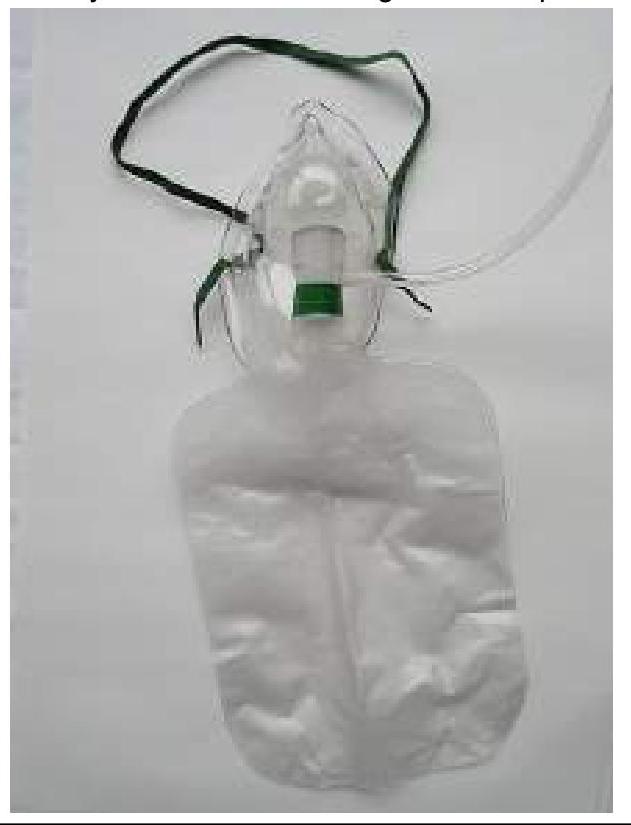
Identify the mask used for patients requiring high concentrations of oxygen.
A patient presents with complaints of hair loss and behavioral changes noted by his wife. Upon examination, the doctor observes a loss of eyebrows. After further assessment, including an examination of the nails, what type of poisoning is suspected in this case?
Which of the following is not seen in MEN 2B syndrome?
A patient presents to you with fever, night sweats, ptosis, and bilateral facial nerve palsy. Investigations showed leukocytosis and bilateral hilar lymphadenopathy. Which of the following is the most likely diagnosis?
Which of the following is NOT an absolute contraindication for the use of an Intra Uterine Contraceptive Device (IUD)?
A 65-year-old male presents with blurred vision and a history of cataract surgery. Upon examination, fluffy white deposits are noted on the anterior lens capsule. What is the most likely diagnosis?
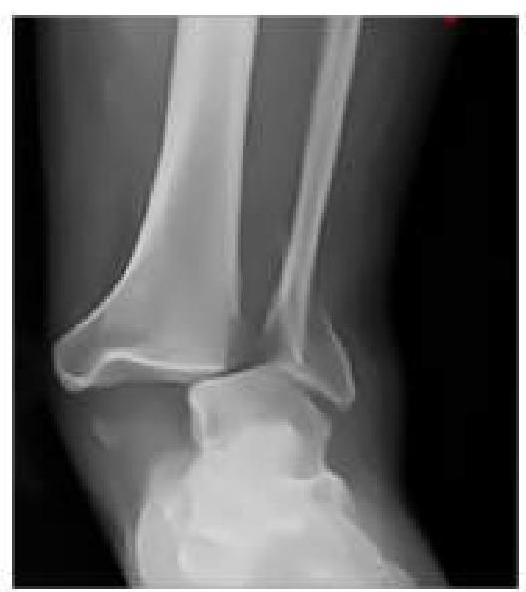
An RTA patient presented to the emergency department with severe pain in the ankle. An X-ray was performed, given below. What is the best next step in management?
An 11-year-old child with a history of streptococcal pharyngitis presents you with fever and arthralgia. There is no past history of rheumatic heart disease or features of carditis or valvular disease. How often is 600,000 IU of benzathine penicillin recommended for prophylaxis of rheumatic heart disease?
A patient presents to the emergency department with a history of ingestion of ten tablets of paracetamol. He has developed oliguria and liver function tests show deranged values. In the context of paracetamol overdose, which of the following can be used in the management of this condition?